Continuing Education Activity
Congenital syphilis (CS) is caused by transmission of the spirochete Treponema pallidum from mother to fetus, resulting in diverse clinical presentations. Congenital syphilis in a fetus is sometimes associated with a full term, seemingly healthy infant but can also be associated with premature birth or stillbirth Rates of CS are increasing, and 2017 had the greatest number of cases since 1997. CS is a nationally notifiable disease, meaning each case in each state must be reported to the Centers for Disease Control (CDC). This activity reviews the clinical presentation, evaluation, and management of congenital syphilis and the role of the interprofessional team in caring for affected patients.
Objectives:
- Explain when congenital syphilis should be suspected.
- Explain how to manage congenital syphilis.
- Explain how to prevent congenital syphilis.
- Explain how an interprofessional approach is imperative to the effective management of congenital syphilis.
Introduction
Congenital syphilis (CS) is caused by transmission of the spirochete Treponema pallidum from the mother to the fetus, resulting in a multitude of clinical presentations ranging from asymptomatic, premature birth, and a wide array of clinical signs and symptoms to stillbirth. Rates for CS are on the rise, with 2017 having the most cases of CS since 1997.[1] CS is a nationally notifiable disease with each case being reported to the CDC by all 50 states.
Etiology
The causative organism of syphilis was first identified by Fritz Schaudinn and Erich Hoffmann in 1905. CS is caused by Treponema pallidum which is a motile spirochete, a helically coiled, corkscrew-shaped bacterium that is 6 to 15 micrometers long and 0.1 to 0.2 micrometers wide.[2] The first recorded outbreak of syphilis was in Europe in 1494 in modern day Italy when the term “French disease” was coined. Treponemes have not yet been cultured in vitro and humans remain the only known host for T. pallidum.[3]
Epidemiology
Researchers estimate that congenital syphilis is a complicating factor in about 1 million pregnancies every year worldwide.[4] CS has a largely contributed toward infant death and has been responsible for 305,000 perinatal deaths worldwide annually.[5] As syphilis remains an easily treatable disease, most cases of CS are seen in women who did not receive proper prenatal care or receive improper treatment. In the United States, the rate of CS was at the highest point at roughly 100 cases per 100,000 live births in 1991 and then declined until 2012 to 334 total annual cases (8.4 cases per 100,000 live births).[6][7] However, since then CS has been on the rise. From 2012 through 2014, the number of reported CS cases in the United States increased from 334 to 458 (8.4 to 11.6 cases per 100,000 live births).[7] The CDC reported 918 cases of CS in the United States in 2017 (23.8 cases per 100,000 births), reaching a 20-year high.[1]
Significant racial disparity is seen in the incidence of CS, and in 2014 the CDC reported that CS was 10 times more prevalent in mothers who were black compared to mothers who were white (38.2 versus 3.7 cases per 100,000 births). They also report a 3-times higher prevalence in black mothers compared to Hispanic mothers (38.2 versus 12.2 cases per 100,000 births).[7] As far as regional distribution of CS is concerned, the incidence in the southern United States is highest, followed by the western United States, then the Midwest, while the lowest incidence is in the Northeastern parts of the United States.[7]
Pathophysiology
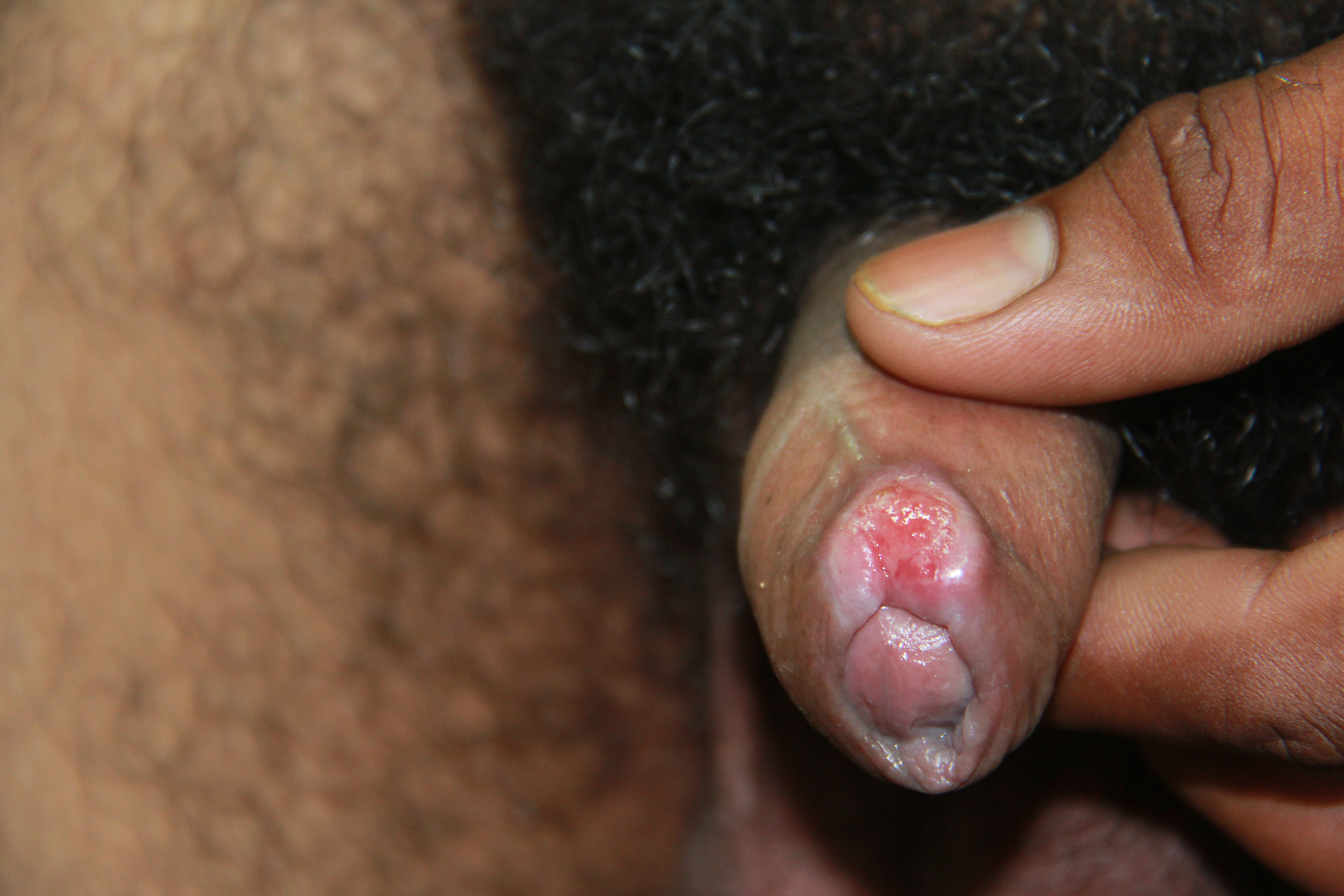
In adults, syphilis initiates an infection after local infiltration through subcutaneous tissues to cause a local immune response and establish an initial ulcerative lesion. However, congenital syphilis differs from syphilis in adults in that T. pallidum is released straight into the bloodstream of the fetus causing spirochetemia with spread to most organs including the bones, kidney, spleen, liver, and heart. This leads to widespread inflammation throughout these organ systems leading to a variety of clinical manifestations.
Histopathology
T. pallidum is 6 to 15 micrometers long and 0.1 to 0.2 micrometers wide.[2] Because of the limited width, it cannot be visualized by direct microscopy and requires darkfield microscopy for visualization.[8] Darkfield microscopy allows visualization of live treponemes that are thin, corkscrew spiral-shaped organisms that may appear to be moving forward and backward.[8] T. pallidum may also be visualized using immunofluorescent staining and special silver stains.[9] These imaging modalities also show the characteristic corkscrew shaped-spiral organism. The placenta may also exhibit signs of enlarged hypercellular villi, proliferative vascular changes, and acute and/or chronic villitis on histologic examination.[10]
History and Physical
Most cases of CS are seen in women without proper prenatal care or in those who receive improper treatment. Syphilis screening is part of routine standard of care in all pregnant women in the United States, and it has shown to decrease rates of CS.[11] Treatment with penicillin in pregnant women with syphilis is 98% effective at preventing CS.[7] While CS can cause severe illness and fetal demise, most neonates born with CS are asymptomatic at birth.[12] However, in untreated infants clinical manifestations usually appear by three months of age and commonly include:
- Hepatomegaly: This is the most common finding and may occur with splenomegaly. Biopsy of the liver followed by darkfield microscopy may reveal the spirochete. Liver function tests may be abnormal.
- Jaundice: Jaundice may or may not be present depending on the extent of liver injury.
- Rhinitis: One of the first clinical presentations, usually in the first week of life. Copious, persistent white discharge is noted, which contains spirochetes that can be visualized under darkfield microscopy.
- Generalized Lymphadenopathy: Generalized, non-tender lymphadenopathy is also a common finding.
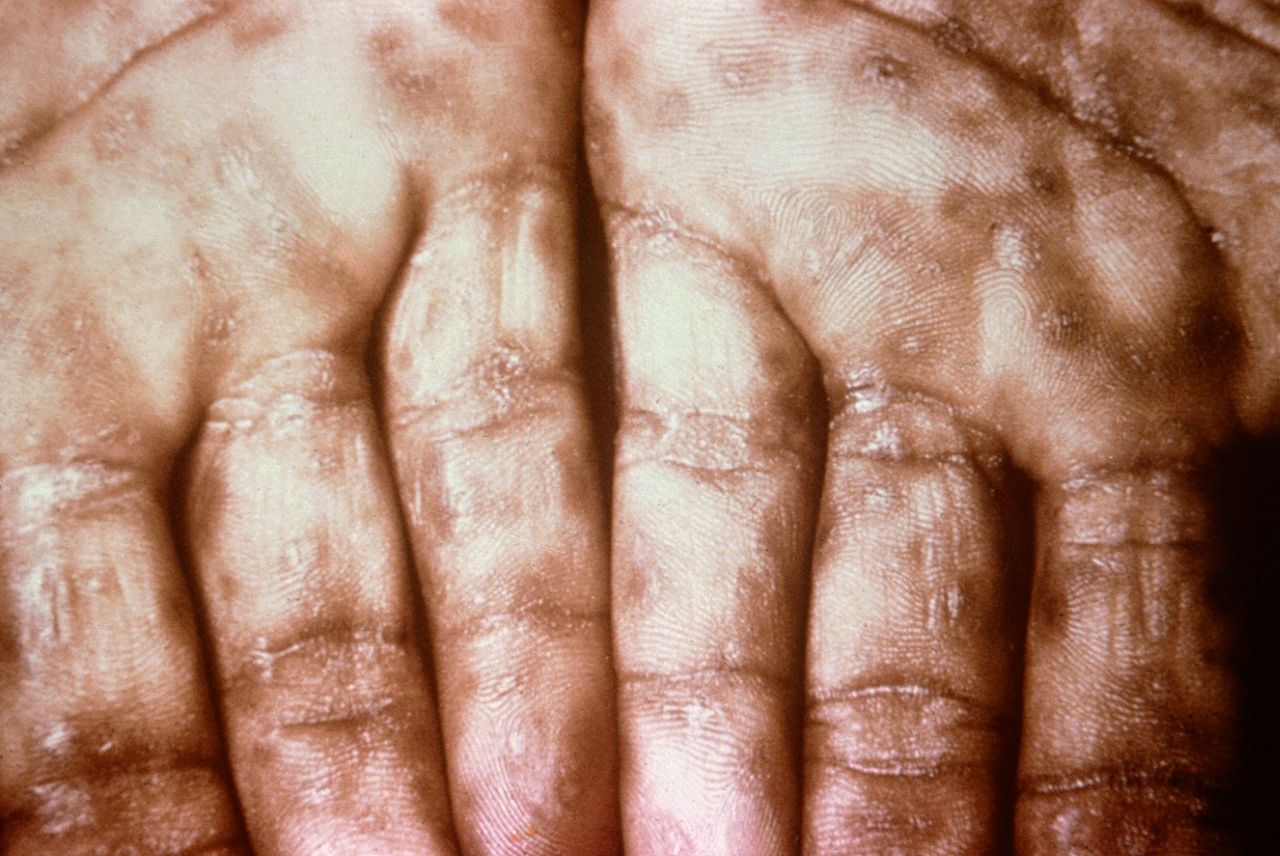
- Rash: Rash usually appears one to two weeks after rhinitis. Small red or pink colored maculopapular lesions may be commonly seen on the back, buttocks, posterior thigh and soles of the feet. The rash progresses to desquamation and crusting.
If there is a failure to diagnose congenital syphilis early, persistent inflammation may lead to scarring and gumma formation.[13] Clinical findings in late CS includes[14][15]:
- Skin and mucous membrane gummas and perioral fissures/scarring
- Facial changes including frontal bossing, saddle nose, prominent maxilla
- Anterior bowing of the shin called saber shins.
- Hutchinson teeth which are hypoplastic notched permanent teeth, most commonly of the upper central incisors
- Intellectual disability and cranial nerve palsies
- Sensorineural hearing loss and changes in vision
- Eye involvement may lead to interstitial keratitis, secondary glaucoma, and corneal scarring
Hutchinson triad (Hutchinson teeth, interstitial keratitis, and sensorineural hearing loss) is relatively specific for congenital syphilis.[15]
Evaluation
Maternal screening for syphilis in early pregnancy is of prime importance in preventing CS, and it is considered the standard of care in the United States. Maternal treatment of syphilis with penicillin is 98% effective at preventing CS.[7]
The following laboratory and radiographic abnormalities can aid in the diagnosis of CS:
- Histologic examination of the placenta and cord for the typical pathological changes and presence of spirochetes
- Darkfield microscopic examination of nasal discharge if present
- Long bone radiographs that may show findings of pathologic fractures, metaphyseal serration, localized demineralization, and osseous destruction.[16]
- Chest x-ray which may show diffuse opacification of both lung fields
- Non-treponemal tests: Venereal Disease Research Laboratory (VDRL) or Rapid Plasma Reagin (RPR)
- Specific treponemal tests: Fluorescent treponemal antibody absorption (FTA-ABS) and/or micro hemagglutination test for antibodies to T.Pallidum (MHA-TP) testing
- CSF abnormalities including reactive CSF VDRL, CSF pleocytosis, elevated CSF protein
- CSF PCR for detection of treponemal DNA
Initial workup for an infant born to a woman with reactive non-treponemal and treponemal testing should follow the recommendations of the CDC[17] or American Academy of Pediatrics as listed in Red Book (Red Book: 2015 Report of the Committee on Infectious Diseases, 30th ed, Kimberlin DW (Ed), American Academy of Pediatrics, Elk Grove Village, IL 2015. p.755.)
Treatment / Management
Treatment for congenital syphilis when the disease is confirmed or likely to be present is:
- Infants up to 4 weeks of age: Aqueous crystalline penicillin G, 50,000 units/kg per dose intravenously every 12 hours in the first seven days of life. After 7 days of life, 50,000 units/kg per dose intravenously (IV) every 8 hours for 10 to 14 days. Alternatively, procaine penicillin G, 50,000 units/kg/day intramuscularly for 10 to 14 days.[18]
- Infants older than 4 weeks and older children: Aqueous penicillin G, 50,000 units/kg per dose every 6 hours intravenously for 10 to 14 days.[18]
The management of an asymptomatic infant potentially exposed to syphilis but unlikely to have the disease is controversial. These are infants of mothers who received adequate treatment more than 4 weeks before delivery. However, most experts and the CDC recommends benzathine penicillin G 50,000 units/kg per dose intramuscularly (IM) in a single dose in these asymptomatic children.[18]
Differential Diagnosis
Congenital syphilis may present similarly to other disease processes which should also be considered by the clinician. These include neonatal sepsis especially given the pneumonia-like chest x-ray findings in CS. Other considerations include TORCH infections including Toxoplasmosis, Rubella, Cytomegalovirus, herpes simplex virus. Neonatal hepatitis should also be considered given hepatomegaly and elevated LFTs. Co-infections with HIV should also be considered.
Prognosis
Excellent prognosis if diagnosed and treated appropriately in a timely fashion. Syphilis is easily treated with penicillin. However, there is an increased risk for worse outcomes and possible death in:
- Premature infants
- Those who have a delay or do not receive proper treatment
- Patients who display an extensive spread of the disease with multiple organ failure
- Infants with a severe Jarisch-Herxheimer reaction upon treatment
Complications
Delayed diagnosis and treatment can lead to late, persistent clinical features of intellectual disability, skin gummas, scarring, hearing deficits and skeletal abnormalities. Initiation of treatment in some infants can lead to a Jarisch–Herxheimer reaction leading to fevers, chills, hypotension, and possibly fetal death as a result of an inflammatory response to the dying spirochetes.
Consultations
Consultation with a pediatric infectious disease specialist will be very helpful in the workup, diagnosis, and management of patients with CS.
Deterrence and Patient Education
The surveillance of all pregnant women for syphilis and timely treatment of the disease during pregnancy is the most effective means of eliminating CS. The following are considerations that may lead to decreased rates of congenital syphilis.
- Expansion of basic prenatal care to all pregnant women for early detection of syphilis in pregnancy
- Education on safe sexual practices and the use of condoms to decrease the spread of syphilis
- Expansion of free STD clinics for early diagnosis and treatment
Enhancing Healthcare Team Outcomes
Congenital syphilis is a serious infection with potential for long-term complications. In the United States, each CS case must result in notification to the public health department. Besides adequate treatment of both the infant and the mother, sexual partners of the mother need to be tested and adequately treated. The treatment of CS involves a team approach including infectious disease, neonatology, pediatrics, obstetrics, and nursing staff. Infectious disease specialists, pediatricians, and neonatologists are usually involved in the acute treatment of the disease. Pediatricians also have the task of following up on successful eradication of the disease and monitoring for disease complications. Obstetricians have the important task of testing pregnant women for syphilis and treating syphilis in pregnancy which significantly decreases the incidence of CS.
The US Preventative Services Task Force (USPSTF) is an independent panel of national disease prevention and evidence-based medicine experts. The task force improves the health of all Americans by making evidence-based recommendations about clinical preventive services. USPSTF developed the current guidelines after an exhaustive review of current medical literature. A recent Cochrane review performed by USPSTF concluded Level A recommendation (high certainty of substantial net benefit) for screening for syphilis in pregnancy as well as screening for syphilis in high-risk individuals.[19][20] Given the strong level of evidence, physicians should strongly follow these guidelines across the country.