Continuing Education Activity
Xerostomia is defined as the sensation of oral dryness. Patients usually report mouth dryness, oral burning, swallowing difficulty, and decreased or altered taste. There are numerous causes of xerostomia; the most common cause is medication side effects, followed by Sjogren syndrome (SS) and radiotherapy and other autoimmune diseases in no particular order. Numerous etiologies have been described, but xerostomia mainly presents as a medication side effect, secondary to head and neck radiation therapy, and associated with Sjögren syndrome. This activity outlines the etiology, pathophysiology, evaluation, and treatment of xerostomia and highlights the role of the interprofessional team to aid in managing patients with xerostomia.
Objectives:
- Review the etiology of xerostomia.
- Explain the pathophysiology of xerostomia.
- Describe the history and physical findings of the patient with xerostomia and the evaluation.
- Describe the management of patients with xerostomia.
Introduction
Xerostomia refers to the sensation of oral dryness, which can result from diminished saliva production.[1] But, patients may report dry mouth even in the absence of a measurable decrease in saliva quantity.[1] A lack of normal salivary flow may lead to complaints of mouth dryness, oral burning, swallowing difficulty, and loss or decreased taste.[2]
Numerous etiologies have been described, but xerostomia mainly presents as a medication side effect, secondary to head and neck radiation therapy, and associated with Sjögren syndrome. Irrespective of a specific etiology, the patient's primary complaint is dry mouth. The treatment aims to alleviate symptoms, but a complete resolution is not always achieved. Initial management includes patient education, like regular water sipping and avoiding tobacco smoking, and local measures, such as artificial saliva [3]. Pharmacological therapy, mainly with pilocarpine [4], is implemented when local efforts are unsuccessful.
Etiology
Xerostomia is linked to multiple etiologies. However, it most frequently develops as an adverse effect of medication, secondary to head and neck radiation therapy, and due to Sjogren syndrome. A wide variety of drugs have the potential to affect salivary gland function and induce oral dryness, which is dependent on the dose and the number of drugs being taken.[5] This may explain why oral dryness is a common complaint in the geriatric population, likely due to the higher use of medications and incidence of comorbid conditions.
Multiple classes of drugs show a correlation with xerostomia.[1] Medications with a reported incidence of xerostomia of 10% or more include but are not limited to:
- Anticholinergic agents: atropine, belladonna, oxybutynin
- Antidepressant and antipsychotic agents: citalopram, haloperidol, phenelzine
- Diuretics: furosemide, chlorothiazide, hydrochlorothiazide
- Antihypertensive agents: captopril, lisinopril, enalapril
- Sedative and anxiolytic agents: alprazolam, diazepam, triazolam
- Muscle relaxants: tizanidine, cyclobenzaprine, orphenadrine
- Analgesic agents: opioids and NSAIDs
- Antihistamines: astemizole, loratadine, brompheniramine
Xerostomia develops in most patients undergoing head and neck radiation therapy for cancer treatment when the major salivary glands are in the radiation path.[3] Salivary flow usually decreases about 50% to 60% when 25 to 30 Gy of standard fractionated radiotherapy has been applied during the first week, reaching its lowest point after two to three weeks.[6] The reduction seen in salivary function depends on the amount of salivary gland tissue contained in the radiation area and the dose.[3] Unfortunately, pre-radiation salivary flow levels are not usually regained.[3] Eisbruch et al. found that in parotid mean radiation doses of more than 24 to 26 Gy, recovery was unlikely; doses under this level were associated with a higher chance of significant recovery.[7]
Xerostomia is commonly attributed to Sjögren syndrome, characterized by oral and ocular dryness [1]. Chronic lymphocytic infiltration causes eventual fibrosis of salivary glands. The condition is more common in women more than 40 years of age. It is unusual for Sjogren to present after the age of 65, and dry mouth after this age is more commonly attributable to age-related exocrine atrophy. In primary Sjögren syndrome, the condition is limited to the salivary glands and eyes. Secondary Sjögren syndrome is also associated with an autoimmune (rheumatoid arthritis) or connective tissue disease.[1]
Other potential causes for oral dryness may include autoimmune system disorders such as systemic lupus erythematosus (SLE), rheumatoid arthritis (RA), thyroid disease, and primary biliary cirrhosis (PBC), patients with a history of mouth breathing, dehydration, poorly controlled diabetes mellitus, nerve damage from head or neck injury, end-stage renal disease (ESRD), graft versus host disease (GVHD), and HIV/AIDS.[8]
Epidemiology
Data regarding the sex predominance of xerostomia vary. In 1996, a statistically significant study in Sweden concluded that 21.3% of men and 27.3% of women reported xerostomia.[9] According to a study in 2006, the prevalence of xerostomia ranged from 0.9% to 64.8%. The majority of data collected for these studies was in Scandinavia (most patients aged over 50, the rest were over 18).[10] In contrast, 100% of patients who received radiation for head and neck cancer or were diagnosed with Sjogren syndrome complained of xerostomia. The prevalence of xerostomia is increasing due to the increasing aging population.[11] Age by itself is not a cause of xerostomia, but older patients tend to be on multiple medications and have a higher incidence of comorbid conditions.
Pathophysiology
Histologically, major salivary glands are made up of salivary acini and ducts, which produce two types of fluids, serous and mucinous. All major and minor salivary glands have nerve supplies, and upon stimulation, salivatory nuclei in the medulla generate an efferent response. The efferent nerve impulses release acetylcholine (ACh), which works on muscarinic receptors (specifically M3 receptors), stimulating salivary glands to produce saliva. The stimuli that cause salivary production ranges from smelling to chewing. Pathology arises when there is a dysfunction in gland innervation or in the gland itself.
Medication-Induced Xerostomia
Xerostomia-inducing medications may exert their effect on the central nervous system (CNS) or at the neuroglandular junction.[5] The secretory cells of the salivary glands receive nerve supply from muscarinic M1 and M3 receptors, alpha1 and beta1-adrenergic receptors, and specific peptidergic receptors that initiate salivary secretion.[5] Medication-induced xerostomia is caused when a medication directly suppresses the CNS from producing ACh or occupies the muscarinic/adrenergic receptors.[5]
Radiation-Induced Xerostomia
Radiation causes xerostomia because the oral cavity, lymph nodes, and salivary glands are in the radiation field of head and neck radiation therapy. Radiation causes quantitative and qualitative changes in the salivary glands [3]. Serous acini, mostly found in the parotid glands, are the main producers of stimulated saliva and are more susceptible to radiation injury.[3] The saliva thickens, becomes more sticky, and decreases during important functions, like mastication.[3]
Although the tissues of salivary glands have a low mitotic index which should make them quite stable and typically radiation-resistant, studies have shown a decline in salivary gland function proportional to the radiation dose. This dose-dependent radiation causes a secretory dysfunction of the gland. Acinar atrophy and chronic inflammation are considered hallmarks of radiation-induced xerostomia. Fibrosis mainly presents as periductal and intralobular, but the structure of the ducts remains intact.
Sjögren Syndrome
In Sjögren syndrome, chronic lymphocytic infiltration and inflammation of acinar cells lead to exocrine fibrosis resulting in gland damage.[12] Only CD4+ lymphocytes were believed to be involved in the pathophysiology of Sjögren syndrome. However, new data also suggests the involvement of B-cells.[13] The presence of anti-SSA (Ro) or anti-SSB (La) antibodies can help diagnose disease. Salivary gland dysfunction seen in Sjögren syndrome has also been linked to an inhibition of nerve stimuli.[1] The decrease in saliva secretion may affect the minor salivary glands first, initiating the symptoms of oral dryness.[1]
History and Physical
Patients with xerostomia, regardless of the etiology, usually report the following symptoms:
- A sensation of oral dryness
- Oral burning or soreness
- Diminished or altered taste
- The need to sip water when swallowing, for which patients usually carry a water bottle at all times
- Difficulty swallowing dry foods, e.g., crackers
- A sensation of thickened saliva
- Sensitivity to acidic or spicy foods
- Loss of appetite and weight loss[1][3]
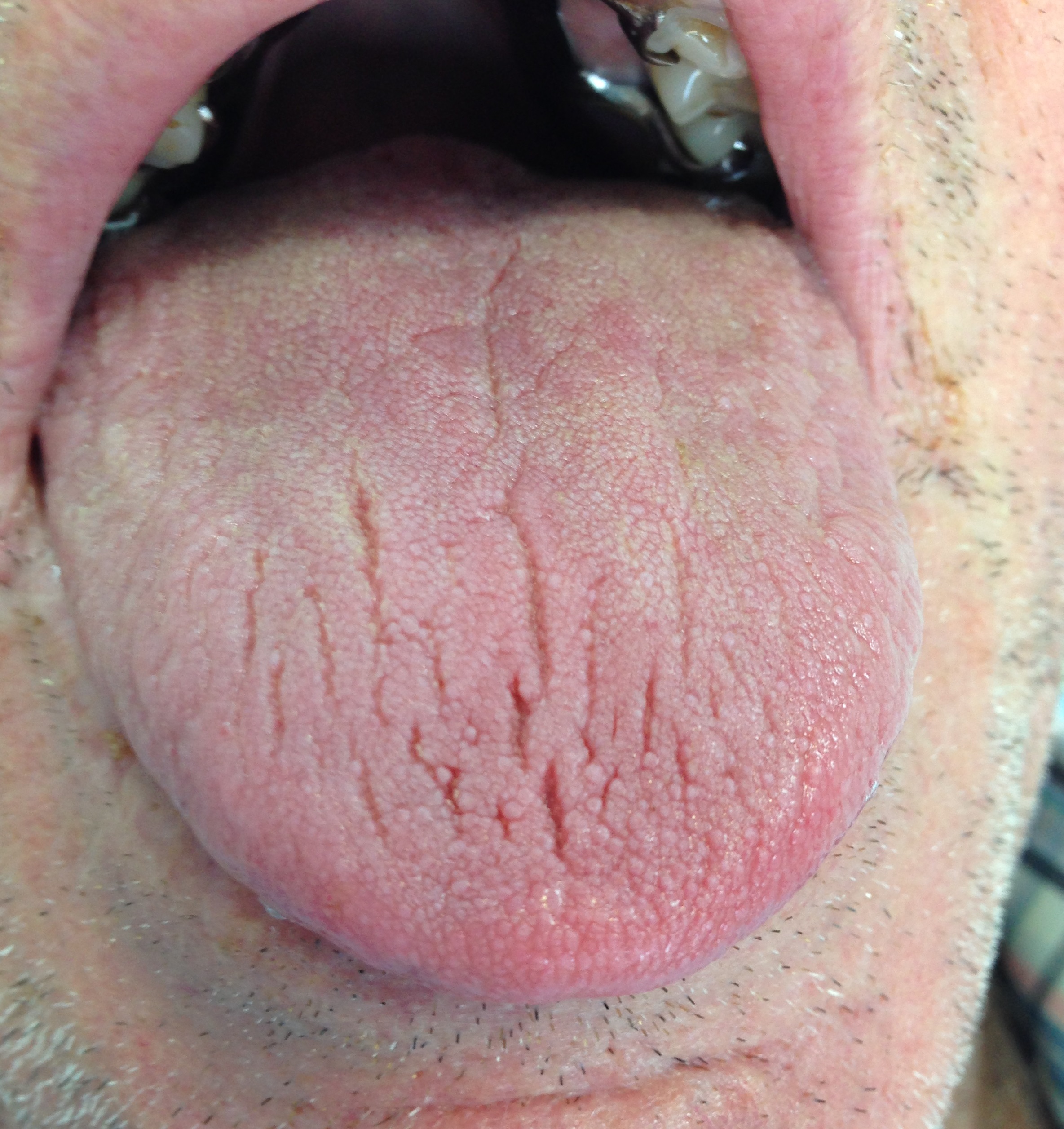
Clinical examination findings may include:
- Fissured tongue and lips
- Filiform papillae atrophy
- Erythematous and parched oral mucosa
- The finger may adhere to the oral mucosa during palpation[1][3]
- Evident lack of saliva on the floor of the mouth[14]
A decrease in salivary production makes the oral cavity more susceptible to dental caries - particularly cervical caries - periodontal disease, halitosis, and candidiasis. Patients using dentures also report loss of retention and denture discomfort. Patients with xerostomia associated with Sjögren syndrome may initially complain of dry eyes and parotid gland enlargement before oral symptoms occur.[1]
Evaluation
Xerostomia is a clinical diagnosis primarily based on history and physical examination. It is estimated that salivary secretion needs to be decreased by half before xerostomia is evident.[1] Patients' subjective symptoms of oral dryness should be sufficient to establish a diagnosis of xerostomia and start treatment, as there may not be a measurable reduction in salivary flow initially.[1] Because so many drugs carry associations with xerostomia, checking the patient's medication list is imperative.
If needed, there are numerous techniques employed to evaluate hyposalivation, such as:
- Sialometry: The normal stimulated salivary flow rate is between 1.5 to 2.0 mL/min, while the unstimulated flow rate ranges from 0.3 to 0.4 mL/min.[4] A diagnosis of hyposalivation is if stimulated salivary flow is less than 0.5 to 0.7 mL/min or unstimulated flow of under 0.1 mL/min.[4]
- Sialography: An imaging technique that can be used to identify salivary stones or masses.[15] Three-dimensional (3D) MR sialography looks to be a promising diagnostic approach in patients with radiation exposure as the salivary gland flow can be visualized.[16] A small trial on 3D MR sialography in pre and post-radiation patients has shown promise. Imaging performed at six weeks pre-radiation and six months post-radiation showed a decrease in salivary flow.
- Biopsy: If a systemic cause such as sarcoidosis, amyloidosis, or a salivary mass is suspected, a biopsy of a salivary gland may be necessary. Further management then depends on biopsy results.
In secondary Sjögren syndrome, patients exhibit further signs and symptoms of an autoimmune or connective tissue disease such as rheumatoid arthritis or systemic lupus erythematosus.[1] Laboratory tests may show abnormalities such as raised erythrocyte sedimentation rate (ESR), anemia, leukopenia, and rheumatoid factor or autoantibodies.[1] A lip biopsy usually reveals focal lymphocytes infiltrating the minor salivary glands.[17]
Treatment / Management
The main goal of management is symptomatic relief. The underlying cause should be treated whenever possible, e.g., treating nasal congestion to avoid mouth breathing. If xerostomia is medication-induced, stopping or swapping to one with less xerostomic effects should be considered.[14] Xerostomia is initially treated by educating the patients on lifestyle habits that help decrease symptoms and local measures. If these deem unsuccessful, a pharmacological treatment could be established.
Patient Education
- Frequent sipping of water
- Chewing sugar-free gum
- Sucking on sugar-free candy
- Avoiding caffeine, tobacco, alcohol, and dry or hard-to-chew foods
- Correcting dehydration by increasing fluid intake
- Regular oral hygiene and dental care
Local Measures
Artificial saliva in dose forms such as sprays, lozenges, and gels may be indicated before meals and as needed. The disadvantages of saliva substitute products are that they do not work reliably, the duration of action is limited, they have an unpleasant taste, and carry a high monetary cost. Despite this, they are helpful for special times, like during a flight or bedtime.[3]
Pharmacological Treatment
The sialogogue drugs pilocarpine and cevimeline are FDA-approved medications for managing xerostomia.[4] Both medications work on muscarinic receptors and stimulate salivation. Pilocarpine is given orally with normal dosing of 5 to 10 mg three times a day.[18] The cevimeline dose is 30 mg three times a day. Either agent is tried for up to three months to ascertain efficacy. These medications require some residual salivary gland function to be effective as they stimulate the patent gland to secrete saliva.
The most prevalent adverse effects of pilocarpine include sweating, nausea, and rhinitis.[3] Treatment with cevimeline is also linked to increased sweating.[3]
The application of topical physostigmine has also been a therapy option in treating xerostomia. Physostigmine is a cholinesterase inhibitor, thus increasing the amount of acetylcholine available to stimulate salivary glands. It increases the production of saliva by stimulating mucin-producing glands. A gel containing 1.8 mg of physostigmine may provide relief for about two hours.[19]
Malic acid has demonstrated some benefits if xerostomia is drug-induced.[14] Anethole trithionate (cholagogue-bile secretion stimulant) is another drug that has proven beneficial for xerostomia.[20]
Other Measures
Electrical stimulation has been shown to improve salivary flow, but these intraoral devices are not practical for everyday use. Patients undergoing radiation to the head and neck area may benefit from amifostine.
Differential Diagnosis
Patients presenting with a primary complaint of dry mouth should be evaluated for various conditions known for causing sicca symptoms. These conditions include primary Sjögren syndrome, idiopathic sicca syndrome, other autoimmune diseases, and drug-induced sicca syndrome.[21] Other disorders might need to be ruled out and require separate specific management. These include sarcoidosis, granulomatosis with polyangiitis, IgG4-related disease, chronic hepatitis C (HCV) or HIV, GVHD, ESRD, and head and neck radiation therapy.[21]
Prognosis
The underlying cause of dry mouth determines prognosis. Almost all patients will benefit from symptomatic treatment. Providers can address a temporary etiology such as dehydration, medication-induced salivary hypofunction, and use of substances such as caffeine, smoking, and alcohol with good results. The symptoms tend to be persistent for chronic and irreversible causes such as Sjögren syndrome and head and neck cancer post-irradiation, where palliative treatment is the only alternative.
Complications
Saliva provides lubrication and keeps the oral cavity moist and clean, protecting the oral mucosa from mechanical injury. Salivary amylase helps to initiate the digestive process. Mucin and immunoglobulin in saliva protect the oral mucosa from microbial infection. Therefore, xerostomia can adversely affect oral intake leading to poor nutrition, gingivitis and periodontitis, dental caries, halitosis, fungal infections (candidiasis), and accelerating enamel erosion. Chronic discomfort from dry mouth can contribute to symptoms of anxiety and depression.
Deterrence and Patient Education
Patients should be encouraged to openly communicate with providers if they have any symptoms of dry mouth or halitosis. Patients should be encouraged to try preventative measures, which include and are not limited to:
- Sipping water
- Chewing gum (preferably sugar-free)
- Using a mouth humidifier
- Reducing the consumption of alcohol, coffee, tobacco, sugary drinks, and candy
- Keeping cracked mucosal areas moist
Patients should also be encouraged to regularly follow up with their dentist, incorporate flossing, and use fluoride toothpaste. Providing appropriate therapy in time will help patients with their mental health, decrease anxiety and depression, and maintain a better quality of life.[22]
Enhancing Healthcare Team Outcomes
Xerostomia has many causes, including medications and radiation. Despite being a common disorder, its diagnosis usually gets delayed, and the treatment is not satisfactory. For this reason, an interprofessional team is the best management strategy.
Xerostomia is a clinical diagnosis primarily based on history and physical examination.[22] It is crucial that healthcare professional reviews the patient's medication list. Anti-hypertensives, Parkinson drugs, diuretics, and many others have implications as a cause of xerostomia. If a medication is the suspected cause and alteration of regimen is straightforward, it should merit consideration. A pharmacy consult is often necessary to discuss alternative regimens and avoid drug-drug interactions.
Patients with Sjögren disease usually have poor results with present-day treatments. The constant dry mouth also leads to dental cavities and a poor quality of life. The dentist and rheumatologist should be involved in the care of these complex patients and report their findings back to the entire interprofessional healthcare team.
The primary care providers, specialists, nurses, and pharmacists should provide interprofessional education to the patient regarding hydration and avoid triggers like tobacco, coffee, alcohol, and dry or hard-to-chew foods. If medications are involved in treatment, the pharmacist should verify all dosing, perform medication reconciliation, and report any concerns to the nursing staff, informing the treating physicians. Nursing staff can check progress or lack thereof in treatment and report therapy and lifestyle compliance to the team.
Finally, patients should be aware that several intra-oral appliances and electrical therapies are available, but none of these work reliably, and most have not had testing in clinical trials. The patient needs to speak to a clinician before investing in these therapies.
Because of the wide variety of xerostomia etiologies, the condition requires an interprofessional team approach, including physicians, specialists, dentists, specialty-trained nurses, and pharmacists, all collaborating across disciplines to achieve optimal patient results. [Level 5]