Introduction
Appendectomy is among the most commonly performed surgical procedures.[1] The most common indication for appendectomy is acute appendicitis. The lifetime risk of acute appendicitis ranges from 9% to 10%.[2] Acute appendicitis most commonly occurs between the ages of 10 and 20 years.[3]
Appendicitis is called the first American surgical disease, and appendectomy holds a prominent and storied position in surgical history. Charles McBurney published his report on the surgical management of appendicitis in 1895. He described the potential consequences of undrained purulent appendicitis, the disadvantages of the classical midline laparotomy, and exploratory needle puncture. Finally, he described a novel surgical approach and exposure, introducing consecutive lateral incisions through the external oblique aponeurosis, internal oblique, and transversus abdominis muscles rather than midline laparotomy.[4]
Appendectomy was the first laparotomy performed with a source control approach to eradicate an infectious threat.[5] Since appendicitis was first described over a century ago, appendectomy remains the gold standard of treatment.[6] Today, the inflamed appendix can be surgically removed using either an open approach or the laparoscopic appendectomy method first described by Semm in 1983.
Despite a significant change in managing acute appendicitis with primary antibiotic therapy, the primary option for treating acute appendicitis remains a surgical approach. A large, randomized trial of antibiotic therapy for the primary management of acute appendicitis showed that while antibiotic therapy might have comparable results with appendectomy in the short term, 1 of 4 participants in the antibiotic therapy arm required appendectomy within one year.[7]
Anatomy and Physiology
Register For Free And Read The Full Article
Search engine and full access to all medical articles
10 free questions in your specialty
Free CME/CE Activities
Free daily question in your email
Save favorite articles to your dashboard
Emails offering discounts
Learn more about a Subscription to StatPearls Point-of-Care
Anatomy and Physiology
The vermiform appendix is a small, tubular, blind-ended hollow outpouching attached to the posteromedial wall of the cecum, typically 1.7 cm below the ileocecal valve. The base of the appendix arises from the convergence of the taeniae coli, making this point of convergence a useful surgical landmark. The human appendix is typically 8 to 10 cm long in adults and is considered a vestigial organ.[8]
The appendix is anterior to the lumbar plexus and iliopsoas muscle and posterior to the greater omentum. It is attached to the terminal ileum by the mesoappendix, a triangular fold of mesentery that is also connected to the cecum. The shorter length of the mesoappendix than the appendix gives the appendix its distinct curled, twisted appearance.
Typically, the appendix is located in the right lower quadrant of the abdomen. However, it may also be found in the left upper quadrant, left anterior para-midline, and lower midline. It may also be positioned in several other orientations, such as the pelvic, where it points towards the psoas muscle and hangs over the pelvic brim; sub-cecal, where it is in the iliac fossa and inferior to the cecum; retro-ileal, where it lies posterior to the ileum; and pre-ileal, where it is anterior to the ileum.[9]
The appendix is supplied by the appendicular artery, which arises from the ileocolic artery in 35% of patients. However, the origin of the appendiceal artery is anomalous, and it may arise from the posterior cecal (13%), anterior cecal (4.25%), medial branch of the ileocolic (8.25%), or ileal artery (4.25%).[9]
Indications
Diagnosing Acute Appendicitis
When evaluating a patient with suspected acute appendicitis, the medical history, physical examination, laboratory findings, and pertinent diagnostic imaging should be holistically reviewed. Several scoring systems have been designed using these diagnostic pillars to aid in timely decision-making and select the patient population requiring appendectomy. The Alvarado scoring system is a practical tool used to diagnose acute appendicitis and can help reduce the incidence of unnecessary surgery. Still, it is not considered a highly-sensitive measure and should not be used in isolation.[10] An Alvarado score of 7 or greater has a positive predictive value for acute appendicitis, ranging from 78% to 96%.[11]
Appendectomy is indicated in several circumstances; the specific considerations for commonly encountered clinical situations are briefly discussed below.[9]
Uncomplicated Appendicitis
Appendectomy is indicated in patients with a history, physical examination, and laboratory and imaging findings consistent with acute uncomplicated appendicitis. Uncomplicated or simple appendicitis is defined as an inflamed appendix without evidence of necrosis or perforation.[2] In most cases of acute appendicitis, the appendix is not perforated at the time of presentation.
The efficacy of antibiotics as the primary treatment for acute uncomplicated appendicitis has been extensively researched, yielding mixed and contradictory results and conclusions.[12][13][14] Adverse events, including the incidence of 30-day postintervention peritonitis, were higher in the antibiotic therapy arm of one trial. However, other trials support the feasibility of antibiotic therapy alone despite the cumulative incidence of appendicitis recurrence for uncomplicated acute appendicitis.[15]
Although the Comparison of Outcomes of Antibiotic Drugs and Appendectomy (CODA) trial offers the option of using antibiotics alone to manage acute appendicitis, it is imperative to exercise caution when considering this approach. Several outcomes of this approach remain uncertain, including the potential of missed malignancies, cases of recurrent appendicitis, and the long-term efficacy of this method.[16]
The Prospective Observational Study on Acute Appendicitis Worldwide (POSAW), an international collaborative study, has confirmed that surgical management remains the main effective option for treating appendicitis.[7][17] Despite the availability of alternative therapeutic approaches with primary antibiotic therapy, appendectomy remains the standard practice for treating acute uncomplicated appendicitis.[18]
Complicated Appendicitis
Complicated appendicitis is characterized by a peri-appendiceal abscess or phlegmon.[19]
One of two approaches is used in treating complicated appendicitis, operative or nonoperative. The operative approach is an immediate surgical procedure, and the nonoperative approach is initial conservative management followed by a surgical procedure.
The effectiveness of immediate versus delayed appendectomy in managing complicated appendicitis remains unclear. The evidence suggests that immediate open procedures may lead to a longer hospital stay and more time away from regular activities; the quality of this evidence is very low. Similarly, the evidence supporting improved health-related quality of life following immediate laparoscopic appendectomy is of very low quality. Therefore, the limited data makes it impossible to determine whether early or delayed appendectomy has significant benefits or harms.
Immediate surgery should be avoided in patients with phlegmon, abscesses, or prolonged symptoms, as these patients will likely have significant inflammation and dense adhesions, which are associated with higher morbidity.[20] For septic or unstable patients, however, immediate surgery may be necessary; this approach may lead to increased complications due to adhesions and inflammation. To avoid these issues, a staged management protocol is typically attempted. Patients should receive intravenous antibiotics, resuscitation, and for those with persistent infection, percutaneous image-guided drainage. This approach boasts a success rate of 79%, particularly for those with lower-grade abscesses or those who receive transgluteal or CT-guided drainage instead of ultrasound-guided drainage. Single-stage surgical intervention is employed if nonoperative management fails or free intraperitoneal perforation is present.[21][22][23] An immediate appendectomy is indicated if the peri-appendiceal abscess cannot be drained percutaneously.
An emergent appendectomy may be required in cases of perforated appendicitis if there is resulting sepsis or instability, as a rescue appendectomy if initial nonoperative management with antibiotics or percutaneous drainage failed, or immediately if the appendiceal abscess is small or if the abscess is large and inaccessible for percutaneous drainage.[24]
Subcategorizing complicated appendicitis into the following stages can assist with management decisions: gangrenous nonperforated appendicitis, perforated appendicitis with local contamination, perforated appendicitis with periappendiceal phlegmon or abscess, and perforated appendicitis with generalized peritonitis.[25]
Laparoscopic appendectomy is indicated in gangrenous non-perforated appendicitis and perforated appendicitis with local contamination.[26][27] When feasible, laparoscopic appendectomy is indicated in patients with perforated appendicitis with generalized peritonitis. Initial or definitive nonoperative treatment is indicated in patients with a perforated appendix with periappendiceal phlegmon or abscess.[28]
Acute Appendicitis in Patients with Crohn Disease
Patients with Crohn disease are at significant risk of entero-enteric fistulas. However, less than 2% of all patients presenting with acute appendicitis are later diagnosed with Crohn disease. Therefore, in patients with an established diagnosis of Crohn disease without cecal involvement and evidence of acute appendicitis, appendectomy is indicated.[29][30][31][32][33][34]
Appendiceal Neoplasms
Appendiceal neoplasms are present in approximately 1% of all appendectomy specimens. However, the exact incidence of these neoplasms is unknown. The classification of appendiceal neoplasms can be complicated, but they typically are classified into four subtypes: colonic-type adenocarcinoma, mucinous neoplasm, goblet cell carcinoma, and neuroendocrine neoplasms.
It is crucial to note that any appendiceal tumor can present as acute appendicitis, making the preoperative diagnosis uncertain. Therefore, the definitive histopathological diagnosis, classification, and the need for additional therapies and surgeries are determined only after the appendectomy. The indications for appendectomy remain similar to non-neoplastic conditions and should be decided according to the physical examination, laboratory, and imaging findings present at the initial presentation.[9]
Contraindications
Contraindications to appendectomy in acute appendicitis include the following:
- Inability to tolerate general anesthesia
- Inability to tolerate the pneumoperitoneum of a laparoscopic method
- Uncorrectable coagulopathy
Incidental appendectomy is contraindicated under the following conditions:
- Patients with unstable hemodynamics
- Patients with an established diagnosis of Crohn disease
- Patients with a predetermined plan for radiation treatment.[35]
Equipment
Open Appendectomy
- Scalpel (11 or 15 blade) and forceps
- Atraumatic graspers and electrocautery, retractors
- Absorbable sutures and needle drivers [36]
Laparoscopic Appendectomy
- One laparoscopic monitor
- One laparoscope (5 or 10 mm, 0 or 30 degrees), including the light source and camera cord
- Veress needle or Hasson trocar, carbon dioxide source, and tubing for insufflation
- Standard laparoscopy instrument tray and endoscopic retrieval bag[20]
- Trocars (on average: two 5 mm working trocars and one 10 to 12 mm trocar)
- Scalpel (11 or 15 blade), needle driver, forceps, and absorbable sutures
- Open major abdominal tray for possible conversion to open appendectomy[37]
Personnel
Open and Laparoscopic Procedures
- Operating surgeon
- Surgical first assistant
- Surgical technician or operating room nurse
- Circulator or operating room nurse
- General anesthesia personnel
Preparation
Prophylactic Antibiotic Therapy
Administration of prophylactic antibiotics against aerobic and anaerobic gram-negative bacteria is essential before an appendectomy. To ensure maximal effectiveness, prophylactic antibiotics should be administered within 60 minutes before initiating the procedure.
Antibiotics are essential in helping to prevent postoperative surgical site infection and intra-abdominal abscesses.[38] Generally, an antibiotic with broad gram-negative coverage covering Pseudomonas aeruginosa, Enterobacteriaceae resistant to non-pseudomonal cephalosporins, enteric streptococci, and anaerobes is indicated. However, after culture and antibiotic sensitivity assays, antibiotics should be adjusted.[39][40]
The Surgical Care Improvement Project has established current guidelines for prophylactic antibiotics.[41] One of the following options is recommended for patients without known allergies to penicillins or cephalosporins: either a single dose of intravenous cefotetan or cefoxitin or combination therapy with intravenous metronidazole and weight-adjusted cefazolin. In patients with known penicillin or cephalosporin allergy, combination therapy with intravenous clindamycin and levofloxacin, ciprofloxacin, gentamycin, or aztreonam is preferred.[41]
Technique or Treatment
Laparoscopic Appendectomy
Patient Preparation and Draping Procedures
- A wide abdominal prep and draping are indicated.
- The patient should be supine with the left arm tucked. However, after the port placements, a Trendelenburg position, with the right side up, provides improved visibility and access.
- Create a sterile surgical field from slightly superior to the bilateral costal margins extending inferiorly to the pubic tubercle and laterally to both the right and left flanks. The sterile field should allow for possible conversion to an open procedure.[42]
Abdominal Access
- Abdominal access may be obtained using the periumbilical Hasson technique, with a Veress needle or an optical trocar as dictated by the clinical situation and surgeon preference.[43]
Abdominal Insufflation and Port Placements
- If using the Hasson technique or a Veress needle, insufflate the peritoneal cavity with carbon dioxide gas. Insert a 5-mm angled laparoscope. Under direct visualization, place a 5-mm operating port in the midline above the pubic bone and a second 5-mm port in the lateral left lower quadrant.[44]
- Optical trocars, if used, are placed periumbilically. Under direct visualization, place a 5 mm port in the right lower quadrant just above the pubis and another 5-mm port in the left iliac fossa. Assuming a usual anatomic position of the appendix and a right-handed surgeon, the first trocar will be used to grasp and manipulate the appendix, and the second trocar will be used for the operating instruments.[37]
- Using a third trocar should be considered for appendiceal anatomical variations, including a subhepatic appendix.[37]
Procedure
- Exploration of the abdomen is completed before attention is turned to the right lower quadrant.
- The omentum and small bowel are swept cephalad. The fold of Treves or antimesenteric fat can be used to identify the terminal ileum; follow this to the cecum. In normal anatomy, the appendix can be identified at the confluence of the taeniae coli. If the appendix is retrocecal, mobilization of the retroperitoneal attachments of the cecum and ascending colon may be required. Proper patient positioning, as described above, facilitates the identification of the appendix. For a right-handed surgeon, the right-hand instrument retracts the most distal ileal loop, and the left-hand instrument optimizes cecal exposure. The preferred approach in patients with the subserosal appendix is the complete, meticulous dissection of the visceral peritoneum.[37]
- Once the appendix is identified, it should be held taut without specific preference to grasp the appendix by its tip or body. Complicated appendicitis with phlegmon or gangrene requires careful handling, and direct meso-appendiceal grasping is preferred.
- Divide the mesoappendix from the tip to the base using bipolar cautery; monopolar cautery is discouraged due to an increased risk of bowel injury.[37]
- Any adhesions formed by inflammatory processes between the appendix, small bowel, and cecum can be divided using blunt dissection; sharp dissection may be necessary.[45] The avoidance of electrocautery is recommended to prevent contact and conductive injury.[46]
- In cases of suboptimal visualization or dissection of the appendix, consider conversion to an open procedure.
- Once the tip of the appendix is visualized, it can be grasped and elevated off the cecum anteriorly. A window is created between the mesoappendix and the base of the appendix using a Maryland dissector. The safest orientation to create this window is placing the appendix and mesoappendix parallel to the lateral abdominal wall; this reduces the risk of bowel injury.
- Divide the mesoappendix using an endoscopic stapler loaded with vascular staples. Divide the appendix at its base using a second load of vascular staples. Caution must be taken to ensure the stapler is brought together close to the cecum to prevent the creation of an extra unnecessary appendiceal stump.[47]
- Place the resected appendix in an endoscopic retrieval bag; remove the bag through the umbilical port.
- Assess the staple lines to confirm hemostasis and integrity.
- Sweep the bowel caudally to return it to the lower abdomen; drape the omentum back over the small bowel and, ideally, the appendiceal stump.
- Insert the laparoscope through the midline port to ensure hemostasis of the anterior abdominal wall.
- Accessory port sites may be left open, reducing the risk of needle stick, length of the procedure, and overall cost without a higher incident rate of port-site hernias than fascial closure.[48]
- Close the skin according to the surgeon's preference.
Open Appendectomy
Patient Preparation and Draping Procedures
- A wide abdominal prep and draping are indicated.
- The patient should be supine.
- Create a sterile surgical field from slightly superior to the bilateral costal margins extending inferiorly to the pubic tubercle and laterally to both the right and left flanks.
Procedure
- In uncomplicated appendicitis, access to the McBurney point may be provided by selecting either an oblique (McBurney) incision or a transverse (Rockey-Davis or Elliot) incision. Alternatively, based on preoperative imaging, an incision can be made using the point of maximal tenderness or appendiceal location.
- A McBurney incision is made one-third of the way from the anterior-superior iliac spine (ASIS) to the umbilicus following Langer lines. Separate the external oblique, internal oblique, and transversus abdominis muscles along their fibers.[49]
- The Rockey-Davis or Elliot incision is a transverse incision close to the McBurney point, extending medially to the rectus abdominis muscle and laterally an equal distance. Blunt dissection and electrocautery are used to dissect the external aponeurosis. Expose the external aponeurosis in a superolateral to inferomedial fashion along its fibers to expose the underlying internal oblique muscle. Use blunt dissection to divide the internal oblique perpendicular to the direction of the fibers to expose the transverse abdominal muscle, which is divided in a similar fashion to expose the peritoneum.[50]
- Grasp the peritoneum with forceps, and if free of adhesion, incise it with a scalpel.
- Attention is then turned to locating the appendix. If the cecum can be visualized, it can be mobilized and used to identify the appendix. The appendix can be externalized using atraumatic graspers to advance with the taeniae coli. Alternatively, the cecum can be used as a guide to locate the appendix.
- Once the appendix is identified, dissect the mesoappendix, divide the appendiceal vessels between clamps, and ligate them with silk sutures.
- Crush the tissue at the appendiceal base with a right-angle clamp. Move the clamp distally and ligate the appendiceal base distal to the clamp with an absorbable suture.
- Excise the appendix proximal to the right-angle clamp with a blade. The appendiceal stump mucosa can be obliterated using electrocautery. Place a silk purse-string suture around the appendiceal base and invert the stump.[51]
- Confirm hemostasis. Close the peritoneal and fascial layers using absorbable sutures.[52]
- Close the skin according to the surgeon's preference.[53]
- Even in class III (contaminated) wounds due to perforated or gangrenous appendicitis, primary skin closure, and broad-spectrum antibiotic coverage are recommended.[54]
Complications
The most common complication following appendectomy is surgical site infection, including wound infections and intraabdominal abscesses. Surgical site infections are relatively rare in cases of uncomplicated appendicitis but may occur in up to 10% of patients with a perforated appendix.
Wound Infection
Superficial wound infections occur within the 30 days following an appendectomy and involve the skin and subcutaneous tissues. Diagnosis is based primarily on history and physical examination. Examination findings consistent with superficial wound infection include peri-incisional pain, swelling, and erythema. The diagnosis is supported by purulent drainage from the incision, a positive wound culture, or the need to open a surgical incision.
Deep wound infections occur in the 30 to 90 days following an appendectomy and include the muscles and fascia deep to the subcutaneous tissue. Again, a thorough medical history and physical examination should be performed. Examination findings consistent with a deep wound infection include per-incisional pain, tenderness, and systemic findings such as fever. The diagnosis is supported by purulent drainage from the incision site, a positive wound culture, or wound dehiscence.[55]
Preoperative antibiotics, appropriate wound scrubbing, specific intraoperative retractors, and intraoperative irrigation may be used to minimize the risk of postoperative wound infections. There is no difference in the rate of wound infection between primary and delayed primary incision closure.[56]
Compared to open appendectomy, laparoscopic appendectomy is associated with a lower risk of incision site infection but a higher risk of intra-abdominal and pelvic infection.[57]
Pelvic Abscess
Approximately 9.4% of patients who undergo appendectomy for complicated appendicitis will develop a postoperative pelvic abscess. Several measures have been recommended to reduce the risk of postoperative pelvic abscesses, including intraoperative peritoneal irrigation. Outcomes of the measures conflict, and no intervention has been proven more effective than another.[58]
Stump Appendicitis
Stump appendicitis, a form of recurrent appendicitis, may occur when an inadequate amount of appendiceal tissue is resected, and a long stump is left behind.[59] Post-appendectomy stump appendicitis most commonly occurs in cases of perforated appendicitis. Resection of adequate appendiceal tissue with less than 5 mm of stump preservation is recommended to minimize risk.[60]
Mortality
The mortality associated with appendectomy is low; it is considered a relatively safe procedure. Morbidity and mortality after appendiceal perforation are 5.1 per 1000. However, the mortality rate can differ depending on the geographic location, as evidenced by more developed countries having a rate of 0.09% to 0.24% and developing countries having a rate of 1% to 4%.
Clinical Significance
Appendiceal Perforation Rate and Timing of the Appendectomy
The risk of appendiceal perforation within 36 hours ranges from 16% to 36%, with the risk of perforation increasing by 5% every 12 hours. This highlights the importance of timely diagnosis and appendectomy.[8]
Postoperative Care for Nonperforated Appendicitis
Following an appendectomy procedure for nonperforated appendicitis, patients must adhere to a clear liquid diet and gradually transition to a regular diet. Typically, postoperative antibiotic therapy is unnecessary. Most patients can be discharged within 1 to 2 days postoperatively. However, uneventful same-day discharge is a viable option following laparoscopic appendectomy.[61]
Postoperative Care for Complicated Appendicitis
Patients who have undergone appendectomy for complicated appendicitis are advised to have a longer hospital admission period of about 5 to 7 days. However, it is important to note that achieving a complete diet tolerance to prevent ileus may be a more accurate index when making decisions. A 3- to 5-day course of postoperative antibiotic therapy is also recommended.[39][62][39]
Laparoscopic Appendectomy
Compared to open appendectomy, laparoscopic appendectomy has been found to reduce wound infection rates and hospital stays. The conversion rates from laparoscopic to open appendectomy vary from 0% to 27%.[8][59] Conversion should be done according to the surgeon’s experience, judgment, and ability to manage operative findings safely.[63] When deciding to proceed laparoscopically, the availability of trained staff, equipment, the ability and training of the operating surgeon, and the patient’s ability to tolerate pneumoperitoneum and anesthesia must be considered. Prior laparotomy is not considered an absolute contraindication to laparoscopic appendectomy. A laparoscopic approach is safe and effective for treating uncomplicated appendicitis and may also be safely performed in cases of perforated appendicitis.[64]
Appendectomy in the Case of a Normal Appearing Appendix
If a normal-appearing appendix is found intraoperatively and no other pathology has been identified, the decision for appendectomy should be individualized. Grossly normal appendixes may still be histopathologically abnormal in up to 40% of patients with a history compatible with acute appendicitis. It should be noted that an appendix is a viable option for antegrade continence enema (ACE), either following sphincteric trauma or in several pediatric congenital disabilities, including neurogenic bowel dysfunctions.[65][66]
Appendectomy in Unique Patient Populations
Laparoscopic appendectomy is the preferred surgical approach in patients over 65; in this population, open appendectomy has a 2.4% complication and mortality rate versus 0.5% in the laparoscopic approach.[67]
In pediatric patients, laparoscopic appendectomy may be performed safely.[59]
In pregnant patients with presumed appendicitis, laparoscopic appendectomy may be performed safely in any trimester. Laparoscopic appendectomy is considered the standard of care for pregnant patients by many.[68]
Enhancing Healthcare Team Outcomes
Patients with appendicitis typically present with abdominal pain localizing to the right lower quadrant. Emergency department triage staff should be familiar with the presenting signs and symptoms of acute appendicitis to facilitate urgent admission and treatment.
While the patient is undergoing further clinical evaluation, IV access should be obtained, and fluids, pain medication, and antibiotics administered as ordered. Imaging study orders should indicate the possibility of acute appendicitis. In addition, a pregnancy test should be performed in patients of childbearing age with a uterus.
After a presumptive diagnosis of appendicitis, the surgeon should coordinate with the patient and interprofessional team to determine the preferred surgical approach. The pharmacist should evaluate potential drug interaction allergies and report any concerns to the interprofessional team. Before surgery, the anesthesiologist and surgical assistant should be notified of the patient’s scenario and surgical plan. The operating room staff should ensure all necessary instruments and materials are available. Postoperatively, the nurse should monitor for acute changes in vital signs or symptoms and report findings to the team.
Early recognition of the signs and symptoms of appendicitis lowers rates of complications to improve outcomes. Laparoscopic appendectomy is an effective and safe method for treating uncomplicated appendicitis and may also be performed safely in patients with perforated appendicitis. [Level 1, 2] The laparoscopic approach is associated with lower morbidity and mortality rates and shorter stays regardless of whether abscesses developed or perforations occurred. [Level 2] Developing consistent operative methods decreases operating time, costs, and complications.[59] [Level 2]
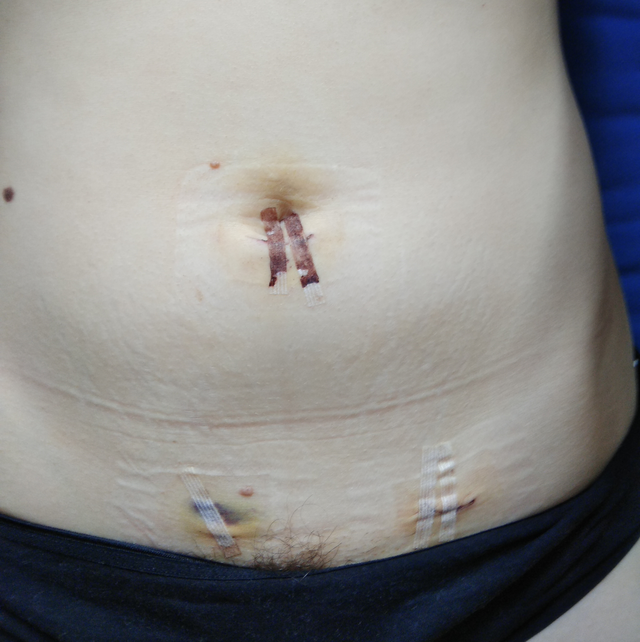
Media
(Click Image to Enlarge)
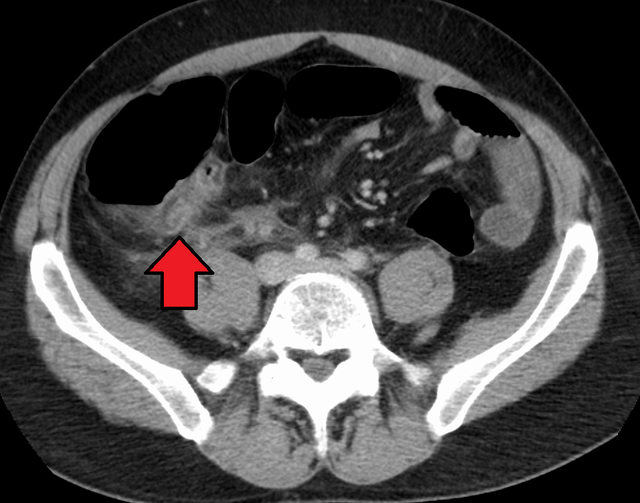
(Click Image to Enlarge)
References
Addiss DG, Shaffer N, Fowler BS, Tauxe RV. The epidemiology of appendicitis and appendectomy in the United States. American journal of epidemiology. 1990 Nov:132(5):910-25 [PubMed PMID: 2239906]
Level 2 (mid-level) evidenceBom WJ, Scheijmans JCG, Salminen P, Boermeester MA. Diagnosis of Uncomplicated and Complicated Appendicitis in Adults. Scandinavian journal of surgery : SJS : official organ for the Finnish Surgical Society and the Scandinavian Surgical Society. 2021 Jun:110(2):170-179. doi: 10.1177/14574969211008330. Epub 2021 Apr 14 [PubMed PMID: 33851877]
Krzyzak M, Mulrooney SM. Acute Appendicitis Review: Background, Epidemiology, Diagnosis, and Treatment. Cureus. 2020 Jun 11:12(6):e8562. doi: 10.7759/cureus.8562. Epub 2020 Jun 11 [PubMed PMID: 32670699]
McBurney C. Appendicitis. The Southern medical record. 1895 Jan:25(1):32-34 [PubMed PMID: 36025534]
Rutkow IM. Appendicitis: the quintessential American surgical disease. Archives of surgery (Chicago, Ill. : 1960). 1998 Sep:133(9):1024 [PubMed PMID: 9749862]
Sallinen V, Akl EA, You JJ, Agarwal A, Shoucair S, Vandvik PO, Agoritsas T, Heels-Ansdell D, Guyatt GH, Tikkinen KA. Meta-analysis of antibiotics versus appendicectomy for non-perforated acute appendicitis. The British journal of surgery. 2016 May:103(6):656-667. doi: 10.1002/bjs.10147. Epub 2016 Mar 17 [PubMed PMID: 26990957]
Level 1 (high-level) evidenceCODA Collaborative, Flum DR, Davidson GH, Monsell SE, Shapiro NI, Odom SR, Sanchez SE, Drake FT, Fischkoff K, Johnson J, Patton JH, Evans H, Cuschieri J, Sabbatini AK, Faine BA, Skeete DA, Liang MK, Sohn V, McGrane K, Kutcher ME, Chung B, Carter DW, Ayoung-Chee P, Chiang W, Rushing A, Steinberg S, Foster CS, Schaetzel SM, Price TP, Mandell KA, Ferrigno L, Salzberg M, DeUgarte DA, Kaji AH, Moran GJ, Saltzman D, Alam HB, Park PK, Kao LS, Thompson CM, Self WH, Yu JT, Wiebusch A, Winchell RJ, Clark S, Krishnadasan A, Fannon E, Lavallee DC, Comstock BA, Bizzell B, Heagerty PJ, Kessler LG, Talan DA. A Randomized Trial Comparing Antibiotics with Appendectomy for Appendicitis. The New England journal of medicine. 2020 Nov 12:383(20):1907-1919. doi: 10.1056/NEJMoa2014320. Epub 2020 Oct 5 [PubMed PMID: 33017106]
Level 1 (high-level) evidenceHumes DJ, Simpson J. Acute appendicitis. BMJ (Clinical research ed.). 2006 Sep 9:333(7567):530-4 [PubMed PMID: 16960208]
Barlow A, Muhleman M, Gielecki J, Matusz P, Tubbs RS, Loukas M. The vermiform appendix: a review. Clinical anatomy (New York, N.Y.). 2013 Oct:26(7):833-42. doi: 10.1002/ca.22269. Epub 2013 May 29 [PubMed PMID: 23716128]
Awayshih MMA, Nofal MN, Yousef AJ. Evaluation of Alvarado score in diagnosing acute appendicitis. The Pan African medical journal. 2019:34():15. doi: 10.11604/pamj.2019.34.15.17803. Epub 2019 Sep 6 [PubMed PMID: 31762884]
Bundy DG, Byerley JS, Liles EA, Perrin EM, Katznelson J, Rice HE. Does this child have appendicitis? JAMA. 2007 Jul 25:298(4):438-51 [PubMed PMID: 17652298]
Hansson J, Körner U, Khorram-Manesh A, Solberg A, Lundholm K. Randomized clinical trial of antibiotic therapy versus appendicectomy as primary treatment of acute appendicitis in unselected patients. The British journal of surgery. 2009 May:96(5):473-81. doi: 10.1002/bjs.6482. Epub [PubMed PMID: 19358184]
Level 1 (high-level) evidenceStyrud J, Eriksson S, Nilsson I, Ahlberg G, Haapaniemi S, Neovius G, Rex L, Badume I, Granström L. Appendectomy versus antibiotic treatment in acute appendicitis. a prospective multicenter randomized controlled trial. World journal of surgery. 2006 Jun:30(6):1033-7 [PubMed PMID: 16736333]
Level 1 (high-level) evidenceSalminen P, Tuominen R, Paajanen H, Rautio T, Nordström P, Aarnio M, Rantanen T, Hurme S, Mecklin JP, Sand J, Virtanen J, Jartti A, Grönroos JM. Five-Year Follow-up of Antibiotic Therapy for Uncomplicated Acute Appendicitis in the APPAC Randomized Clinical Trial. JAMA. 2018 Sep 25:320(12):1259-1265. doi: 10.1001/jama.2018.13201. Epub [PubMed PMID: 30264120]
Level 1 (high-level) evidenceVons C, Barry C, Maitre S, Pautrat K, Leconte M, Costaglioli B, Karoui M, Alves A, Dousset B, Valleur P, Falissard B, Franco D. Amoxicillin plus clavulanic acid versus appendicectomy for treatment of acute uncomplicated appendicitis: an open-label, non-inferiority, randomised controlled trial. Lancet (London, England). 2011 May 7:377(9777):1573-9. doi: 10.1016/S0140-6736(11)60410-8. Epub [PubMed PMID: 21550483]
Level 1 (high-level) evidenceWriting Group for the CODA Collaborative, Zhang IY, Voldal EC, Davidson GH, Liao JM, Thompson CM, Self WH, Kao LS, Cherry-Bukowiec J, Raghavendran K, Kaji AH, DeUgarte DA, Gonzalez E, Mandell KA, Ohe K, Siparsky N, Price TP, Evans DC, Victory J, Chiang W, Jones A, Kutcher ME, Ciomperlik H, Liang MK, Evans HL, Faine BA, Neufeld M, Sanchez SE, Krishnadasan A, Comstock BA, Heagerty PJ, Lawrence SO, Monsell SE, Fannon EEC, Kessler LG, Talan DA, Flum DR. Association of Patient Belief About Success of Antibiotics for Appendicitis and Outcomes: A Secondary Analysis of the CODA Randomized Clinical Trial. JAMA surgery. 2022 Dec 1:157(12):1080-1087. doi: 10.1001/jamasurg.2022.4765. Epub [PubMed PMID: 36197656]
Level 1 (high-level) evidenceSartelli M, Baiocchi GL, Di Saverio S, Ferrara F, Labricciosa FM, Ansaloni L, Coccolini F, Vijayan D, Abbas A, Abongwa HK, Agboola J, Ahmed A, Akhmeteli L, Akkapulu N, Akkucuk S, Altintoprak F, Andreiev AL, Anyfantakis D, Atanasov B, Bala M, Balalis D, Baraket O, Bellanova G, Beltran M, Melo RB, Bini R, Bouliaris K, Brunelli D, Castillo A, Catani M, Che Jusoh A, Chichom-Mefire A, Cocorullo G, Coimbra R, Colak E, Costa S, Das K, Delibegovic S, Demetrashvili Z, Di Carlo I, Kiseleva N, El Zalabany T, Faro M, Ferreira M, Fraga GP, Gachabayov M, Ghnnam WM, Giménez Maurel T, Gkiokas G, Gomes CA, Griffiths E, Guner A, Gupta S, Hecker A, Hirano ES, Hodonou A, Hutan M, Ioannidis O, Isik A, Ivakhov G, Jain S, Jokubauskas M, Karamarkovic A, Kauhanen S, Kaushik R, Kavalakat A, Kenig J, Khokha V, Khor D, Kim D, Kim JI, Kong V, Lasithiotakis K, Leão P, Leon M, Litvin A, Lohsiriwat V, López-Tomassetti Fernandez E, Lostoridis E, Maciel J, Major P, Dimova A, Manatakis D, Marinis A, Martinez-Perez A, Marwah S, McFarlane M, Mesina C, Pędziwiatr M, Michalopoulos N, Misiakos E, Mohamedahmed A, Moldovanu R, Montori G, Mysore Narayana R, Negoi I, Nikolopoulos I, Novelli G, Novikovs V, Olaoye I, Omari A, Ordoñez CA, Ouadii M, Ozkan Z, Pal A, Palini GM, Partecke LI, Pata F, Pędziwiatr M, Pereira Júnior GA, Pintar T, Pisarska M, Ploneda-Valencia CF, Pouggouras K, Prabhu V, Ramakrishnapillai P, Regimbeau JM, Reitz M, Rios-Cruz D, Saar S, Sakakushev B, Seretis C, Sazhin A, Shelat V, Skrovina M, Smirnov D, Spyropoulos C, Strzałka M, Talving P, Teixeira Gonsaga RA, Theobald G, Tomadze G, Torba M, Tranà C, Ulrych J, Uzunoğlu MY, Vasilescu A, Occhionorelli S, Venara A, Vereczkei A, Vettoretto N, Vlad N, Walędziak M, Yilmaz TU, Yuan KC, Yunfeng C, Zilinskas J, Grelpois G, Catena F. Prospective Observational Study on acute Appendicitis Worldwide (POSAW). World journal of emergency surgery : WJES. 2018:13():19. doi: 10.1186/s13017-018-0179-0. Epub 2018 Apr 16 [PubMed PMID: 29686725]
Level 2 (mid-level) evidenceHarnoss JC, Zelienka I, Probst P, Grummich K, Müller-Lantzsch C, Harnoss JM, Ulrich A, Büchler MW, Diener MK. Antibiotics Versus Surgical Therapy for Uncomplicated Appendicitis: Systematic Review and Meta-analysis of Controlled Trials (PROSPERO 2015: CRD42015016882). Annals of surgery. 2017 May:265(5):889-900. doi: 10.1097/SLA.0000000000002039. Epub [PubMed PMID: 27759621]
Level 1 (high-level) evidencePerez KS, Allen SR. Complicated appendicitis and considerations for interval appendectomy. JAAPA : official journal of the American Academy of Physician Assistants. 2018 Sep:31(9):35-41. doi: 10.1097/01.JAA.0000544304.30954.40. Epub [PubMed PMID: 30153202]
Mentula P, Sammalkorpi H, Leppäniemi A. Laparoscopic Surgery or Conservative Treatment for Appendiceal Abscess in Adults? A Randomized Controlled Trial. Annals of surgery. 2015 Aug:262(2):237-42. doi: 10.1097/SLA.0000000000001200. Epub [PubMed PMID: 25775072]
Level 1 (high-level) evidenceSimillis C, Symeonides P, Shorthouse AJ, Tekkis PP. A meta-analysis comparing conservative treatment versus acute appendectomy for complicated appendicitis (abscess or phlegmon). Surgery. 2010 Jun:147(6):818-29. doi: 10.1016/j.surg.2009.11.013. Epub 2010 Feb 10 [PubMed PMID: 20149402]
Level 2 (mid-level) evidenceAndersson RE, Petzold MG. Nonsurgical treatment of appendiceal abscess or phlegmon: a systematic review and meta-analysis. Annals of surgery. 2007 Nov:246(5):741-8 [PubMed PMID: 17968164]
Level 1 (high-level) evidenceDarwazeh G, Cunningham SC, Kowdley GC. A Systematic Review of Perforated Appendicitis and Phlegmon: Interval Appendectomy or Wait-and-See? The American surgeon. 2016 Jan:82(1):11-5 [PubMed PMID: 26802841]
Level 1 (high-level) evidenceCheng Y, Xiong X, Lu J, Wu S, Zhou R, Cheng N. Early versus delayed appendicectomy for appendiceal phlegmon or abscess. The Cochrane database of systematic reviews. 2017 Jun 2:6(6):CD011670. doi: 10.1002/14651858.CD011670.pub2. Epub 2017 Jun 2 [PubMed PMID: 28574593]
Level 1 (high-level) evidenceSchuster KM, Holena DN, Salim A, Savage S, Crandall M. American Association for the Surgery of Trauma emergency general surgery guideline summaries 2018: acute appendicitis, acute cholecystitis, acute diverticulitis, acute pancreatitis, and small bowel obstruction. Trauma surgery & acute care open. 2019:4(1):e000281. doi: 10.1136/tsaco-2018-000281. Epub 2019 Mar 27 [PubMed PMID: 31058240]
Gorter RR, Eker HH, Gorter-Stam MA, Abis GS, Acharya A, Ankersmit M, Antoniou SA, Arolfo S, Babic B, Boni L, Bruntink M, van Dam DA, Defoort B, Deijen CL, DeLacy FB, Go PM, Harmsen AM, van den Helder RS, Iordache F, Ket JC, Muysoms FE, Ozmen MM, Papoulas M, Rhodes M, Straatman J, Tenhagen M, Turrado V, Vereczkei A, Vilallonga R, Deelder JD, Bonjer J. Diagnosis and management of acute appendicitis. EAES consensus development conference 2015. Surgical endoscopy. 2016 Nov:30(11):4668-4690 [PubMed PMID: 27660247]
Level 3 (low-level) evidenceDi Saverio S, Birindelli A, Kelly MD, Catena F, Weber DG, Sartelli M, Sugrue M, De Moya M, Gomes CA, Bhangu A, Agresta F, Moore EE, Soreide K, Griffiths E, De Castro S, Kashuk J, Kluger Y, Leppaniemi A, Ansaloni L, Andersson M, Coccolini F, Coimbra R, Gurusamy KS, Campanile FC, Biffl W, Chiara O, Moore F, Peitzman AB, Fraga GP, Costa D, Maier RV, Rizoli S, Balogh ZJ, Bendinelli C, Cirocchi R, Tonini V, Piccinini A, Tugnoli G, Jovine E, Persiani R, Biondi A, Scalea T, Stahel P, Ivatury R, Velmahos G, Andersson R. WSES Jerusalem guidelines for diagnosis and treatment of acute appendicitis. World journal of emergency surgery : WJES. 2016:11():34. doi: 10.1186/s13017-016-0090-5. Epub 2016 Jul 18 [PubMed PMID: 27437029]
Sauerland S, Lefering R, Neugebauer EA. Laparoscopic versus open surgery for suspected appendicitis. The Cochrane database of systematic reviews. 2002:(1):CD001546 [PubMed PMID: 11869603]
Level 1 (high-level) evidenceRipollés T, Martínez MJ, Morote V, Errando J. Appendiceal involvement in Crohn's disease: gray-scale sonography and color Doppler flow features. AJR. American journal of roentgenology. 2006 Apr:186(4):1071-8 [PubMed PMID: 16554581]
Esteban JM, Maldonado L, Sanchiz V, Minguez M, Benages A. Activity of Crohn's disease assessed by colour Doppler ultrasound analysis of the affected loops. European radiology. 2001:11(8):1423-8 [PubMed PMID: 11519551]
Machado NO, Chopra PJ, Hamdani AA. Crohn's disease of the appendix with enterocutaneous fistula post-appendicectomy: An approach to management. North American journal of medical sciences. 2010 Mar:2(3):158-61 [PubMed PMID: 22624132]
Level 3 (low-level) evidenceTsukui H, Koinuma K, Morimoto M, Horie H, Lefor AK, Kagaya Y, Takahashi H, Yano T, Matsubara D, Yamamoto H, Sata N. Crohn's disease presenting as a ceco-urachal fistula. Clinical journal of gastroenterology. 2017 Feb:10(1):32-36. doi: 10.1007/s12328-016-0691-2. Epub 2016 Oct 20 [PubMed PMID: 27766543]
Zhang L, Hu C, Zhang Z, Liu R, Liu G, Xue D, Wang Z, Wu C, Wu X, She J, Shi F. Association between prior appendectomy and the risk and course of Crohn's disease: A systematic review and meta-analysis. Clinics and research in hepatology and gastroenterology. 2023 Mar:47(3):102090. doi: 10.1016/j.clinre.2023.102090. Epub 2023 Feb 4 [PubMed PMID: 36746236]
Level 1 (high-level) evidencePiovani D, Danese S, Peyrin-Biroulet L, Nikolopoulos GK, Lytras T, Bonovas S. Environmental Risk Factors for Inflammatory Bowel Diseases: An Umbrella Review of Meta-analyses. Gastroenterology. 2019 Sep:157(3):647-659.e4. doi: 10.1053/j.gastro.2019.04.016. Epub 2019 Apr 20 [PubMed PMID: 31014995]
Level 1 (high-level) evidenceKaderli R. [Incidental appendectomy: standard or unjustified risk?]. Therapeutische Umschau. Revue therapeutique. 2014 Dec:71(12):753-8. doi: 10.1024/0040-5930/a000621. Epub [PubMed PMID: 25447090]
Kim SH, Kim HY, Lee SH, Yang K, Park BS, Choi BH, Jung HJ. Reducing Supply Cost by Standardization of Surgical Equipment in Laparoscopic Appendectomy. Quality management in health care. 2021 Oct-Dec 01:30(4):259-266. doi: 10.1097/QMH.0000000000000315. Epub [PubMed PMID: 34354034]
Level 2 (mid-level) evidenceVeziant J, Slim K. Laparoscopic appendectomy. Journal of visceral surgery. 2014 Jun:151(3):223-8. doi: 10.1016/j.jviscsurg.2014.03.011. Epub 2014 Apr 24 [PubMed PMID: 24768620]
Andersen BR, Kallehave FL, Andersen HK. Antibiotics versus placebo for prevention of postoperative infection after appendicectomy. The Cochrane database of systematic reviews. 2005 Jul 20:2005(3):CD001439 [PubMed PMID: 16034862]
Level 1 (high-level) evidenceSolomkin JS, Mazuski JE, Bradley JS, Rodvold KA, Goldstein EJ, Baron EJ, O'Neill PJ, Chow AW, Dellinger EP, Eachempati SR, Gorbach S, Hilfiker M, May AK, Nathens AB, Sawyer RG, Bartlett JG. Diagnosis and management of complicated intra-abdominal infection in adults and children: guidelines by the Surgical Infection Society and the Infectious Diseases Society of America. Surgical infections. 2010 Feb:11(1):79-109. doi: 10.1089/sur.2009.9930. Epub [PubMed PMID: 20163262]
Woerther PL, Burdet C, Chachaty E, Andremont A. Trends in human fecal carriage of extended-spectrum β-lactamases in the community: toward the globalization of CTX-M. Clinical microbiology reviews. 2013 Oct:26(4):744-58. doi: 10.1128/CMR.00023-13. Epub [PubMed PMID: 24092853]
Bratzler DW, Dellinger EP, Olsen KM, Perl TM, Auwaerter PG, Bolon MK, Fish DN, Napolitano LM, Sawyer RG, Slain D, Steinberg JP, Weinstein RA, American Society of Health-System Pharmacists (ASHP), Infectious Diseases Society of America (IDSA), Surgical Infection Society (SIS), Society for Healthcare Epidemiology of America (SHEA). Clinical practice guidelines for antimicrobial prophylaxis in surgery. Surgical infections. 2013 Feb:14(1):73-156. doi: 10.1089/sur.2013.9999. Epub 2013 Mar 5 [PubMed PMID: 23461695]
Level 1 (high-level) evidenceAhmed K, Connelly TM, Bashar K, Walsh SR. Are wound ring protectors effective in reducing surgical site infection post appendectomy? A systematic review and meta-analysis. Irish journal of medical science. 2016 Feb:185(1):35-42. doi: 10.1007/s11845-015-1381-7. Epub 2015 Nov 11 [PubMed PMID: 26560110]
Level 1 (high-level) evidenceKovachev S, Ganovska A, Atanasova V, Sergeev S, Mutafchiyski V, Vladov N. [OPEN LAPAROSCOPY--A MODIFIED HASSON TECHNIQUE]. Akusherstvo i ginekologiia. 2015:54(4):52-6 [PubMed PMID: 26410948]
Ferzli GS, Fingerhut A. Trocar placement for laparoscopic abdominal procedures: a simple standardized method. Journal of the American College of Surgeons. 2004 Jan:198(1):163-73 [PubMed PMID: 14698326]
Szomstein S, Lo Menzo E, Simpfendorfer C, Zundel N, Rosenthal RJ. Laparoscopic lysis of adhesions. World journal of surgery. 2006 Apr:30(4):535-40 [PubMed PMID: 16555020]
Bhullar JS, Gayagoy J, Chaudhary S, Kolachalam RB. Delayed presentation of a bowel Bovie injury after laparoscopic ventral hernia repair. JSLS : Journal of the Society of Laparoendoscopic Surgeons. 2013 Jul-Sep:17(3):495-8 [PubMed PMID: 24018096]
Level 3 (low-level) evidenceBeldi G, Vorburger SA, Bruegger LE, Kocher T, Inderbitzin D, Candinas D. Analysis of stapling versus endoloops in appendiceal stump closure. The British journal of surgery. 2006 Nov:93(11):1390-3 [PubMed PMID: 16862615]
Level 2 (mid-level) evidenceGutierrez M, Stuparich M, Behbehani S, Nahas S. Does closure of fascia, type, and location of trocar influence occurrence of port site hernias? A literature review. Surgical endoscopy. 2020 Dec:34(12):5250-5258. doi: 10.1007/s00464-020-07826-8. Epub 2020 Jul 29 [PubMed PMID: 32728766]
McBurney C. IV. The Incision Made in the Abdominal Wall in Cases of Appendicitis, with a Description of a New Method of Operating. Annals of surgery. 1894 Jul:20(1):38-43 [PubMed PMID: 17860070]
Level 3 (low-level) evidenceCavalli M, Bruni PG, Lombardo F, Morlacchi A, Andretto Amodeo C, Campanelli G. Original concepts in anatomy, abdominal-wall surgery, and component separation technique and strategy. Hernia : the journal of hernias and abdominal wall surgery. 2020 Apr:24(2):411-419. doi: 10.1007/s10029-019-02030-7. Epub 2019 Sep 6 [PubMed PMID: 31493052]
Okamoto S, Otowa Y, Fujinaka R, Arai K, Murata K, Mii Y, Kakinoki K, Oka S, Kanaji S, Kakeji Y, Kuroda D. Purse-string suture after ligating by endoloop for closing of the appendiceal stump is an alternative for endostapler in selected cases: A propensity score-matched study. Asian journal of endoscopic surgery. 2021 Oct:14(4):775-781. doi: 10.1111/ases.12942. Epub 2021 Apr 21 [PubMed PMID: 33881223]
Level 3 (low-level) evidenceMuysoms FE, Antoniou SA, Bury K, Campanelli G, Conze J, Cuccurullo D, de Beaux AC, Deerenberg EB, East B, Fortelny RH, Gillion JF, Henriksen NA, Israelsson L, Jairam A, Jänes A, Jeekel J, López-Cano M, Miserez M, Morales-Conde S, Sanders DL, Simons MP, Śmietański M, Venclauskas L, Berrevoet F, European Hernia Society. European Hernia Society guidelines on the closure of abdominal wall incisions. Hernia : the journal of hernias and abdominal wall surgery. 2015 Feb:19(1):1-24. doi: 10.1007/s10029-014-1342-5. Epub 2015 Jan 25 [PubMed PMID: 25618025]
Switzer NJ, Gill RS, Karmali S. The evolution of the appendectomy: from open to laparoscopic to single incision. Scientifica. 2012:2012():895469. doi: 10.6064/2012/895469. Epub 2012 May 27 [PubMed PMID: 24278754]
Margenthaler JA, Longo WE, Virgo KS, Johnson FE, Oprian CA, Henderson WG, Daley J, Khuri SF. Risk factors for adverse outcomes after the surgical treatment of appendicitis in adults. Annals of surgery. 2003 Jul:238(1):59-66 [PubMed PMID: 12832966]
Stryja J. Surgical site infection and local management of the wound meta-analysis. Rozhledy v chirurgii : mesicnik Ceskoslovenske chirurgicke spolecnosti. 2021 Summer:100(7):313-324. doi: 10.33699/PIS.2021.100.7.313-324. Epub [PubMed PMID: 34465107]
Level 1 (high-level) evidenceLemieur TP, Rodriguez JL, Jacobs DM, Bennett ME, West MA. Wound management in perforated appendicitis. The American surgeon. 1999 May:65(5):439-43 [PubMed PMID: 10231213]
Fleming FJ, Kim MJ, Messing S, Gunzler D, Salloum R, Monson JR. Balancing the risk of postoperative surgical infections: a multivariate analysis of factors associated with laparoscopic appendectomy from the NSQIP database. Annals of surgery. 2010 Dec:252(6):895-900. doi: 10.1097/SLA.0b013e3181f194fe. Epub [PubMed PMID: 21107099]
Level 2 (mid-level) evidenceBhangu A, Søreide K, Di Saverio S, Assarsson JH, Drake FT. Acute appendicitis: modern understanding of pathogenesis, diagnosis, and management. Lancet (London, England). 2015 Sep 26:386(10000):1278-1287. doi: 10.1016/S0140-6736(15)00275-5. Epub [PubMed PMID: 26460662]
Level 3 (low-level) evidenceKorndorffer JR Jr, Fellinger E, Reed W. SAGES guideline for laparoscopic appendectomy. Surgical endoscopy. 2010 Apr:24(4):757-61. doi: 10.1007/s00464-009-0632-y. Epub 2009 Sep 29 [PubMed PMID: 19787402]
Kanona H, Al Samaraee A, Nice C, Bhattacharya V. Stump appendicitis: a review. International journal of surgery (London, England). 2012:10(9):425-8. doi: 10.1016/j.ijsu.2012.07.007. Epub 2012 Jul 27 [PubMed PMID: 22846617]
. Discussion. Journal of the American College of Surgeons. 2016 Apr:222(4):709-11. doi: 10.1016/j.jamcollsurg.2016.01.013. Epub [PubMed PMID: 27016999]
Berríos-Torres SI, Umscheid CA, Bratzler DW, Leas B, Stone EC, Kelz RR, Reinke CE, Morgan S, Solomkin JS, Mazuski JE, Dellinger EP, Itani KMF, Berbari EF, Segreti J, Parvizi J, Blanchard J, Allen G, Kluytmans JAJW, Donlan R, Schecter WP, Healthcare Infection Control Practices Advisory Committee. Centers for Disease Control and Prevention Guideline for the Prevention of Surgical Site Infection, 2017. JAMA surgery. 2017 Aug 1:152(8):784-791. doi: 10.1001/jamasurg.2017.0904. Epub [PubMed PMID: 28467526]
Liu Y, Cui Z, Zhang R. Laparoscopic Versus Open Appendectomy for Acute Appendicitis in Children. Indian pediatrics. 2017 Nov 15:54(11):938-941 [PubMed PMID: 28849763]
Gignoux B, Blanchet MC, Lanz T, Vulliez A, Saffarini M, Bothorel H, Robert M, Frering V. Should ambulatory appendectomy become the standard treatment for acute appendicitis? World journal of emergency surgery : WJES. 2018:13():28. doi: 10.1186/s13017-018-0191-4. Epub 2018 Jun 28 [PubMed PMID: 29988464]
Gelpke K, Hamminga JTH, van Bastelaar JJ, de Vos B, Bodegom ME, Heineman E, Hofker HS, El Moumni M, Haveman JW. Reducing the negative appendectomy rate with the laparoscopic appendicitis score; a multicenter prospective cohort and validation study. International journal of surgery (London, England). 2020 Jul:79():257-264. doi: 10.1016/j.ijsu.2020.04.041. Epub 2020 May 6 [PubMed PMID: 32387211]
Level 1 (high-level) evidenceSpinelli M, Sampogna G, Rizzato L, Spinelli A, Sammartano F, Cimbanassi S, Montanari E, Chiara O. The Malone antegrade continence enema adapting a transanal irrigation system in patients with neurogenic bowel dysfunction. Spinal cord series and cases. 2021 Apr 23:7(1):34. doi: 10.1038/s41394-021-00397-3. Epub 2021 Apr 23 [PubMed PMID: 33893272]
Level 3 (low-level) evidenceWang D, Dong T, Shao Y, Gu T, Xu Y, Jiang Y. Laparoscopy versus open appendectomy for elderly patients, a meta-analysis and systematic review. BMC surgery. 2019 May 28:19(1):54. doi: 10.1186/s12893-019-0515-7. Epub 2019 May 28 [PubMed PMID: 31138196]
Level 1 (high-level) evidenceLee SH, Lee JY, Choi YY, Lee JG. Laparoscopic appendectomy versus open appendectomy for suspected appendicitis during pregnancy: a systematic review and updated meta-analysis. BMC surgery. 2019 Apr 25:19(1):41. doi: 10.1186/s12893-019-0505-9. Epub 2019 Apr 25 [PubMed PMID: 31023289]
Level 1 (high-level) evidence