Introduction
Acute rheumatic fever (ARF) is an immune-mediated nonsuppurative complication of group A streptococcal (GAS) pharyngitis.[1] Approximately 470,000 new cases of ARF occur annually, with a more significant disease burden in developing countries with higher rates of untreated or inadequately treated GAS infections.[2] Globally, over 275,000 deaths yearly are attributed to rheumatic heart disease (RHD).[3] The most significant contributors to the spread of GAS pharyngitis are household overcrowding, poor sanitation, and inadequate access to healthcare.[4]
The pathophysiology of ARF is characterized by an aberrant immune response to GAS infection triggered by molecular mimicry between GAS antigens and self-antigens. This immune response typically manifests 2 to 4 weeks after the initial GAS infection and may lead to the development of carditis, valvulitis, Sydenham chorea, subcutaneous nodules, erythema marginatum, and polyarthritis that is usually migratory.[5] The severity and distribution of these manifestations vary significantly between individuals making the diagnosis of ARF challenging. Early recognition of ARF using the modified Jones criteria is essential in treating acute infection and preventing complications. A major long-term consequence is RHD, which carries significant morbidity and mortality.
Etiology
Register For Free And Read The Full Article
Search engine and full access to all medical articles
10 free questions in your specialty
Free CME/CE Activities
Free daily question in your email
Save favorite articles to your dashboard
Emails offering discounts
Learn more about a Subscription to StatPearls Point-of-Care
Etiology
ARF is an inflammatory response to a preceding GAS pharyngeal infection. GAS infections can manifest as a broad range of clinical conditions, from superficial infections such as impetigo and pharyngitis to more invasive processes, including toxic shock syndrome and necrotizing fasciitis.[6] ARF is more strongly associated with GAS pharyngitis than skin infections.[7] However, some data suggest that skin infections, particularly impetigo, may play a role for high-risk populations such as the Indigenous people of Australia.[8]
In most cases, appropriate antibiotic treatment of acute GAS infection prevents the development of ARF. Individuals with GAS infection who cannot seek medical care or have subclinical GAS infection and do not present to care are at risk for developing ARF. Environmental and socioeconomic factors, such as household overcrowding, also play a significant role in spreading GAS infections and developing ARF.
Epidemiology
There are approximately 470,000 new cases of ARF and 233,000 attributable deaths to ARF or RHD yearly.[9] Overall, the incidence and severity of ARF have declined since the 1900s, likely owing to industrialization, improved housing conditions, improvement in healthcare access, and the introduction of penicillin. Historically, an estimated 3% of patients with untreated acute GAS pharyngitis develop ARF.[10]
High-risk patients with a history of ARF have an estimated 50% recurrence rate of ARF following untreated GAS pharyngitis.[11] Globally, the reported incidence of ARF is likely underestimated due to a lack of data, primarily from developing areas. While anyone can develop ARF, the disease is most commonly seen in children between 5 and 15 years old.[12] There is no gender predilection for ARF, but females are more likely to progress to RHD.[13]
The populations of developing countries and Indigenous people are disproportionately affected by ARF, likely due to many environmental and socioeconomic factors, including lack of access to treatment and increased GAS transmission due to overcrowding.[14] The yearly incidence of ARF in the United States is 10/100,000 compared to an annual incidence in India of 51/100,000. The Indigenous population in Australia has one of the highest reported incidence rates, ranging from 150 to 380 cases per 100,000 children aged 5 to 14 years.[15]
In the United States, hospitalizations secondary to ARF are more common in boys, with the highest rates occurring in 6- to 11-year-old boys of Asian and Pacific Islander descent.[16]
The significant sequela of ARF is the development of RHD. Approximately 39 million people worldwide are estimated to be living with RHD.[17] There are currently no available reports on the incidence of ARF in Africa, where it is believed that almost 50% of all cases of RHD in children younger than 15 occur.[18]
Pathophysiology
The pathophysiology of ARF is incompletely understood but thought to be multifactorial. Preceding GAS infection is necessary for the development of ARF. Additionally, host factors and repeated exposures to GAS contribute to the pathogenesis of ARF.
Group A Streptococcus
The emm genes of GAS encode for the M and M-like proteins. There are 5 chromosomal patterns of emm genes, labeled A-E. Evidence suggests that pharyngitis-inducing strains of GAS have the more “rheumatogenic” emm gene patterns A, B, and C.[19][20] There has been a significant decrease in the circulation of rheumatogenic strains in low-risk areas like the United States.[21] However, the complete role of bacterial strains and virulence factors in the pathogenesis of ARF is incompletely understood, and it has been shown that any strain of GAS can cause ARF.[7][22]
Molecular Mimicry
In molecular mimicry, antibodies formed against GAS antigens crossreact with self-antigens, leading to a dysregulated immune response. There are a variety of GAS antigens implicated in molecular mimicry. The M protein moiety and N-acetyl-β-D-glucosamine (NABG) of GAS species exhibit structural similarity to myosin, leading to cardiac myositis and valvulitis.[23][24] Antibody-antigen complexes may also deposit in joints leading to the characteristic migratory polyarthritis.
Aschoff bodies are granulomatous formations found on the surface of cardiac valves in patients with RHD presumptively secondary to an interaction between T-cells and upregulated expression of vascular cell adhesion molecule-1 (VCAM-1).[25]
In animal models, antibodies to NABG crossreact with mammalian lysoganglioside and reproduce chorea, indicating that molecular mimicry may play a role in the development of Sydenham chorea.[26] In humans, the basal ganglia are impacted in Sydenham Chorea; patients with ARF demonstrate putamen enlargement with magnetic resonance imaging.[27]
Group A carbohydrates share epitopes with keratin, and cross-reactivity may lead to erythema marginatum.[28]
Host Susceptibility
Host susceptibility to ARF is likely polygenic.[29] Monozygotic twin studies demonstrate a greater than 40% concordance risk for ARF.[30] Human leukocyte antigen alleles and tumor necrosis factor polymorphisms play a role in genetic susceptibility to acute rheumatic fever.[31][32][33] A study conducted across 8 countries in Oceania has suggested an allele on the immunoglobulin heavy chain is associated with susceptibility to ARF.[34][32]
Histopathology
When antibodies against GAS surface antigen bind to the surface of heart valves, they upregulate vascular cell adhesion molecule 1 (VCAM1), which allows T cells to adhere to the endocardium and form granulomatous depositions characteristic of acute rheumatic fever, termed Aschoff bodies.[32] These Aschoff bodies contain areas of active inflammation with fibrinoid necrosis, lymphocytic infiltration, plasma cells, and enlarged macrophages with condensed nuclei termed Anitschkow cells. The chromatin within the nucleus of the Anitschkow cells may appear ribbon-like and resemble a caterpillar; therefore, these cells are also called caterpillar cells.[35] Over time, valvular fibrosis, histiocytosis, and neovascularization suggest developing chronic disease and RHD.[36]
The classic histopathology of skin biopsies of erythema marginatum shows a polymorphous infiltrate of neutrophils and mononuclear cells in the papillary and upper half of the reticular dermis.[37]
Biopsies of subcutaneous nodules demonstrate increased numbers of dilated blood vessels with peripherally thickened walls, fibrinoid necrosis, and fibrosis with attachment to tendons. Histologically they resemble the lesions of rheumatoid arthritis with central fibrinoid necrosis, surrounded by histiocytes, perivascular lymphocytes, and neutrophils.[38]
History and Physical
The diagnosis of ARF is clinically based on the revised Jones criteria and typically presents within 2 to 4 weeks after an untreated GAS infection, most commonly GAS pharyngitis. A history of recurrent skin infections consistent with GAS may also be a preceding illness in specific high-risk populations. As many as one-third of patients with ARF do not recall preceding pharyngitis.[39]
The hallmarks of GAS pharyngitis include fever, throat pain, headaches, and chills. Additionally, abdominal pain, nausea, and vomiting may be present, particularly in young children. An antecedent illness with these signs and symptoms should alert clinicians to the possibility of GAS pharyngitis.[40] The clinical manifestations of ARF vary drastically; some infections may be subclinical, and a diagnosis of ARF is not made until a patient is diagnosed with cardiac disease. Most patients with ARF display constitutional symptoms, including fevers, chills, and fatigue. Arthritis or arthralgias are usually the earliest manifestations of ARF, occurring in 60% to 80% of patients. Joint symptoms are typically migratory and characterized by erythematous, swollen, and extremely tender joints; the large joints such as the knee, ankle, or wrist are most commonly affected.
Carditis is the most serious presentation of ARF. The most common physical examination findings of carditis are tachycardia or the presence of a new murmur. Carditis occurs in 50% to 80% of patients with ARF and usually presents as pancarditis within 2 to 3 weeks involving the pericardium, epicardium, myocardium, and endocardium.[41] Carditis may also present with valvulitis, often seen on left-sided high-pressure valves. The mitral valve is affected in 50% to 60% of cases of valvulitis; mitral regurgitation is usually the earliest manifestation.[42] The physical examination of patients with mitral regurgitation frequently reveals a holosystolic murmur loudest at the apex and radiating to the left axilla. Progressive valvular damage can lead to mitral stenosis.
The aortic valve is affected in 20% of patients with valvulitis.[42] Early aortic valve damage leads to aortic regurgitation, marked by a diastolic murmur heard best at the base of the heart and increased by the patient sitting forward. Progressive damage leads to aortic stenosis. The tricuspid valve is only affected in 10% of cases of valvulitis and typically results in tricuspid regurgitation.[42]
The transition from ARF to RHD occurs when valvular lesions evolve over the years or during multiple episodes of ARF. Cardiomyopathy and heart failure can occur, even during acute rheumatic fever, due to severe pancarditis or valvulopathy.
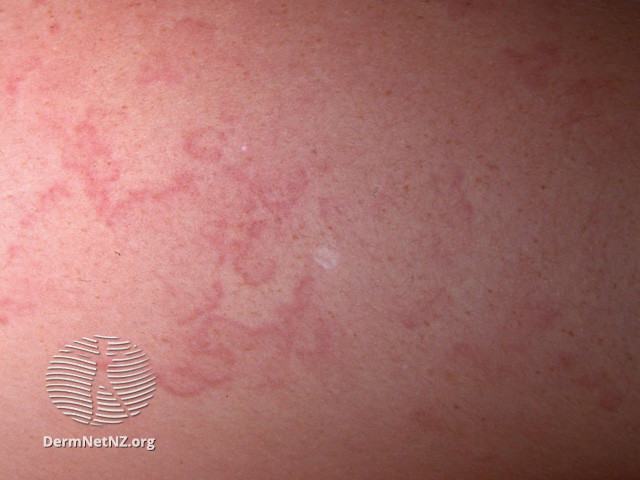
Dermatologic manifestations of acute rheumatic fever include subcutaneous nodules and erythema marginatum. Subcutaneous nodules occur in less than 10% of patients with ARF and are firm, painless lesions over joints, predominately on extensor surfaces. These nodules are typically associated with severe carditis. Erythema marginatum occurs in less than 6% of patients with ARF and generally is a pink or pale red annular, nonpruritic rash with raised edges and central clearing found on the trunk and limbs (see Image. Erythema Marginatum). Erythema marginatum is often described as serpiginous and fleeting, appearing on one body part, fading, and reappearing elsewhere. Erythema marginatum seems to be a more common manifestation in older children with ARF.[43]
Sydenham chorea (SC) is a neurologic manifestation of ARF that occurs in 10% to 30% of cases. It is a late-stage neurological complication usually occurring 1 to 8 months after GAS infection. SC presents as involuntary, irregular “jerking” movements of the face, hands, or feet.[44] These choreiform movements are more extreme on one side of the body and do not occur during sleep. SC can be complicated by behavioral symptoms such as agitation, anxiety, or inappropriate laughing or crying.[45] Facial grimaces and tics are common and may be accompanied by emotional lability and characteristics of obsessive-compulsive disorder. Dysarthria and dysgraphia are also frequently noted.[46] A physical examination findings characteristic for SC is the “milkmaid's sign,” where a patient cannot maintain her grip when asked to squeeze the examiner’s fingers due to intermittent loss of muscle contraction, leading to a squeeze-and-release motion. Patients with SC often lack the traditional dermatologic and joint manifestations of ARF.
Evaluation
Revised Jones Criteria
The diagnosis of ARF is mainly clinical and considered when a GAS infection is followed by the clinical manifestations outlined in the Revised Jones Criteria. In this classification scheme, low-risk populations have an ARF incidence of ≤2 per 100,000 school-aged children, and moderate- and high-risk populations have an ARF incidence of >2 per 100,000.[45]
The presence of 2 major criteria or 1 major and 2 minor criteria is required for the diagnosis of an initial episode of ARF in any risk population. The diagnosis of a recurrent episode of ARF requires 2 major criteria, 1 major and 2 minor criteria, or 3 minor criteria (see Table 1).[45]
A presumptive diagnosis of ARF may be made without using the Jones Criteria in patients presenting with SC or indolent carditis months after GAS infection. These cases require further evaluation with an echocardiogram.
A possible case can be defined as patients who meet the criteria for an initial infection but lack evidence of preceding GAS infection. Patients with 1 major and 1 minor criteria with evidence of a preceding GAS infection are also labeled as possible cases of ARF.[47]
Table 1. Revised Jones Criteria for Diagnosing Acute Rheumatic Fever
|
|
Low-risk population |
Moderate- and high-risk populations |
|
Major Criteria |
Carditis (clinical or subclinical) |
Carditis (clinical or subclinical) |
|
|
Polyarthritis |
Monoarthritis, polyarthritis, or polyarthralgia |
|
|
Chorea |
Chorea |
|
|
Subcutaneous nodules |
Subcutaneous nodules |
|
|
Erythema marginatum |
Erythema marginatum |
|
Minor Criteria |
Polyarthralgia |
Monoarthralgia |
|
|
Fever ≥38.5° C |
Fever ≥38°C |
|
|
ESR >60 mm/h and/or CRP >3.0 mg/dL |
ESR >30 mm/h and/or CRP >3.0 mg/dL |
|
|
ECG with prolonged PR interval |
ECG with prolonged PR interval |
|
ESR = erythrocyte sedimentation rate; CRP = C-reactive protein |
Detecting group A Streptococcus
The number of laboratory tests available to diagnose GAS infection has vastly increased. Throat culture remains the gold standard, but its use is limited by its time to result. Point-of-care testing is frequently used in primary care settings. Nucleic acid amplification tests (NAAT) detect GAS and normally result in less than 1 hour. NAATs for GAS a highly sensitive and do not require backup culture testing when negative.[48][49] Rapid antigen detection tests (RADT) identify the presence of the Lancefield group A carbohydrate, provide very rapid results, and are inexpensive. The sensitivity of RADT may be less than 90%; most experts recommend backup throat culture for negative RADT results due to the low sensitivity.[50] Neither the NAAT nor the RADT allows for detecting emm types or antimicrobial susceptibility if those are the goals of obtaining a test.
Laboratory testing to assess for a recent past GAS infection may be performed using serology. Antistreptolysin O (ASO) or antideoxyribonuclease B (ADB) antibody titers are most commonly utilized. These titers usually rise 2 to 3 weeks after a GAS infection. The interpretation of titer results is age dependent (see Table 2).[51]
Table 2. Age-dependent Upper Normal Limits for Antistreptolysin O and Antideoxyribonuclease B Antibody Titers
| Upper Normal Limit (IU) | Upper Normal Limit (IU) | |
| Age, y | Antistreptolysion O titer | Antideoxyribonuclease B titer |
| 1-4 | 170 | 366 |
| 5-14 | 276 | 499 |
| 15-24 | 238 | 473 |
| 25-34 | 177 | 390 |
| 35+ | 127 | 265 |
Cardiac Evaluation
All patients with ARF should undergo cardiac evaluation with chest radiography, electrocardiography (ECG), and echocardiography. Chest imaging may reveal cardiomegaly and pulmonary edema. The most common ECG finding is a prolongation of the PR interval, which must be adjusted for age (see Table 3).
Table 3. Age-adjusted PR Intervals
| Age, y | Duration, s |
| 3-12 | 0.16 |
| 12-16 | 0.18 |
| 17+ | 0.20 |
An echocardiogram may reveal signs of valvulopathy or heart failure. One of the keys to the successful treatment of ARF is the ability to diagnose subclinical carditis, which relies on the accessibility of echocardiography. One recent study suggested that 10.8% of patients with ARF suffer from subclinical carditis diagnosed only by echocardiography.[8] The expansion of mobile echocardiography has resulted in a vast improvement in the diagnosis of carditis and should be sought even in resource-limited settings.
Treatment / Management
The treatment of ARF is multimodal and involves GAS eradication therapy, symptomatic treatment, and prophylaxis to prevent recurrence. The initial management of ARF should occur in an inpatient hospital setting. The trend of inflammatory markers helps monitor disease progression. The normalization of inflammatory markers after completion of therapy indicates disease resolution.
Group A Streptococcus Eradication Therapy
All patients diagnosed with GAS pharyngitis should receive antibiotics to treat and attempt to eradicate GAS. Similarly, all patients diagnosed with ARF should receive a course of antibiotics even if they have a negative throat culture.[52] (B2)
The recommended antibiotic for GAS eradication therapy is penicillin; dosage is based on the patient's weight.[50] If the patient weighs less than 27kg, penicillin V 250 mg 2 to 3 times daily for 10 days is preferred; if the patient weighs more than 27kg, 500 mg 2 to 3 times daily for 10 days is recommended. A single intramuscular dose of penicillin G benzathine 600,000 units (if below 27 kg) or 1.2 million units (if above 27 kg) may also be used for GAS eradication therapy and may be preferable, as it is the recommended therapy for patients with ARF requiring secondary antibiotic prophylaxis. Amoxicillin has a slightly broader spectrum of antimicrobial activity but some practitioners prefer it for its palatability. The amoxicillin dose is 50 mg/kg/d orally for 10 days, administered once or twice daily.(A1)
Cephalosporins are recommended in cases of documented penicillin allergy with a history of anaphylaxis.[50] The most common cephalosporins administered are cephalexin, cefuroxime, cefpodoxime, or cefdinir. Macrolides are recommended when there is history of anaphylaxis to penicillin. Common macrolides administered are azithromycin at 12 mg/kg/d for 5 days with a maximum dose of 500 mg/dose and clarithromycin at 7.5 mg/kg/dose, twice daily for 10 days with a maximum dose of 250 mg/dose. There is evidence of increasing GAS resistance to macrolides.[53] Macrolide resistance is often regional and fluctuates depending on the clone of GAS circulating through a community. Clindamycin is another alternative; some have touted it as the best at eradicating the GAS carrier state. However, clindamycin has significantly more gastrointestinal adverse effects.[54](A1)
Symptomatic Therapy
Symptomatic therapy is geared toward managing the manifestations of ARF.
Arthritis is the earliest and most common manifestation of ARF and historically has been managed with aspirin 60 to 100 mg/kg/day in divided doses until symptom resolution. However, this dosing regimen required frequent measurement of serum salicylate levels and subsequent dose adjustments while increasing the risk of developing Reye syndrome. Newer data suggest that initially treating arthritis with nonsteroidal anti-inflammatory drugs (NSAIDs), typically naproxen 5 to 10 mg/kg every 12 hours with a maximum daily dose of 1000 mg until symptoms resolve, is equally effective.[55][56] One recent study suggests that ibuprofen may be equally effective.[57] The major adverse effect of NSAID therapy is gastrointestinal upset; patients are often prescribed a concurrent proton-pump inhibitor. Glucocorticoids are recommended if the patient has an allergy to aspirin or NSAIDs.(A1)
Carditis is the most serious complication of ARF, and GAS eradication therapy removes the infection inducing the autoimmune response against cardiac tissues. Decreasing systemic inflammation has been associated with reducing the risk of developing cardiac disease. A recent systematic review assessed various therapies for carditis and their ability to prevent further cardiac damage. In summary, neither corticosteroids nor intravenous immunoglobulin (IVIG) were determined superior to aspirin therapy for this purpose.[58] Corticosteroids may help manage patients with severe acute rheumatic heart disease, marked by significant mitral regurgitation or persistent atrioventricular block.[59] (A1)
If a patient develops heart failure or RHD, treatment can be pharmacological or surgical, depending on the severity of the cardiac disease. Pharmacotherapy options recommended for managing heart failure include fluid and salt restriction, angiotensin-converting enzyme (ACE) inhibitors, and diuretics.[42] All patients with ARF should be evaluated and followed by a cardiologist, even if carditis is not initially present, and undergo periodic evaluation to monitor for potential progression to RHD.
Subcutaneous nodules and erythema marginatum associated with ARF are commonly self-limited.
Sydenham chorea (SC) is a late-stage finding and is generally self-limited. SC is treated with rest and avoidance of overstimulation. Immunomodulating agents have been studied as a treatment for SC and appear to have a positive impact. Studies suggest that corticosteroids will improve symptoms in patients suffering from SC. The most common treatment regimen is intravenous methylprednisolone, followed by oral prednisone.[60][61][62] Some practitioners advocate for treatment with prednisone alone.[63][64][65][66] Others have observed that patients demonstrate clinical improvement after receiving IVIG or plasmapheresis therapy.[67][68][69][60]][70](A1)
Pharmacotherapy is recommended for SC which is negatively impacting activities of daily living. Options include carbamazepine, pimozide, haloperidol, and valproic acid for refractory cases. Haloperidol has shown efficacy, but its significant adverse effects limit its use in children.[71][72] Carbamazepine and valproic acid are effective against the symptoms of SC and have been used in children with neurologic diseases for many years.[73][74] One case report suggests that pimozide may be effective with minimal adverse effects.[75](B3)
Secondary Antibiotic Prophylaxis
Patients with a history of ARF are at increased risk for disease recurrence and worsening RHD and should receive secondary antibiotic prophylaxis against GAS infections. Patients with SC as the only presenting symptom of ARF should also initiate secondary antibiotic prophylaxis.
Antibiotic prophylaxis typically involves the administration of intramuscular penicillin G benzathine every 28 days. In populations with a higher incidence of ARF, injections should be administered every 21 days. Oral penicillin V twice daily may be used prophylactically but is associated with decreased adherence and increased recurrence.[76] However, penicillin V is the recommended prophylactic therapy in patients with severe, symptomatic valvular disease with evidence of significant heart failure, as vasovagal episodes associated with intramuscular injections have been associated with an increased risk of sudden death. In patients with penicillin allergies, macrolides and sulfadiazines can be used. All patients with a history of penicillin allergy should undergo evaluation by an allergist to determine if they can be cleared for penicillin therapy. In cases of breakthrough GAS pharyngitis, clindamycin can be used for the acute episode before restarting penicillin prophylaxis.
The duration of secondary prophylactic therapy may vary based on evidence of carditis. Patients with echocardiographic evidence of carditis without residual valvulopathy should continue prophylactic therapy for 10 years or until age 21. Patients with evidence of residual valvulopathy should continue prophylactic therapy for 10 years or until age 40. If there is no echocardiographic evidence of carditis, prophylaxis should continue for 5 years or until the patient reaches age 21. In all cases, prophylactic therapy should be continued until the latest age criteria are met (see Table 4).[52] (B2)
Table 4. Secondary Antibiotic Prophylaxis of Acute Rheumatic Fever
| Level of carditis | Duration of antimicrobial prophylaxis |
| Carditis and detectably persistent heart disease | 10 y from the last episode of ARF or until age 40 y, whichever is longer |
| Carditis without detectably persistent heart disease | 10 y from the last episode of ARF or until age 21 y, whichever is longer |
| No evidence of carditis | 5 y from the last episode of ARF or until age 21 y, whichever is longer |
Differential Diagnosis
Patients with ARF may present with one or more clinical symptoms. The presentation of ARF varies widely. The differential diagnosis of ARF is broad and will be dictated by the presenting symptomatology. Diagnoses that may be considered include:
- Polyarthritis:
- Lyme disease
- Poststreptococcal reactive arthritis
- Septic arthritis
- Drug reactions and serum sickness
- Postinfectious reactive arthritis
- Carditis:
- Endocarditis
- Viral myocarditis
- Sydenham Chorea:
- Pediatric autoimmune neuropsychiatric disorders associated with streptococcal infections (PANDAS)
- Tardive dyskinesia
- Tourette syndrome
- Dermatologic manifestations:
- Urticaria
- Scarlet fever
- Kawasaki disease
- Erythema multiforme
- Erythema migrans (Lyme disease)
- Viral exanthem
- Systemic Illnesses
- Juvenile idiopathic arthritis
- Kawasaki disease
- Systemic lupus erythematosus
Prognosis
The usual course of ARF is about 3 months, and recurrence rates approximate 65%.[77] Recurrence increases the risk of progression to RHD and heart failure. Risk factors contributing to recurrence include poor adherence to prophylaxis, shorter intervals between episodes of ARF, younger age, and the presence of carditis.[78]
Cardiac involvement is the most critical prognosticating factor in ARF. Patients with carditis are at the highest risk for developing RHD, the most common cause of morbidity and mortality in patients with ARF. The long-term prognosis of ARF has significantly improved over the last century in developed areas with enhanced therapy for GAS eradication, long-term secondary prophylaxis, and improvement in living conditions. Despite this, it is very common for patients in resource-poor areas to present with late-stage RHD. Valve replacement or valvuloplasty is indicated in cases of severe rheumatic valvular disease.
A study conducted on Australian patients with cardiac disease during their ARF episode showed that 50% of patients with severe RHD underwent valvular surgery within 2 years and experienced a 10% mortality rate. Among patients with minimal carditis, 64% had mild cardiac disease even after 10 years of developing ARF. Of these patients, 11.4% progressed to clinically severe RHD, and half needed surgery.[79]
A systematic review recently summarized the outcomes of mitral valvuloplasty versus mitral valve replacement. Patients who underwent valve repair were noted to have lower short- and long-term mortality but often required additional procedures. Surgical repair is preferred for older patients, but concomitant aortic valve disease favors mitral valve replacement.[80]
Sydenham chorea (SC) typically will resolve in about 12-15 weeks. Persistent SC does occur, but the mechanism is unclear. Some experts suspect damage to the basal ganglia accounts for this phenomenon.[81] Additionally, psychiatric symptoms may be more prevalent in patients who have suffered from SC.[82]
Complications
The most common complicating sequela of ARF is RHD, which occurs 10 to 20 years after the original illness and is due to valvular damage by severe or recurrent bouts of ARF. RHD is the most common cause of acquired valvular pathology worldwide. RHD can lead to heart failure, pulmonary hypertension, dysrhythmias, embolic strokes, and sudden cardiac death.[83]
Another complication of ARF is Jaccuod arthropathy, a chronic, benign arthropathy that may result in joint deformities due to repeated bouts of arthritis caused by ARF.[84] The arthritic changes of Jaccoud arthropathy appear similar to the joint deformities seen with rheumatoid arthritis and include thumb subluxation, ulnar deviation, hallux valgus, and swan neck and boutonniere deformities of the fingers. However, unlike in rheumatoid arthritis, patients with Jaccoud arthropathy do not have bony erosions, and the deformations can be manipulated into a normal anatomic position.
SC may rarely lead to persistent symptoms and has been related to increased psychiatric symptoms in some patients.
Consultations
Care for patients with ARF should be carried out in consultation with an infectious disease specialist and a cardiologist. As part of the diagnostic criteria, it will be necessary to obtain echocardiography to look for evidence of carditis. If patients develop carditis with severe valvulopathy with signs of heart failure, a cardiothoracic surgeon should be consulted to consider valvuloplasty. In patients with SC, consultation with a neurologist may be necessary. In patients with persistent arthralgias and arthritis, consultation with a rheumatologist may help design a long-term management plan.
Deterrence and Patient Education
ARF and the subsequent development of RHD are significant causes of morbidity and mortality, especially in developing countries. Deterrence involves strategies to avoid GAS pharyngitis, early detection and treatment of GAS pharyngitis, and prophylaxis against recurrent ARF. Patient education is one of the cornerstones of successful lifelong management of ARF. Patients should be informed about the consequences of their diagnosis of ARF and the importance of adherence to prophylactic antibiotic therapy. Caregivers should also be educated about the signs of GAS pharyngitis and early manifestations of acute rheumatic fever. Household and school-aged contacts are the most likely sources of GAS exposure in people with a history of ARF.
Enhancing Healthcare Team Outcomes
The presentation and severity of ARF varies significantly. Recurrence is frequent and may be challenging to manage. Patients with ARF benefit from a multidisciplinary, interprofessional team approach.
Primary care practitioners and urgent or emergency care clinicians are frequently the first medical contacts of patients with ARF. Recognition of the early clinical symptoms and signs is imperative to improve outcomes for patients with ARF. Prompt initiation of pharmacotherapy and early cardiac assessment is essential when evaluating and treating patients with ARF.
If the patient evaluation reveals signs of carditis or RHD, cardiologists and cardiothoracic surgeons should primarily manage the symptoms of heart failure and valvulopathies. Consultation with an infectious disease specialist is crucial to help guide the initial treatment and secondary prophylactic therapy of ARF. A statement by the American Heart Association and endorsed by the American Academy of Pediatrics confirms that penicillin G is the most studied pharmacotherapy in the prevention of the recurrence of acute rheumatic fever, and continuous prophylaxis is the most strongly recommended intervention for those with a history of acute rheumatic fever.[52]
All clinicians caring for patients with ARF are responsible for educating patients on the importance of adherence to pharmacotherapy and secondary antibiotic prophylaxis.
Media
(Click Image to Enlarge)
References
Karthikeyan G, Guilherme L. Acute rheumatic fever. Lancet (London, England). 2018 Jul 14:392(10142):161-174. doi: 10.1016/S0140-6736(18)30999-1. Epub 2018 Jun 29 [PubMed PMID: 30025809]
Zühlke LJ, Steer AC. Estimates of the global burden of rheumatic heart disease. Global heart. 2013 Sep:8(3):189-95. doi: 10.1016/j.gheart.2013.08.008. Epub 2013 Sep 26 [PubMed PMID: 25690495]
GBD 2013 Mortality and Causes of Death Collaborators. Global, regional, and national age-sex specific all-cause and cause-specific mortality for 240 causes of death, 1990-2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet (London, England). 2015 Jan 10:385(9963):117-71. doi: 10.1016/S0140-6736(14)61682-2. Epub 2014 Dec 18 [PubMed PMID: 25530442]
Level 1 (high-level) evidenceWebb RH, Grant C, Harnden A. Acute rheumatic fever. BMJ (Clinical research ed.). 2015 Jul 14:351():h3443. doi: 10.1136/bmj.h3443. Epub 2015 Jul 14 [PubMed PMID: 26175053]
Cunningham MW. Rheumatic fever, autoimmunity, and molecular mimicry: the streptococcal connection. International reviews of immunology. 2014 Jul-Aug:33(4):314-29. doi: 10.3109/08830185.2014.917411. Epub 2014 Jun 3 [PubMed PMID: 24892819]
Level 3 (low-level) evidenceBennett J, Moreland NJ, Oliver J, Crane J, Williamson DA, Sika-Paotonu D, Harwood M, Upton A, Smith S, Carapetis J, Baker MG. Understanding group A streptococcal pharyngitis and skin infections as causes of rheumatic fever: protocol for a prospective disease incidence study. BMC infectious diseases. 2019 Jul 17:19(1):633. doi: 10.1186/s12879-019-4126-9. Epub 2019 Jul 17 [PubMed PMID: 31315580]
Level 3 (low-level) evidenceParks T, Smeesters PR, Steer AC. Streptococcal skin infection and rheumatic heart disease. Current opinion in infectious diseases. 2012 Apr:25(2):145-53. doi: 10.1097/QCO.0b013e3283511d27. Epub [PubMed PMID: 22327467]
Level 3 (low-level) evidenceMcDonald M, Currie BJ, Carapetis JR. Acute rheumatic fever: a chink in the chain that links the heart to the throat? The Lancet. Infectious diseases. 2004 Apr:4(4):240-5 [PubMed PMID: 15050943]
Carapetis JR. Rheumatic heart disease in developing countries. The New England journal of medicine. 2007 Aug 2:357(5):439-41 [PubMed PMID: 17671252]
Markowitz M. Eradication of rheumatic fever: an unfulfilled hope. Circulation. 1970 Jun:41(6):1077-84 [PubMed PMID: 5482905]
Stewart T, McDonald R, Currie B. Acute rheumatic fever: adherence to secondary prophylaxis and follow up of Indigenous patients in the Katherine region of the Northern Territory. The Australian journal of rural health. 2007 Aug:15(4):234-40 [PubMed PMID: 17617086]
Level 2 (mid-level) evidenceLahiri S, Sanyahumbi A. Acute Rheumatic Fever. Pediatrics in review. 2021 May:42(5):221-232. doi: 10.1542/pir.2019-0288. Epub [PubMed PMID: 33931507]
Negi PC, Kandoria A, Asotra S, Ganju NK, Merwaha R, Sharma R, Mahajan K, Rao S. Gender differences in the epidemiology of Rheumatic Fever/Rheumatic heart disease (RF/RHD) patient population of hill state of northern India; 9 years prospective hospital based, HP-RHD registry. Indian heart journal. 2020 Nov-Dec:72(6):552-556. doi: 10.1016/j.ihj.2020.09.011. Epub 2020 Sep 18 [PubMed PMID: 33357644]
Noonan S, Zurynski YA, Currie BJ, McDonald M, Wheaton G, Nissen M, Curtis N, Isaacs D, Richmond P, Ramsay JM, Elliott EJ, Carapetis JR. A national prospective surveillance study of acute rheumatic fever in Australian children. The Pediatric infectious disease journal. 2013 Jan:32(1):e26-32. doi: 10.1097/INF.0b013e31826faeb3. Epub [PubMed PMID: 22926211]
Parnaby MG, Carapetis JR. Rheumatic fever in indigenous Australian children. Journal of paediatrics and child health. 2010 Sep:46(9):527-33. doi: 10.1111/j.1440-1754.2010.01841.x. Epub [PubMed PMID: 20854325]
Miyake CY, Gauvreau K, Tani LY, Sundel RP, Newburger JW. Characteristics of children discharged from hospitals in the United States in 2000 with the diagnosis of acute rheumatic fever. Pediatrics. 2007 Sep:120(3):503-8 [PubMed PMID: 17766522]
Global Burden of Disease Study 2013 Collaborators. Global, regional, and national incidence, prevalence, and years lived with disability for 301 acute and chronic diseases and injuries in 188 countries, 1990-2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet (London, England). 2015 Aug 22:386(9995):743-800. doi: 10.1016/S0140-6736(15)60692-4. Epub 2015 Jun 7 [PubMed PMID: 26063472]
Level 1 (high-level) evidenceTibazarwa KB, Volmink JA, Mayosi BM. Incidence of acute rheumatic fever in the world: a systematic review of population-based studies. Heart (British Cardiac Society). 2008 Dec:94(12):1534-40. doi: 10.1136/hrt.2007.141309. Epub 2008 Jul 31 [PubMed PMID: 18669552]
Level 2 (mid-level) evidenceShulman ST, Stollerman G, Beall B, Dale JB, Tanz RR. Temporal changes in streptococcal M protein types and the near-disappearance of acute rheumatic fever in the United States. Clinical infectious diseases : an official publication of the Infectious Diseases Society of America. 2006 Feb 15:42(4):441-7 [PubMed PMID: 16421785]
Bessen DE, Sotir CM, Readdy TL, Hollingshead SK. Genetic correlates of throat and skin isolates of group A streptococci. The Journal of infectious diseases. 1996 Apr:173(4):896-900 [PubMed PMID: 8603968]
Lee GM, Wessels MR. Changing epidemiology of acute rheumatic fever in the United States. Clinical infectious diseases : an official publication of the Infectious Diseases Society of America. 2006 Feb 15:42(4):448-50 [PubMed PMID: 16421786]
Kaplan EL, Johnson DR, Cleary PP. Group A streptococcal serotypes isolated from patients and sibling contacts during the resurgence of rheumatic fever in the United States in the mid-1980s. The Journal of infectious diseases. 1989 Jan:159(1):101-3 [PubMed PMID: 2642516]
Quinn A, Kosanke S, Fischetti VA, Factor SM, Cunningham MW. Induction of autoimmune valvular heart disease by recombinant streptococcal m protein. Infection and immunity. 2001 Jun:69(6):4072-8 [PubMed PMID: 11349078]
Level 3 (low-level) evidencevan de Rijn I, Zabriskie JB, McCarty M. Group A streptococcal antigens cross-reactive with myocardium. Purification of heart-reactive antibody and isolation and characterization of the streptococcal antigen. The Journal of experimental medicine. 1977 Aug 1:146(2):579-99 [PubMed PMID: 327018]
Level 3 (low-level) evidenceRoberts S, Kosanke S, Terrence Dunn S, Jankelow D, Duran CM, Cunningham MW. Pathogenic mechanisms in rheumatic carditis: focus on valvular endothelium. The Journal of infectious diseases. 2001 Feb 1:183(3):507-11 [PubMed PMID: 11133385]
Kirvan CA, Swedo SE, Heuser JS, Cunningham MW. Mimicry and autoantibody-mediated neuronal cell signaling in Sydenham chorea. Nature medicine. 2003 Jul:9(7):914-20 [PubMed PMID: 12819778]
Karalok ZS, Öztürk Z, Gunes A, Gurkas E. Sydenham Chorea: Putaminal Enlargement. Journal of child neurology. 2021 Jan:36(1):48-53. doi: 10.1177/0883073820951364. Epub 2020 Aug 27 [PubMed PMID: 32851928]
Shikhman AR, Cunningham MW. Immunological mimicry between N-acetyl-beta-D-glucosamine and cytokeratin peptides. Evidence for a microbially driven anti-keratin antibody response. Journal of immunology (Baltimore, Md. : 1950). 1994 May 1:152(9):4375-87 [PubMed PMID: 7512592]
Level 3 (low-level) evidenceBryant PA, Robins-Browne R, Carapetis JR, Curtis N. Some of the people, some of the time: susceptibility to acute rheumatic fever. Circulation. 2009 Feb 10:119(5):742-53. doi: 10.1161/CIRCULATIONAHA.108.792135. Epub [PubMed PMID: 19204317]
Engel ME, Stander R, Vogel J, Adeyemo AA, Mayosi BM. Genetic susceptibility to acute rheumatic fever: a systematic review and meta-analysis of twin studies. PloS one. 2011:6(9):e25326. doi: 10.1371/journal.pone.0025326. Epub 2011 Sep 30 [PubMed PMID: 21980428]
Level 1 (high-level) evidenceGuilherme L, Ramasawmy R, Kalil J. Rheumatic fever and rheumatic heart disease: genetics and pathogenesis. Scandinavian journal of immunology. 2007 Aug-Sep:66(2-3):199-207 [PubMed PMID: 17635797]
Level 3 (low-level) evidenceCarapetis JR, Beaton A, Cunningham MW, Guilherme L, Karthikeyan G, Mayosi BM, Sable C, Steer A, Wilson N, Wyber R, Zühlke L. Acute rheumatic fever and rheumatic heart disease. Nature reviews. Disease primers. 2016 Jan 14:2():15084. doi: 10.1038/nrdp.2015.84. Epub 2016 Jan 14 [PubMed PMID: 27188830]
Gray LA, D'Antoine HA, Tong SYC, McKinnon M, Bessarab D, Brown N, Reményi B, Steer A, Syn G, Blackwell JM, Inouye M, Carapetis JR. Genome-Wide Analysis of Genetic Risk Factors for Rheumatic Heart Disease in Aboriginal Australians Provides Support for Pathogenic Molecular Mimicry. The Journal of infectious diseases. 2017 Dec 12:216(11):1460-1470. doi: 10.1093/infdis/jix497. Epub [PubMed PMID: 29029143]
Parks T, Mirabel MM, Kado J, Auckland K, Nowak J, Rautanen A, Mentzer AJ, Marijon E, Jouven X, Perman ML, Cua T, Kauwe JK, Allen JB, Taylor H, Robson KJ, Deane CM, Steer AC, Hill AVS, Pacific Islands Rheumatic Heart Disease Genetics Network. Association between a common immunoglobulin heavy chain allele and rheumatic heart disease risk in Oceania. Nature communications. 2017 May 11:8():14946. doi: 10.1038/ncomms14946. Epub 2017 May 11 [PubMed PMID: 28492228]
Tandon R, Sharma M, Chandrashekhar Y, Kotb M, Yacoub MH, Narula J. Revisiting the pathogenesis of rheumatic fever and carditis. Nature reviews. Cardiology. 2013 Mar:10(3):171-7. doi: 10.1038/nrcardio.2012.197. Epub 2013 Jan 15 [PubMed PMID: 23319102]
Level 3 (low-level) evidenceMutithu DW, Roberts R, Manganyi R, Ntusi NAB. Chronic rheumatic heart disease with recrudescence of acute rheumatic fever on histology: a case report. European heart journal. Case reports. 2022 Jul:6(7):ytac278. doi: 10.1093/ehjcr/ytac278. Epub 2022 Jul 5 [PubMed PMID: 35865226]
Level 3 (low-level) evidenceTroyer C, Grossman ME, Silvers DN. Erythema marginatum in rheumatic fever: early diagnosis by skin biopsy. Journal of the American Academy of Dermatology. 1983 May:8(5):724-8 [PubMed PMID: 6863635]
Level 3 (low-level) evidenceBenedek TG. Subcutaneous nodules and the differentiation of rheumatoid arthritis from rheumatic fever. Seminars in arthritis and rheumatism. 1984 May:13(4):305-21 [PubMed PMID: 6374898]
Gordis L. Effectiveness of comprehensive-care programs in preventing rheumatic fever. The New England journal of medicine. 1973 Aug 16:289(7):331-5 [PubMed PMID: 4740466]
Mustafa Z, Ghaffari M. Diagnostic Methods, Clinical Guidelines, and Antibiotic Treatment for Group A Streptococcal Pharyngitis: A Narrative Review. Frontiers in cellular and infection microbiology. 2020:10():563627. doi: 10.3389/fcimb.2020.563627. Epub 2020 Oct 15 [PubMed PMID: 33178623]
Level 3 (low-level) evidenceAbernethy M, Bass N, Sharpe N, Grant C, Neutze J, Clarkson P, Greaves S, Lennon D, Snow S, Whalley G. Doppler echocardiography and the early diagnosis of carditis in acute rheumatic fever. Australian and New Zealand journal of medicine. 1994 Oct:24(5):530-5 [PubMed PMID: 7848157]
Dass C, Kanmanthareddy A. Rheumatic Heart Disease. StatPearls. 2024 Jan:(): [PubMed PMID: 30855870]
Tani LY, Veasy LG, Minich LL, Shaddy RE. Rheumatic fever in children younger than 5 years: is the presentation different? Pediatrics. 2003 Nov:112(5):1065-8 [PubMed PMID: 14595047]
Level 2 (mid-level) evidenceEshel G, Lahat E, Azizi E, Gross B, Aladjem M. Chorea as a manifestation of rheumatic fever--a 30-year survey (1960-1990). European journal of pediatrics. 1993 Aug:152(8):645-6 [PubMed PMID: 8404967]
Level 2 (mid-level) evidenceGewitz MH, Baltimore RS, Tani LY, Sable CA, Shulman ST, Carapetis J, Remenyi B, Taubert KA, Bolger AF, Beerman L, Mayosi BM, Beaton A, Pandian NG, Kaplan EL, American Heart Association Committee on Rheumatic Fever, Endocarditis, and Kawasaki Disease of the Council on Cardiovascular Disease in the Young. Revision of the Jones Criteria for the diagnosis of acute rheumatic fever in the era of Doppler echocardiography: a scientific statement from the American Heart Association. Circulation. 2015 May 19:131(20):1806-18. doi: 10.1161/CIR.0000000000000205. Epub 2015 Apr 23 [PubMed PMID: 25908771]
Orsini A, Foiadelli T, Magistrali M, Carli N, Bagnasco I, Dassi P, Verrotti A, Marcotulli D, Canavese C, Nicita F, Capuano A, Marra C, Fetta A, Nosadini M, Sartori S, Papa A, Viri M, Greco F, Pavone P, Simonini G, Matricardi S, Siquilini S, Marchese F, De Grandis E, Brunenghi BM, Malattia C, Bassanese F, Bergonzini P, Bonuccelli A, Consolini R, Marseglia GL, Peroni D, Striano P, Cordelli D, Savasta S. A nationwide study on Sydenham's chorea: Clinical features, treatment and prognostic factors. European journal of paediatric neurology : EJPN : official journal of the European Paediatric Neurology Society. 2022 Jan:36():1-6. doi: 10.1016/j.ejpn.2021.11.002. Epub 2021 Nov 6 [PubMed PMID: 34768201]
Scheel A, Beaton AZ, Katzenellenbogen J, Parks T, Miller KM, Cherian T, Van Beneden CA, Cannon JW, Moore HC, Bowen AC, Carapetis JR. Standardization of Epidemiological Surveillance of Acute Rheumatic Fever(). Open forum infectious diseases. 2022 Sep:9(Suppl 1):S41-S49. doi: 10.1093/ofid/ofac252. Epub 2022 Sep 15 [PubMed PMID: 36128408]
Level 2 (mid-level) evidenceDubois C, Smeesters PR, Refes Y, Levy C, Bidet P, Cohen R, Chalumeau M, Toubiana J, Cohen JF. Diagnostic accuracy of rapid nucleic acid tests for group A streptococcal pharyngitis: systematic review and meta-analysis. Clinical microbiology and infection : the official publication of the European Society of Clinical Microbiology and Infectious Diseases. 2021 Dec:27(12):1736-1745. doi: 10.1016/j.cmi.2021.04.021. Epub 2021 May 6 [PubMed PMID: 33964409]
Level 1 (high-level) evidenceLean WL, Arnup S, Danchin M, Steer AC. Rapid diagnostic tests for group A streptococcal pharyngitis: a meta-analysis. Pediatrics. 2014 Oct:134(4):771-81. doi: 10.1542/peds.2014-1094. Epub 2014 Sep 8 [PubMed PMID: 25201792]
Level 1 (high-level) evidenceShulman ST, Bisno AL, Clegg HW, Gerber MA, Kaplan EL, Lee G, Martin JM, Van Beneden C. Clinical practice guideline for the diagnosis and management of group A streptococcal pharyngitis: 2012 update by the Infectious Diseases Society of America. Clinical infectious diseases : an official publication of the Infectious Diseases Society of America. 2012 Nov 15:55(10):1279-82. doi: 10.1093/cid/cis847. Epub [PubMed PMID: 23091044]
Level 1 (high-level) evidenceSteer AC, Vidmar S, Ritika R, Kado J, Batzloff M, Jenney AW, Carlin JB, Carapetis JR. Normal ranges of streptococcal antibody titers are similar whether streptococci are endemic to the setting or not. Clinical and vaccine immunology : CVI. 2009 Feb:16(2):172-5. doi: 10.1128/CVI.00291-08. Epub 2008 Dec 3 [PubMed PMID: 19052157]
Gerber MA, Baltimore RS, Eaton CB, Gewitz M, Rowley AH, Shulman ST, Taubert KA. Prevention of rheumatic fever and diagnosis and treatment of acute Streptococcal pharyngitis: a scientific statement from the American Heart Association Rheumatic Fever, Endocarditis, and Kawasaki Disease Committee of the Council on Cardiovascular Disease in the Young, the Interdisciplinary Council on Functional Genomics and Translational Biology, and the Interdisciplinary Council on Quality of Care and Outcomes Research: endorsed by the American Academy of Pediatrics. Circulation. 2009 Mar 24:119(11):1541-51. doi: 10.1161/CIRCULATIONAHA.109.191959. Epub 2009 Feb 26 [PubMed PMID: 19246689]
Level 2 (mid-level) evidenceBrouwer S, Rivera-Hernandez T, Curren BF, Harbison-Price N, De Oliveira DMP, Jespersen MG, Davies MR, Walker MJ. Pathogenesis, epidemiology and control of Group A Streptococcus infection. Nature reviews. Microbiology. 2023 Jul:21(7):431-447. doi: 10.1038/s41579-023-00865-7. Epub 2023 Mar 9 [PubMed PMID: 36894668]
Tanz RR, Poncher JR, Corydon KE, Kabat K, Yogev R, Shulman ST. Clindamycin treatment of chronic pharyngeal carriage of group A streptococci. The Journal of pediatrics. 1991 Jul:119(1 Pt 1):123-8 [PubMed PMID: 2066844]
Level 1 (high-level) evidenceHashkes PJ, Tauber T, Somekh E, Brik R, Barash J, Mukamel M, Harel L, Lorber A, Berkovitch M, Uziel Y, Pediatric Rheumatlogy Study Group of Israel. Naproxen as an alternative to aspirin for the treatment of arthritis of rheumatic fever: a randomized trial. The Journal of pediatrics. 2003 Sep:143(3):399-401 [PubMed PMID: 14517527]
Level 1 (high-level) evidenceÇetin İİ, Ekici F, Kocabaş A, Çevik BŞ, Eminoğlu S, Azak E, Kibar AE, Arı ME, Sürücü M, Orgun A. The efficacy and safety of naproxen in acute rheumatic fever: The comparative results of 11-year experience with acetylsalicylic acid and naproxen. The Turkish journal of pediatrics. 2016:58(5):473-479. doi: 10.24953/turkjped.2016.05.003. Epub [PubMed PMID: 28621087]
Level 2 (mid-level) evidenceYılmaz M, Gürses D, Tükenmez G. The effectiveness and safety of ibuprofen and acetylsalicylic acid in acute rheumatic fever. Pediatrics international : official journal of the Japan Pediatric Society. 2022 Jan:64(1):e15133. doi: 10.1111/ped.15133. Epub [PubMed PMID: 35704468]
Cilliers A, Adler AJ, Saloojee H. Anti-inflammatory treatment for carditis in acute rheumatic fever. The Cochrane database of systematic reviews. 2015 May 28:(5):CD003176. doi: 10.1002/14651858.CD003176.pub3. Epub 2015 May 28 [PubMed PMID: 26017576]
Level 1 (high-level) evidenceTorres RPA, Torres RFA, Torres RA, Torres RSLA. Pulse therapy combined with oral corticosteroids in the management of severe rheumatic carditis and rebound. Cardiology in the young. 2018 Feb:28(2):309-314. doi: 10.1017/S1047951117002062. Epub 2017 Oct 25 [PubMed PMID: 29065944]
Miranda M, Walker RH, Saez D, Renner V. Severe Sydenham's chorea (chorea paralytica) successfully treated with plasmapheresis. Journal of clinical movement disorders. 2015:2():2. doi: 10.1186/s40734-014-0012-1. Epub 2015 Jan 21 [PubMed PMID: 26788338]
Cardoso F, Maia D, Cunningham MC, Valença G. Treatment of Sydenham chorea with corticosteroids. Movement disorders : official journal of the Movement Disorder Society. 2003 Nov:18(11):1374-7 [PubMed PMID: 14639684]
Level 3 (low-level) evidenceFusco C, Ucchino V, Frattini D, Pisani F, Della Giustina E. Acute and chronic corticosteroid treatment of ten patients with paralytic form of Sydenham's chorea. European journal of paediatric neurology : EJPN : official journal of the European Paediatric Neurology Society. 2012 Jul:16(4):373-8. doi: 10.1016/j.ejpn.2011.12.005. Epub 2011 Dec 23 [PubMed PMID: 22197452]
Paz JA, Silva CA, Marques-Dias MJ. Randomized double-blind study with prednisone in Sydenham's chorea. Pediatric neurology. 2006 Apr:34(4):264-9 [PubMed PMID: 16638499]
Level 1 (high-level) evidenceTumas V, Caldas CT, Santos AC, Nobre A, Fernandes RM. Sydenham's chorea: clinical observations from a Brazilian movement disorder clinic. Parkinsonism & related disorders. 2007 Jul:13(5):276-83 [PubMed PMID: 17240185]
Level 2 (mid-level) evidenceFaustino PC, Terreri MT, da Rocha AJ, Zappitelli MC, Lederman HM, Hilário MO. Clinical, laboratory, psychiatric and magnetic resonance findings in patients with Sydenham chorea. Neuroradiology. 2003 Jul:45(7):456-62 [PubMed PMID: 12811441]
Araujo AP, Padua PA, Maia Filho HS. Management of rheumatic chorea: an observational study. Arquivos de neuro-psiquiatria. 2002 Jun:60(2-A):231-3 [PubMed PMID: 12068350]
Level 2 (mid-level) evidenceAli A, Anugwom GO, Rehman U, Khalid MZ, Saeeduddin MO. Sydenham Chorea Managed With Immunoglobulin in Acute Rheumatic Fever. Cureus. 2021 May 12:13(5):e14990. doi: 10.7759/cureus.14990. Epub 2021 May 12 [PubMed PMID: 34131535]
Gregorowski C, Lochner C, Martin L, Simmons C, Kidd M, Walker K, Wilmshurst JM, Seedat S. Neuropsychological manifestations in children with Sydenham's chorea after adjunct intravenous immunoglobulin and standard treatment. Metabolic brain disease. 2016 Feb:31(1):205-12. doi: 10.1007/s11011-015-9681-1. Epub 2015 May 19 [PubMed PMID: 25987537]
Walker K, Brink A, Lawrenson J, Mathiassen W, Wilmshurst JM. Treatment of sydenham chorea with intravenous immunoglobulin. Journal of child neurology. 2012 Feb:27(2):147-55. doi: 10.1177/0883073811414058. Epub 2011 Aug 24 [PubMed PMID: 21868369]
Level 1 (high-level) evidenceGarvey MA, Snider LA, Leitman SF, Werden R, Swedo SE. Treatment of Sydenham's chorea with intravenous immunoglobulin, plasma exchange, or prednisone. Journal of child neurology. 2005 May:20(5):424-9 [PubMed PMID: 15968928]
Level 1 (high-level) evidenceAxley J. Rheumatic chorea controlled with haloperidol. The Journal of pediatrics. 1972 Dec:81(6):1216-7 [PubMed PMID: 4643046]
Shields WD, Bray PF. A danger of haloperidol therapy in children. The Journal of pediatrics. 1976 Feb:88(2):301-3 [PubMed PMID: 1249696]
Level 3 (low-level) evidenceHarel L, Zecharia A, Straussberg R, Volovitz B, Amir J. Successful treatment of rheumatic chorea with carbamazepine. Pediatric neurology. 2000 Aug:23(2):147-51 [PubMed PMID: 11020640]
Alvarez LA, Novak G. Valproic acid in the treatment of Sydenham chorea. Pediatric neurology. 1985 Sep-Oct:1(5):317-9 [PubMed PMID: 3939747]
Level 3 (low-level) evidenceShannon KM, Fenichel GM. Pimozide treatment of Sydenham's chorea. Neurology. 1990 Jan:40(1):186 [PubMed PMID: 2296371]
Level 3 (low-level) evidenceFEINSTEIN AR, WOOD HF, EPSTEIN JA, TARANTA A, SIMPSON R, TURSKY E. A controlled study of three methods of prophylaxis against streptococcal infection in a population of rheumatic children. II. Results of the first three years of the study, including methods for evaluating the maintenance of oral prophylaxis. The New England journal of medicine. 1959 Apr 2:260(14):697-702 [PubMed PMID: 13644570]
Hutchison SJ. Acute rheumatic fever. The Journal of infection. 1998 May:36(3):249-53 [PubMed PMID: 9661932]
. The natural history of rheumatic fever and rheumatic heart disease. Ten-year report of a cooperative clinical trial of ACTH, cortisone, and aspirin. Circulation. 1965 Sep:32(3):457-76 [PubMed PMID: 4284068]
Cannon J, Roberts K, Milne C, Carapetis JR. Rheumatic Heart Disease Severity, Progression and Outcomes: A Multi-State Model. Journal of the American Heart Association. 2017 Mar 2:6(3):. doi: 10.1161/JAHA.116.003498. Epub 2017 Mar 2 [PubMed PMID: 28255075]
Jiang Y, Wang C, Li G, Chen S. Clinical outcomes following surgical mitral valve repair or replacement in patients with rheumatic heart disease: a meta-analysis. Annals of translational medicine. 2021 Feb:9(3):204. doi: 10.21037/atm-20-3542. Epub [PubMed PMID: 33708831]
Level 1 (high-level) evidenceEmery ES, Vieco PT. Sydenham Chorea: magnetic resonance imaging reveals permanent basal ganglia injury. Neurology. 1997 Feb:48(2):531-3 [PubMed PMID: 9040753]
Level 3 (low-level) evidenceMoreira J, Kummer A, Harsányi E, Cardoso F, Teixeira AL. Psychiatric disorders in persistent and remitted Sydenham's chorea. Parkinsonism & related disorders. 2014 Feb:20(2):233-6. doi: 10.1016/j.parkreldis.2013.10.029. Epub 2013 Nov 8 [PubMed PMID: 24268384]
Marcus RH, Sareli P, Pocock WA, Barlow JB. The spectrum of severe rheumatic mitral valve disease in a developing country. Correlations among clinical presentation, surgical pathologic findings, and hemodynamic sequelae. Annals of internal medicine. 1994 Feb 1:120(3):177-83 [PubMed PMID: 8043061]
Level 2 (mid-level) evidenceChaurasia AS, Nawale JM, Patil SN, Yemul MA, Mukhedkar SM, Singh D, Patil PK, Chavan RV. Jaccoud's arthropathy. Lancet (London, England). 2013 Jun 15:381(9883):2108. doi: 10.1016/S0140-6736(12)61681-X. Epub 2013 Jan 4 [PubMed PMID: 23290493]
Level 3 (low-level) evidence