Introduction
An acute ST-elevation myocardial infarction (STEMI) is an event in which transmural myocardial ischemia results in myocardial injury or necrosis.[1] The current 2018 clinical definition of myocardial infarction (MI) requires the confirmation of the myocardial ischemic injury with abnormal cardiac biomarkers.[2] It is a clinical syndrome involving myocardial ischemia, EKG changes and chest pain.
Etiology
Register For Free And Read The Full Article
Search engine and full access to all medical articles
10 free questions in your specialty
Free CME/CE Activities
Free daily question in your email
Save favorite articles to your dashboard
Emails offering discounts
Learn more about a Subscription to StatPearls Point-of-Care
Etiology
An ST-elevation myocardial infarction occurs from occlusion of one or more of the coronary arteries that supply the heart with blood. The cause of this abrupt disruption of blood flow is usually plaque rupture, erosion, fissuring or dissection of coronary arteries that results in an obstructing thrombus. The major risk factors for ST-elevation myocardial infarction are dyslipidemia, diabetes mellitus, hypertension, smoking, and family history of coronary artery disease.[3][4]
Myocardial infarction in general can be classified [5] from Type 1 to Type 5 MI based on the etiology and pathogenesis. Type 1 MI is due to acute coronary atherothrombotic myocardial injury with plaque rupture. Most patients with ST-segment elevation MI (STEMI) and many with non-ST-segment elevation MI (NSTEMI) comprise this category. Type 2 MI is the most common type of MI encountered in clinical settings in which is there is demand-supply mismatch resulting in myocardial ischemia. This demand supply mismatch can be due to multiple reasons including but not limited to presence of a fixed stable coronary obstruction, tachycardia, hypoxia or stress. However, the presence of fixed coronary obstruction is not necessary. Other potential etiologies include coronary asospasm, coronary embolus, and spontaneous coronary artery dissection ( SCAD). Sudden cardiac death patients who succumb before any troponin elevation comprise Type 3 MI. Types 4 and 5 MIs are related to coronary revascularization procedures like Percutaneous Coronry Intervention (PCI) or Coronary artery Bypass Grfting ( CABG).
Epidemiology
The estimated annual incidence of myocardial infarction (MI) in the United States is 550,000 new and 200,000 recurrent.[6] In 2013, 116,793 persons in the United States suffered a fatal MI with 57% occurring in men and 43% in women.[6] The average age of incidence of a first MI is 65.1 for men and 72 for women.[6] Approximately 38% of patients who present to the hospital with acute coronary syndrome have an ST-elevation myocardial infarction.[6]
Pathophysiology
For an acute thrombotic coronary event to cause ST-segment elevation on a surface ECG, there needs to be a complete and persistent occlusion of blood flow. Coronary athersclerosis and presence of high risk thin cap fibroatheroma (TCFA) can result in sudden onset plaque rupture[7]. This results in changes in vascular endothelium resulting in cascade of platelet adhesion , activation and aggregartion [8] resulting in thrombosis formation.
Coronary artery occlusion in animal models shows a "wave-front" of myocardial injury that spreads from the sub-endocardial myocardium to the sub-epicardial myocardium resulting in a transmural infarction that appears as an ST elevation on surface ECG.[9] Myocardial damage occurs as soon as the blood flow is interrupted which makes timely management a necessity. Sudden onset acute ischmemia can result in severe microvascualr dysfunction
History and Physical
Prior to performing an ECG and collecting troponins the history and physical provide the only clues that lead to a diagnosis of myocardial infarction. Initial evaluation should include a focused physical examination and a brief history. Patients should be asked about the characteristics of the pain and associated symptoms, risk factors or history of cardiovascular disease, and recent drug use.[10] Risk factors for an ST-elevation myocardial infarction include age, gender, family history of premature coronary artery disease, tobacco use, dyslipidemia, diabetes mellitus, hypertension, abdominal obesity, sedentary lifestyle, a diet low in fruits and vegetables, psychosocial stressors.[11] Cocaine use can cause an ST-elevation myocardial infarction regardless of risk factors.[12] History of known congential abnormalities can be helpful. [13]
Evaluation
Evaluation of patients with acute onset of chest pain should begin with an electrocardiogram (ECG) and troponin level. The American College of Cardiology, American Heart Association, European Society of Cardiology, and the World Heart Federation committee established the following ECG criteria for ST-elevation myocardial infarction (STEMI)[14]:
- New ST-segment elevation at the J point in 2 contiguous leads with the cutoff point as greater than 0.1 mV in all leads other than V2 or V3
- In leads V2-V3 the cutoff point is greater than 0.2 mV in men older than 40 years old and greater than 0.25 in men younger than 40 years old, or greater than 0.15 mV in women
Patients with a pre-existing left bundle branch block can be further evaluated using Sgarbossa's criteria[15][16]:
- ST-segment elevation of 1 mm or more that is concordant with (in the same direction as) the QRS complex
- ST-segment depression of 1 mm or more in lead V1, V2, or V3
- ST-segment elevation of 5 mm or more that is discordant with (in the opposite direction) the QRS complex
Treatment / Management
After making the diagnosis of acute ST-elevation myocardial infarction, intravenous access should be obtained, and cardiac monitoring started. Patients that are hypoxemic or at risk for hypoxemia benefit from oxygen therapy; however, recent studies show possible deleterious effects in normoxic patients.[17][18] Patients should undergo percutaneous coronary intervention (PCI) within 90 minutes of presentation at a PCI capable hospital or within 120 minutes if transfer to a PCI capable hospital is required.[19] If PCI is not possible within the first 120 minutes of first medical contact, fibrinolytic therapy should be initiated within 30 minutes of patient arrival at the hospital.[19] It is important to rule out conditions that can mimic an acute coronary syndrome like acute aortic dissection or acute pulmonary embolism.(B3)
All patients with an acute myocardial infarction should be started on a beta blocker, high intensity statin, aspirin, and a P2Y12 inhibitor as soon as possible, with certain exceptions. Nitroglycerin administration can reduce anginal pain however it should be avoided in patients who have used phosphodiesterase inhibiting medication within the last 24 hours and in cases of right ventricular infarction. Further pain relief with morphine can be given for patients that continue report discomfort after nitroglycerin administration however judicious use is not recommended as it may adversely affect outcomes.[20] P2Y inhibiting antiplatelet medication choice depends on whether the patient underwent PCI or fibrinolytic therapy. Ticagrelor and prasugrel are preferred to clopidogrel in patients who undergo PCI due to recent trials showing superiority.[21][22] Patients undergoing fibrinolytic therapy should be started on clopidogrel.[23] It is important to be careful about relative contraindications of P2Y12 inhibitors . Prasugrel is contraindicated in pateints with h/o Transient Ischemic attack and stroke.(A1)
Anticoagulation should also be started aongside with unfractionated heparin, low-molecular-weight heparin, bivalirudin, or fondaparinux[24]
Differential Diagnosis
Other pathologies that can cause ST-segment elevations include: myocarditis, pericarditis, stress cardiomyopathy (Takotsubo), benign early repolarization, Acute vasospasm, spontaneous coronary artery dissection, left bundle branch block, various channelopathies, and electrolyte abnormalities.
Prognosis
Mortality rates at 30 days for patients presenting with ST-elevation myocardial infarction are between 2.5% to 10%.[25][26][27][25] The most commonly used scoring system for 30-day mortality is the TIMI risk score.[28] The TIMI scoring system considers:
- Age older than 75 years (3 points); Age 64 to 74 (2 points)
- Diabetes, hypertension, or history of angina (1 point)
- Systolic blood pressure less than 100 mm Hg (3 points)
- Heart rate greater than 100 beats per minute (2 points)
- Killip class II to IV (2 points)
- Body weight less than 150 lbs (1 point)
Complications
There are 3 life-threatening mechanical complications of myocardial infarction: ventricular free wall rupture, interventricular septum rupture, and acute mitral regurgitation. Ventricular free wall rupture occurs within 5 days in half the cases and within 2 weeks in 90% of cases with an overall mortality rate of greater than 80%.[29][30] Rupture of the interventricular septum is reported about half as often as free wall rupture and typically occurs 3 to 5 days with an overall mortality rate greater than 70%.[31][32] Prompt surgery reduces the mortality rate in both conditions. Acute mitral regurgitation following a myocardial infarction is most commonly due to ischemic papillary muscle displacement, left ventricular dilatation, or rupture of the papillary muscle of chordae.[33] In ST-elevation myocardial infarction, the degree of mitral regurgitation is usually severe and associated with a 30-day survival of 24%.[33]
Enhancing Healthcare Team Outcomes
A door-to-balloon time of fewer than 90 minutes is the goal of a PCI capable facility and is one of the core measures of the Joint Commission on Accreditation of Healthcare Organizations.[34][35] This is the time between the patient's arrival in the emergency department and the crossing of the culprit lesion by a guide wire in the cardiac cath lab. Teamwork between EMS, emergency department physician, and interventional cardiologist sets the groundwork for optimal door-to-balloon times (Level 1). As of 2010, the median door-to-balloon time was 64 minutes with 91% of patients receiving PCI in under 90 minutes and 70% in under 75 minutes.[34]
Media
(Click Image to Enlarge)
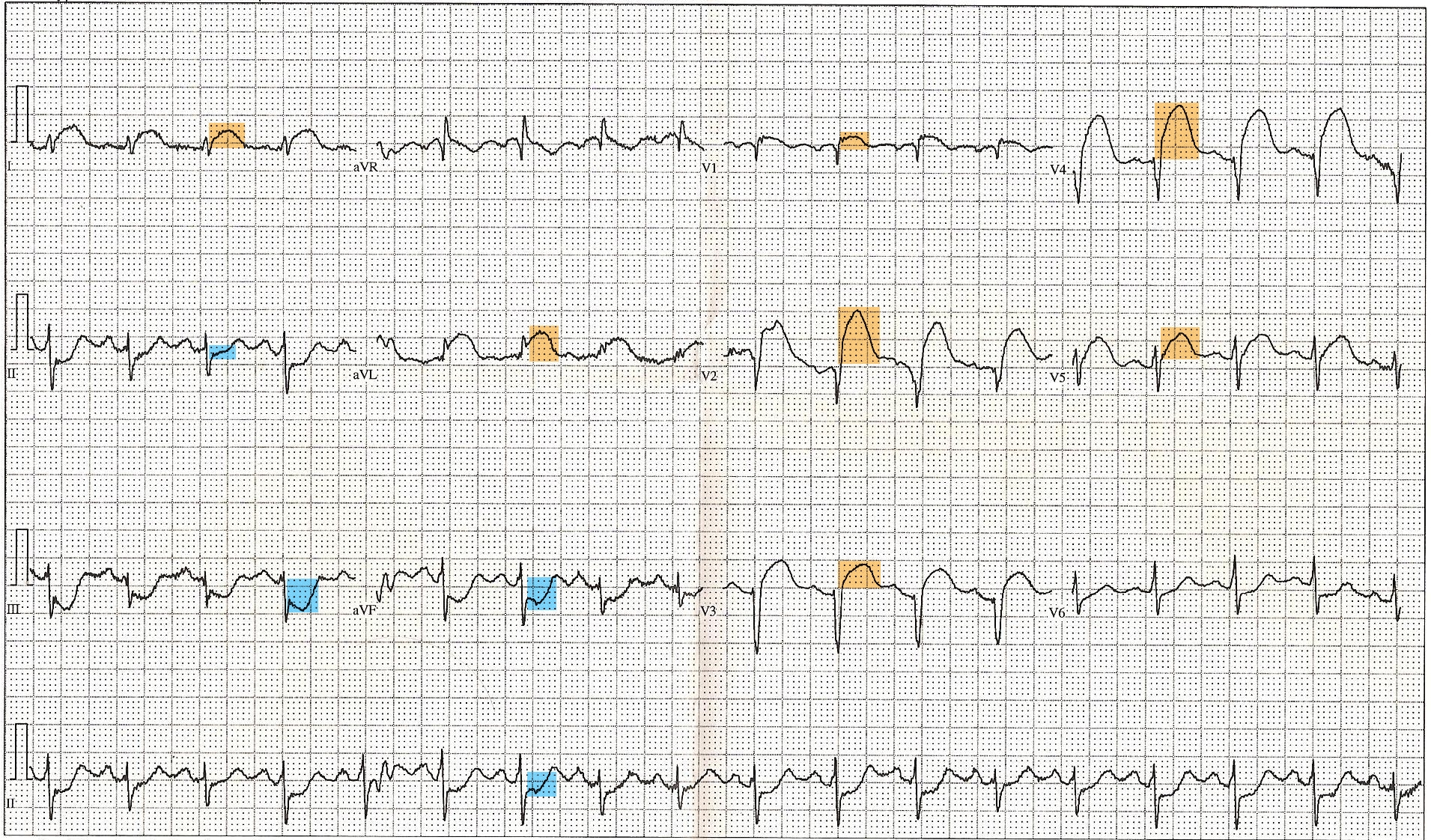
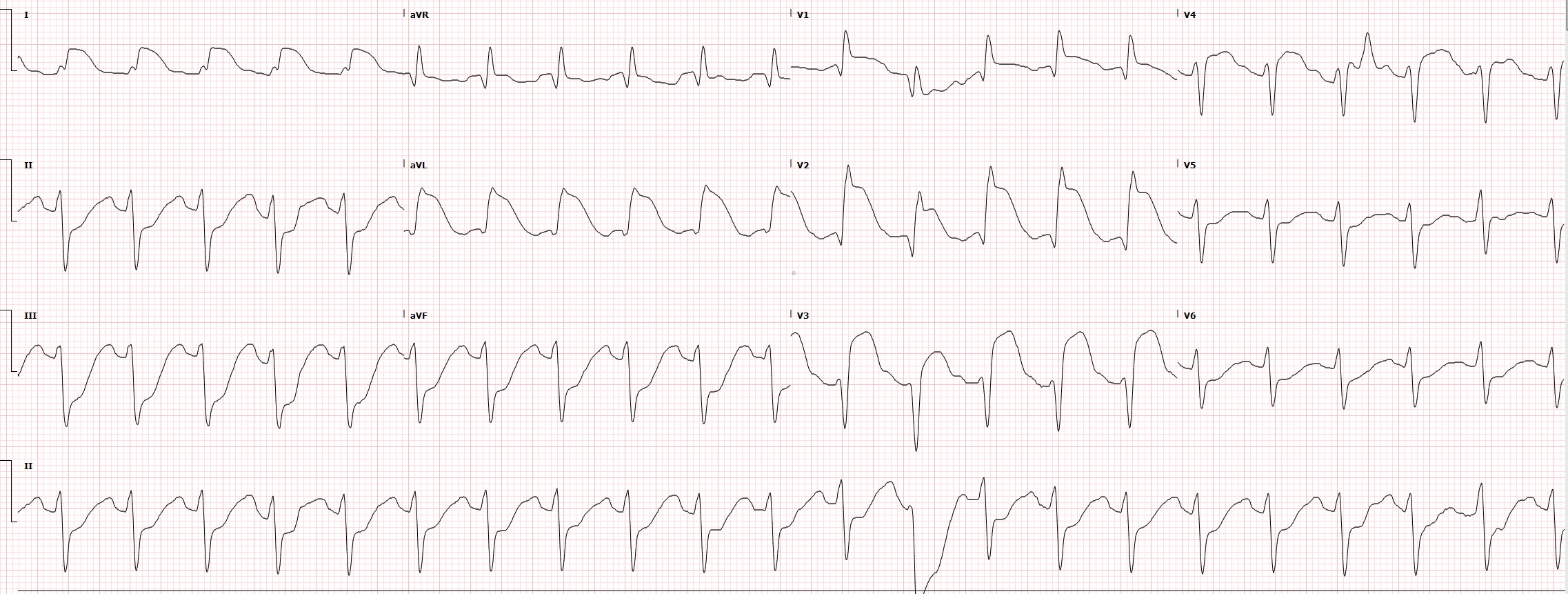
ST-Elevated Myocardial Infarction on ECG. This 12-lead electrocardiogram shows ST elevation in the anterior (orange) and inferior (blue) leads. Tachycardia and anterrior fascicular block are also noted. A diagnosis of ST-elevated myocardial infarction (STEMI) can be made along with clinical evaluation and cardiac marker elevation.
Contributed by Wikimedia Commons, Displaced (Public Domain-Self)
(Click Image to Enlarge)
References
Alpert JS, Thygesen K, Antman E, Bassand JP. Myocardial infarction redefined--a consensus document of The Joint European Society of Cardiology/American College of Cardiology Committee for the redefinition of myocardial infarction. Journal of the American College of Cardiology. 2000 Sep:36(3):959-69 [PubMed PMID: 10987628]
Level 1 (high-level) evidenceThygesen K, Alpert JS, Jaffe AS, Chaitman BR, Bax JJ, Morrow DA, White HD, ESC Scientific Document Group. Fourth universal definition of myocardial infarction (2018). European heart journal. 2019 Jan 14:40(3):237-269. doi: 10.1093/eurheartj/ehy462. Epub [PubMed PMID: 30165617]
Wilson PW. Established risk factors and coronary artery disease: the Framingham Study. American journal of hypertension. 1994 Jul:7(7 Pt 2):7S-12S [PubMed PMID: 7946184]
Canto JG, Kiefe CI, Rogers WJ, Peterson ED, Frederick PD, French WJ, Gibson CM, Pollack CV Jr, Ornato JP, Zalenski RJ, Penney J, Tiefenbrunn AJ, Greenland P, NRMI Investigators. Number of coronary heart disease risk factors and mortality in patients with first myocardial infarction. JAMA. 2011 Nov 16:306(19):2120-7. doi: 10.1001/jama.2011.1654. Epub [PubMed PMID: 22089719]
Hartikainen TS, Sörensen NA, Haller PM, Goßling A, Lehmacher J, Zeller T, Blankenberg S, Westermann D, Neumann JT. Clinical application of the 4th Universal Definition of Myocardial Infarction. European heart journal. 2020 Jun 14:41(23):2209-2216. doi: 10.1093/eurheartj/ehaa035. Epub [PubMed PMID: 32077925]
Writing Group Members, Mozaffarian D, Benjamin EJ, Go AS, Arnett DK, Blaha MJ, Cushman M, Das SR, de Ferranti S, Després JP, Fullerton HJ, Howard VJ, Huffman MD, Isasi CR, Jiménez MC, Judd SE, Kissela BM, Lichtman JH, Lisabeth LD, Liu S, Mackey RH, Magid DJ, McGuire DK, Mohler ER 3rd, Moy CS, Muntner P, Mussolino ME, Nasir K, Neumar RW, Nichol G, Palaniappan L, Pandey DK, Reeves MJ, Rodriguez CJ, Rosamond W, Sorlie PD, Stein J, Towfighi A, Turan TN, Virani SS, Woo D, Yeh RW, Turner MB, American Heart Association Statistics Committee, Stroke Statistics Subcommittee. Heart Disease and Stroke Statistics-2016 Update: A Report From the American Heart Association. Circulation. 2016 Jan 26:133(4):e38-360. doi: 10.1161/CIR.0000000000000350. Epub 2015 Dec 16 [PubMed PMID: 26673558]
Kolodgie FD, Burke AP, Farb A, Gold HK, Yuan J, Narula J, Finn AV, Virmani R. The thin-cap fibroatheroma: a type of vulnerable plaque: the major precursor lesion to acute coronary syndromes. Current opinion in cardiology. 2001 Sep:16(5):285-92 [PubMed PMID: 11584167]
Level 3 (low-level) evidenceScharf RE. Platelet Signaling in Primary Haemostasis and Arterial Thrombus Formation: Part 1. Hamostaseologie. 2018 Nov:38(4):203-210. doi: 10.1055/s-0038-1675144. Epub 2018 Oct 23 [PubMed PMID: 30352470]
Reimer KA, Jennings RB. The "wavefront phenomenon" of myocardial ischemic cell death. II. Transmural progression of necrosis within the framework of ischemic bed size (myocardium at risk) and collateral flow. Laboratory investigation; a journal of technical methods and pathology. 1979 Jun:40(6):633-44 [PubMed PMID: 449273]
Level 3 (low-level) evidenceAmsterdam EA, Wenger NK, Brindis RG, Casey DE Jr, Ganiats TG, Holmes DR Jr, Jaffe AS, Jneid H, Kelly RF, Kontos MC, Levine GN, Liebson PR, Mukherjee D, Peterson ED, Sabatine MS, Smalling RW, Zieman SJ. 2014 AHA/ACC Guideline for the Management of Patients with Non-ST-Elevation Acute Coronary Syndromes: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. Journal of the American College of Cardiology. 2014 Dec 23:64(24):e139-e228. doi: 10.1016/j.jacc.2014.09.017. Epub 2014 Sep 23 [PubMed PMID: 25260718]
Level 3 (low-level) evidenceTorpy JM, Burke AE, Glass RM. JAMA patient page. Coronary heart disease risk factors. JAMA. 2009 Dec 2:302(21):2388. doi: 10.1001/jama.302.21.2388. Epub [PubMed PMID: 19952328]
McCord J, Jneid H, Hollander JE, de Lemos JA, Cercek B, Hsue P, Gibler WB, Ohman EM, Drew B, Philippides G, Newby LK, American Heart Association Acute Cardiac Care Committee of the Council on Clinical Cardiology. Management of cocaine-associated chest pain and myocardial infarction: a scientific statement from the American Heart Association Acute Cardiac Care Committee of the Council on Clinical Cardiology. Circulation. 2008 Apr 8:117(14):1897-907. doi: 10.1161/CIRCULATIONAHA.107.188950. Epub 2008 Mar 17 [PubMed PMID: 18347214]
Akbar H, Kahloon A, Kahloon R. Diagnostic Challenge in a Symptomatic Patient of Arteria Lusoria with Retro-esophageal Right Subclavian Artery and Absent Brachiocephalic Trunk. Cureus. 2020 Feb 18:12(2):e7029. doi: 10.7759/cureus.7029. Epub 2020 Feb 18 [PubMed PMID: 32117665]
Thygesen K, Alpert JS, Jaffe AS, Simoons ML, Chaitman BR, White HD, Joint ESC/ACCF/AHA/WHF Task Force for the Universal Definition of Myocardial Infarction, Katus HA, Lindahl B, Morrow DA, Clemmensen PM, Johanson P, Hod H, Underwood R, Bax JJ, Bonow RO, Pinto F, Gibbons RJ, Fox KA, Atar D, Newby LK, Galvani M, Hamm CW, Uretsky BF, Steg PG, Wijns W, Bassand JP, Menasché P, Ravkilde J, Ohman EM, Antman EM, Wallentin LC, Armstrong PW, Simoons ML, Januzzi JL, Nieminen MS, Gheorghiade M, Filippatos G, Luepker RV, Fortmann SP, Rosamond WD, Levy D, Wood D, Smith SC, Hu D, Lopez-Sendon JL, Robertson RM, Weaver D, Tendera M, Bove AA, Parkhomenko AN, Vasilieva EJ, Mendis S. Third universal definition of myocardial infarction. Circulation. 2012 Oct 16:126(16):2020-35. doi: 10.1161/CIR.0b013e31826e1058. Epub 2012 Aug 24 [PubMed PMID: 22923432]
Sgarbossa EB, Pinski SL, Barbagelata A, Underwood DA, Gates KB, Topol EJ, Califf RM, Wagner GS. Electrocardiographic diagnosis of evolving acute myocardial infarction in the presence of left bundle-branch block. GUSTO-1 (Global Utilization of Streptokinase and Tissue Plasminogen Activator for Occluded Coronary Arteries) Investigators. The New England journal of medicine. 1996 Feb 22:334(8):481-7 [PubMed PMID: 8559200]
Level 2 (mid-level) evidenceSmith SW, Dodd KW, Henry TD, Dvorak DM, Pearce LA. Diagnosis of ST-elevation myocardial infarction in the presence of left bundle branch block with the ST-elevation to S-wave ratio in a modified Sgarbossa rule. Annals of emergency medicine. 2012 Dec:60(6):766-76. doi: 10.1016/j.annemergmed.2012.07.119. Epub 2012 Aug 31 [PubMed PMID: 22939607]
Level 2 (mid-level) evidenceStub D, Smith K, Bernard S, Nehme Z, Stephenson M, Bray JE, Cameron P, Barger B, Ellims AH, Taylor AJ, Meredith IT, Kaye DM, AVOID Investigators. Air Versus Oxygen in ST-Segment-Elevation Myocardial Infarction. Circulation. 2015 Jun 16:131(24):2143-50. doi: 10.1161/CIRCULATIONAHA.114.014494. Epub 2015 May 22 [PubMed PMID: 26002889]
Hofmann R, James SK, Jernberg T, Lindahl B, Erlinge D, Witt N, Arefalk G, Frick M, Alfredsson J, Nilsson L, Ravn-Fischer A, Omerovic E, Kellerth T, Sparv D, Ekelund U, Linder R, Ekström M, Lauermann J, Haaga U, Pernow J, Östlund O, Herlitz J, Svensson L, DETO2X–SWEDEHEART Investigators. Oxygen Therapy in Suspected Acute Myocardial Infarction. The New England journal of medicine. 2017 Sep 28:377(13):1240-1249. doi: 10.1056/NEJMoa1706222. Epub 2017 Aug 28 [PubMed PMID: 28844200]
O'Gara PT, Kushner FG, Ascheim DD, Casey DE Jr, Chung MK, de Lemos JA, Ettinger SM, Fang JC, Fesmire FM, Franklin BA, Granger CB, Krumholz HM, Linderbaum JA, Morrow DA, Newby LK, Ornato JP, Ou N, Radford MJ, Tamis-Holland JE, Tommaso CL, Tracy CM, Woo YJ, Zhao DX, Anderson JL, Jacobs AK, Halperin JL, Albert NM, Brindis RG, Creager MA, DeMets D, Guyton RA, Hochman JS, Kovacs RJ, Kushner FG, Ohman EM, Stevenson WG, Yancy CW, American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. 2013 ACCF/AHA guideline for the management of ST-elevation myocardial infarction: a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. Circulation. 2013 Jan 29:127(4):e362-425. doi: 10.1161/CIR.0b013e3182742cf6. Epub 2012 Dec 17 [PubMed PMID: 23247304]
Level 3 (low-level) evidenceMeine TJ, Roe MT, Chen AY, Patel MR, Washam JB, Ohman EM, Peacock WF, Pollack CV Jr, Gibler WB, Peterson ED, CRUSADE Investigators. Association of intravenous morphine use and outcomes in acute coronary syndromes: results from the CRUSADE Quality Improvement Initiative. American heart journal. 2005 Jun:149(6):1043-9 [PubMed PMID: 15976786]
Level 2 (mid-level) evidenceWiviott SD, Braunwald E, McCabe CH, Montalescot G, Ruzyllo W, Gottlieb S, Neumann FJ, Ardissino D, De Servi S, Murphy SA, Riesmeyer J, Weerakkody G, Gibson CM, Antman EM, TRITON-TIMI 38 Investigators. Prasugrel versus clopidogrel in patients with acute coronary syndromes. The New England journal of medicine. 2007 Nov 15:357(20):2001-15 [PubMed PMID: 17982182]
Level 1 (high-level) evidenceWallentin L, Becker RC, Budaj A, Cannon CP, Emanuelsson H, Held C, Horrow J, Husted S, James S, Katus H, Mahaffey KW, Scirica BM, Skene A, Steg PG, Storey RF, Harrington RA, PLATO Investigators, Freij A, Thorsén M. Ticagrelor versus clopidogrel in patients with acute coronary syndromes. The New England journal of medicine. 2009 Sep 10:361(11):1045-57. doi: 10.1056/NEJMoa0904327. Epub 2009 Aug 30 [PubMed PMID: 19717846]
Level 1 (high-level) evidenceSabatine MS, Cannon CP, Gibson CM, López-Sendón JL, Montalescot G, Theroux P, Claeys MJ, Cools F, Hill KA, Skene AM, McCabe CH, Braunwald E, CLARITY-TIMI 28 Investigators. Addition of clopidogrel to aspirin and fibrinolytic therapy for myocardial infarction with ST-segment elevation. The New England journal of medicine. 2005 Mar 24:352(12):1179-89 [PubMed PMID: 15758000]
Level 1 (high-level) evidenceBraun M, Kassop D. Acute Coronary Syndrome: Management. FP essentials. 2020 Mar:490():20-28 [PubMed PMID: 32150365]
McManus DD, Gore J, Yarzebski J, Spencer F, Lessard D, Goldberg RJ. Recent trends in the incidence, treatment, and outcomes of patients with STEMI and NSTEMI. The American journal of medicine. 2011 Jan:124(1):40-7. doi: 10.1016/j.amjmed.2010.07.023. Epub [PubMed PMID: 21187184]
Jernberg T, Johanson P, Held C, Svennblad B, Lindbäck J, Wallentin L, SWEDEHEART/RIKS-HIA. Association between adoption of evidence-based treatment and survival for patients with ST-elevation myocardial infarction. JAMA. 2011 Apr 27:305(16):1677-84. doi: 10.1001/jama.2011.522. Epub [PubMed PMID: 21521849]
Rosamond WD, Chambless LE, Heiss G, Mosley TH, Coresh J, Whitsel E, Wagenknecht L, Ni H, Folsom AR. Twenty-two-year trends in incidence of myocardial infarction, coronary heart disease mortality, and case fatality in 4 US communities, 1987-2008. Circulation. 2012 Apr 17:125(15):1848-57. doi: 10.1161/CIRCULATIONAHA.111.047480. Epub 2012 Mar 15 [PubMed PMID: 22420957]
Level 3 (low-level) evidenceMorrow DA, Antman EM, Charlesworth A, Cairns R, Murphy SA, de Lemos JA, Giugliano RP, McCabe CH, Braunwald E. TIMI risk score for ST-elevation myocardial infarction: A convenient, bedside, clinical score for risk assessment at presentation: An intravenous nPA for treatment of infarcting myocardium early II trial substudy. Circulation. 2000 Oct 24:102(17):2031-7 [PubMed PMID: 11044416]
Level 2 (mid-level) evidenceBatts KP, Ackermann DM, Edwards WD. Postinfarction rupture of the left ventricular free wall: clinicopathologic correlates in 100 consecutive autopsy cases. Human pathology. 1990 May:21(5):530-5 [PubMed PMID: 2338333]
Level 3 (low-level) evidenceYip HK, Wu CJ, Chang HW, Wang CP, Cheng CI, Chua S, Chen MC. Cardiac rupture complicating acute myocardial infarction in the direct percutaneous coronary intervention reperfusion era. Chest. 2003 Aug:124(2):565-71 [PubMed PMID: 12907544]
Level 2 (mid-level) evidenceFigueras J, Alcalde O, Barrabés JA, Serra V, Alguersuari J, Cortadellas J, Lidón RM. Changes in hospital mortality rates in 425 patients with acute ST-elevation myocardial infarction and cardiac rupture over a 30-year period. Circulation. 2008 Dec 16:118(25):2783-9. doi: 10.1161/CIRCULATIONAHA.108.776690. Epub 2008 Dec 8 [PubMed PMID: 19064683]
Crenshaw BS, Granger CB, Birnbaum Y, Pieper KS, Morris DC, Kleiman NS, Vahanian A, Califf RM, Topol EJ. Risk factors, angiographic patterns, and outcomes in patients with ventricular septal defect complicating acute myocardial infarction. GUSTO-I (Global Utilization of Streptokinase and TPA for Occluded Coronary Arteries) Trial Investigators. Circulation. 2000 Jan 4-11:101(1):27-32 [PubMed PMID: 10618300]
Level 1 (high-level) evidenceTcheng JE, Jackman JD Jr, Nelson CL, Gardner LH, Smith LR, Rankin JS, Califf RM, Stack RS. Outcome of patients sustaining acute ischemic mitral regurgitation during myocardial infarction. Annals of internal medicine. 1992 Jul 1:117(1):18-24 [PubMed PMID: 1596043]
Level 2 (mid-level) evidenceKrumholz HM, Herrin J, Miller LE, Drye EE, Ling SM, Han LF, Rapp MT, Bradley EH, Nallamothu BK, Nsa W, Bratzler DW, Curtis JP. Improvements in door-to-balloon time in the United States, 2005 to 2010. Circulation. 2011 Aug 30:124(9):1038-45. doi: 10.1161/CIRCULATIONAHA.111.044107. Epub 2011 Aug 22 [PubMed PMID: 21859971]
Bradley EH, Nallamothu BK, Herrin J, Ting HH, Stern AF, Nembhard IM, Yuan CT, Green JC, Kline-Rogers E, Wang Y, Curtis JP, Webster TR, Masoudi FA, Fonarow GC, Brush JE Jr, Krumholz HM. National efforts to improve door-to-balloon time results from the Door-to-Balloon Alliance. Journal of the American College of Cardiology. 2009 Dec 15:54(25):2423-9. doi: 10.1016/j.jacc.2009.11.003. Epub [PubMed PMID: 20082933]