Introduction
Appendicitis is characterized by inflammation of the vermiform appendix and typically presents acutely within 24 hours. However, the presenting symptoms may be more indolent and less severe in cases with perforation with a contained abscess.[1][2][3][4]
Notably, acute appendicitis is the leading cause of abdominal surgery in children and the most prevalent abdominal surgical emergency worldwide.[5][6] The significance of this condition in terms of both pediatric and general surgery underscores the need for accurate diagnosis, prompt intervention, and appropriate management. Understanding the clinical features and distinctive nature of appendicitis is vital in providing timely care and preventing complications associated with this common condition.
Etiology
Register For Free And Read The Full Article
Search engine and full access to all medical articles
10 free questions in your specialty
Free CME/CE Activities
Free daily question in your email
Save favorite articles to your dashboard
Emails offering discounts
Learn more about a Subscription to StatPearls Point-of-Care
Etiology
Appendicitis is primarily caused by obstruction of the appendiceal lumen leading to inflammation. The obstruction can be due to various factors such as appendicoliths, appendiceal tumors, intestinal parasites, or hypertrophied lymphatic tissues. These mechanical obstructions result in the development of acute appendicitis. It is important to note that the underlying causes of luminal obstructions may vary among different age groups, highlighting the need for age-specific considerations when evaluating and managing appendicitis.
The appendix is known to naturally host aerobic and anaerobic bacteria, including Escherichia coli and Bacteroides spp. Obstruction of the appendiceal lumen by any mechanism can cause an overgrowth of bacteria leading to acute inflammation and abscess formation. Recent studies utilizing next-generation sequencing techniques have revealed that patients with complicated perforated appendicitis exhibit a significantly higher bacterial phyla load than those with uncomplicated appendicitis. This finding suggests that the severity and complications of appendicitis may be associated with an increased abundance of bacterial species.[7]
In the pediatric population, acute appendicitis is most commonly caused by lymphoid hyperplasia. This condition involves an overgrowth of lymphoid tissue in the appendix, leading to inflammation and localized ischemia. This inflammatory process increases the risk of appendiceal perforation, the formation of contained periappendiceal abscess, and subsequent peritonitis. Reactive lymphoid hyperplasia is frequently misdiagnosed as one of the etiologies of appendicitis.[8]
In adults, acute appendicitis is commonly attributed to various causes, including infections, fecaliths, or tumors. Tumors associated with acute appendicitis in adults include appendiceal adenocarcinoma, mucocele, and carcinoid tumor.[9]
Epidemiology
Acute appendicitis commonly represents a significant proportion of acute abdominal conditions. It has an incidence rate ranging from 100 to 223 new cases per 100,000 individuals per year.[10][11] In the United States alone, approximately 300,000 hospital visits are reported annually related to appendicitis.[12]
While acute appendicitis can occur at any age, it is most commonly observed in the age range of 5 to 45. This age distribution reflects the higher incidence of appendicitis during childhood, adolescence, and early adulthood. The mean age at presentation is 28. Overall, there is a slight preponderance of acute appendicitis in males compared to females. The lifetime incidence of acute appendicitis is 8.6% in males and 6.7% in females.[13] However, it is important to note that appendicitis can occur in both sexes, and the difference in incidence between males and females is not substantial.
Pathophysiology
Regardless of its cause, appendiceal luminal obstruction causes a rise in both intraluminal and intramural pressure. This increased pressure leads to small vessel occlusion, thrombosis, and lymphatic stasis. As a result, the obstructed appendix fills with mucus and becomes distended. As lymphatic and vascular compromise continues to progress, the wall of the appendix undergoes ischemia and necrosis. In addition, bacterial overgrowth occurs within the obstructed appendix, initially dominated by aerobic organisms during the early stages of appendicitis and later transitioning to a mixture of aerobic and anaerobic bacteria as the disease progresses. Commonly involved organisms include E coli, Peptostreptococcus, Bacteroides, and Pseudomonas.
Once significant inflammation and necrosis develop, the appendix becomes susceptible to perforation, which can form a localized abscess. In severe cases, this can progress to peritonitis.[14]
Histopathology
A significant microscopic finding in cases of acute appendicitis is the presence of neutrophilic infiltration within the appendiceal muscularis propria. The severity of the infection and duration of the disease process directly correlates with the degree and extent of the inflammation observed. As acute appendicitis progresses, the inflammation involves the appendiceal fat and surrounding tissues.[15]
Based on histopathological findings, acute appendicitis is classified into three main categories: suppurative or phlegmonous, gangrenous, and periappendicitis.
Suppurative or phlegmonous appendicitis is characterized by neutrophils infiltrating the appendiceal mucosa, submucosa, and muscularis propria. The inflammatory process extends throughout the entire appendiceal wall and can cause extensive ulceration. In addition, intramural abscesses accompanied by vascular thrombosis may be observed. Suppurative appendicitis has a varied gross appearance but commonly observed findings include poorly-demarcated serosa, dilation of the appendix, congestion of surface blood vessels, and fibrinopurulent serosal exudate. However, an increased appendiceal diameter alone is not a conclusive finding and should be interpreted in conjunction with other clinical and histopathological features.
Gangrenous appendicitis is characterized by the necrosis of the appendix wall. If left untreated, perforation will eventually occur. In cases where perforation has taken place, transmural inflammation with areas of necrosis and extensive mucosal ulceration can be observed. Therefore, perforation is considered a complication of untreated gangrenous appendicitis. Grossly, the appendix wall appears friable and may display shades of purple, green, or black.
Periappendicitis primarily involves serosal and subserosal inflammation without extending into the muscularis propria. The gross appearance of periappendicitis varies from normal serosa to congestion, accompanied by exudative infiltration.[16]
Detailed histopathological findings differ in uncomplicated and complicated appendicitis.
Uncomplicated Appendicitis
Uncomplicated appendicitis typically exhibits several characteristic features, including borderline-dilated serosal vessels, indicating increased appendiceal blood flow, and dulling of the serosa. Intraluminal neutrophils are another common finding. Furthermore, neutrophils may also be present within the mucosa and submucosa, and frank erosions may be seen. These findings indicate the presence of inflammation and tissue damage.[17]
Complicated Appendicitis
Complicated appendicitis with phlegmon exhibits several notable features. The appendiceal lumen is often dilated and filled with blood, indicating vascular congestion. Additionally, inflammation of the mesoappendix is observed, characterized by the presence of exudates. Neutrophils within the mucosa, submucosa, and muscularis propria indicate a widespread inflammatory response. Extensive ulceration, signifying tissue damage and loss of epithelial lining, is commonly observed. Intramural microabscesses may also be present. Vascular thrombosis, resulting from the inflammatory process, is not uncommon.
Complicated nonperforated appendicitis includes two distinct histopathologic categories: severe phlegmonous appendicitis and gangrenous non-perforated appendicitis.
The histopathological findings of severe phlegmonous appendicitis are complex and are characterized by severe phlegmonous inflammation accompanied by obstruction and extraluminal fluid. The obstruction is usually caused by a fecalith, resulting in significant distal luminal dilation and adjacent fluid accumulation. The histological examination reveals pronounced transmural edema and infiltration of neutrophils throughout the appendiceal wall.[17]
The histopathological examination of gangrenous appendicitis reveals a friable appendix with purple, green, or black discoloration. In addition, the appendix shows transmural inflammation, with areas of necrosis and extensive mucosal ulceration. These findings indicate a severe inflammatory process that has compromised the blood supply to the appendix, leading to tissue death and decay.
Complicated Perforated Appendicitis
In cases of complicated perforated appendicitis, the histopathological evaluation may exhibit features indicative of abscess formation, characterized by marked transmural inflammation and neutrophils infiltrating the affected tissue. The inflammation frequently extends beyond the appendix to involve the surrounding mesoappendix. Complicated perforated appendicitis is a severe inflammatory process involving the appendix and the surrounding tissues, manifesting as evidence of perforation, abscess formation, and high-grade inflammation.[17]
History and Physical
The primary symptom of acute appendicitis typically begins as a diffuse or periumbilical abdominal pain that eventually becomes localized to the right lower quadrant. Stimulation of the visceral T8-T10 afferent nerve fibers causes this initial vague abdominal pain. As the inflamed parietal peritoneum in the adjacent area becomes irritated, the pain becomes more focused in the right lower quadrant. Patients may experience pain that awakens them from sleep or intensifies when walking or coughing. Alongside abdominal pain, individuals may also present with anorexia, nausea with or without vomiting, diarrhea, malaise, and urinary frequency or urgency.[18] Approximately 40% of patients with acute appendicitis are febrile at the time of presentation. Some patients may exhibit atypical or uncommon presenting features.
Physical examination findings are often subtle, especially in early appendicitis. As inflammation progresses, signs of peritoneal irritation develop. Localized guarding of the right lower abdominal quadrant and rebound tenderness of McBurney point, approximately 1.5 to 2 inches from the anterior superior iliac spine (ASIS) on a straight imaginary line to the umbilicus, are frequently observed in cases of acute appendicitis. However, these clinical findings are not specific to appendicitis and can also be present in other conditions.
There are other commonly encountered physical examination findings in cases of suspected appendicitis. However, it is essential to note that these findings are not diagnostic. Dunphy sign is the finding of increased abdominal pain with coughing or performing any activity that increases intra-abdominal pressure. Rovsing sign is pain in the right lower quadrant elicited by palpation or pressure of the left lower quadrant. A positive psoas sign is right lower quadrant pain with right hip extension or right thigh flexion against resistance. This pain occurs due to irritation of the psoas muscle by the inflamed appendix. Patients often flex the hip to shorten the muscle to relieve this pain.[19]
The time course of symptoms in acute appendicitis is highly variable; symptoms typically escalate gradually from the onset of appendicitis and may progress for 12 to 24 hours. However, it is important to note that in complicated appendicitis cases, symptoms can be prolonged and extend beyond 48 hours. Approximately 75% of patients with acute appendicitis present within 24 hours of the onset of symptoms. The risk of appendiceal rupture can vary, with about 2% of cases rupturing around 36 hours from the onset of symptoms. This risk tends to increase by approximately 5% for every additional 12 hours that pass without appropriate medical intervention.
Following appendiceal perforation, additional complications can arise. These complications may include pylephlebitis, pylethrombosis, hydroureteronephrosis, bowel obstruction, and the formation of internal fistulae. These internal fistulae can involve various structures such as the bladder, vagina, uterus, or skin. These complications may result in resistant fever and significant weight loss.[20]
Evaluation
Laboratory Testing
The laboratory evaluation of patients with suspected acute appendicitis should include a total leukocyte count with differential and serum C-reactive protein (CRP) levels.[21] The white blood cell (WBC) count and CRP concentration have a positive predictive value when used together to differentiate between uncomplicated and complicated appendicitis. A combination of a normal WBC count and a normal CRP value has a high negative predictive value for acute appendicitis. Increasing CRP and WBC levels significantly increases the likelihood of complicated appendicitis.[22]
Leukocytosis is present in approximately two-thirds of patients with acute appendicitis. A left shift or bandemia may accompany this increase in WBC count. While no laboratory value can confirm or exclude acute appendicitis, most patients with acute appendicitis will have a WBC count of >10,000 cells/mm3. Accordingly, a WBC count ≥17,000 cells/mm3 is associated with complicated acute appendicitis.
Imaging
Appendicitis is primarily diagnosed based on clinical evaluation and examination. However, imaging modalities such as computed tomography (CT), ultrasonography (US), and magnetic resonance imaging (MRI) may be used to improve the specificity of the presumptive diagnosis. CT is the preferred imaging modality in patients with suspected acute appendicitis. Ultrasound is less sensitive and specific than CT for diagnosing appendicitis. However, US is useful in evaluating populations where the avoidance of ionizing radiation is preferred, such as children and pregnant patients. MRI may also be useful for pregnant patients with suspected appendicitis who have had an indeterminate ultrasound.
Computed Tomography (CT)
An abdominopelvic CT scan with intravenous contrast demonstrates >95% accuracy in diagnosing acute appendicitis in adults.
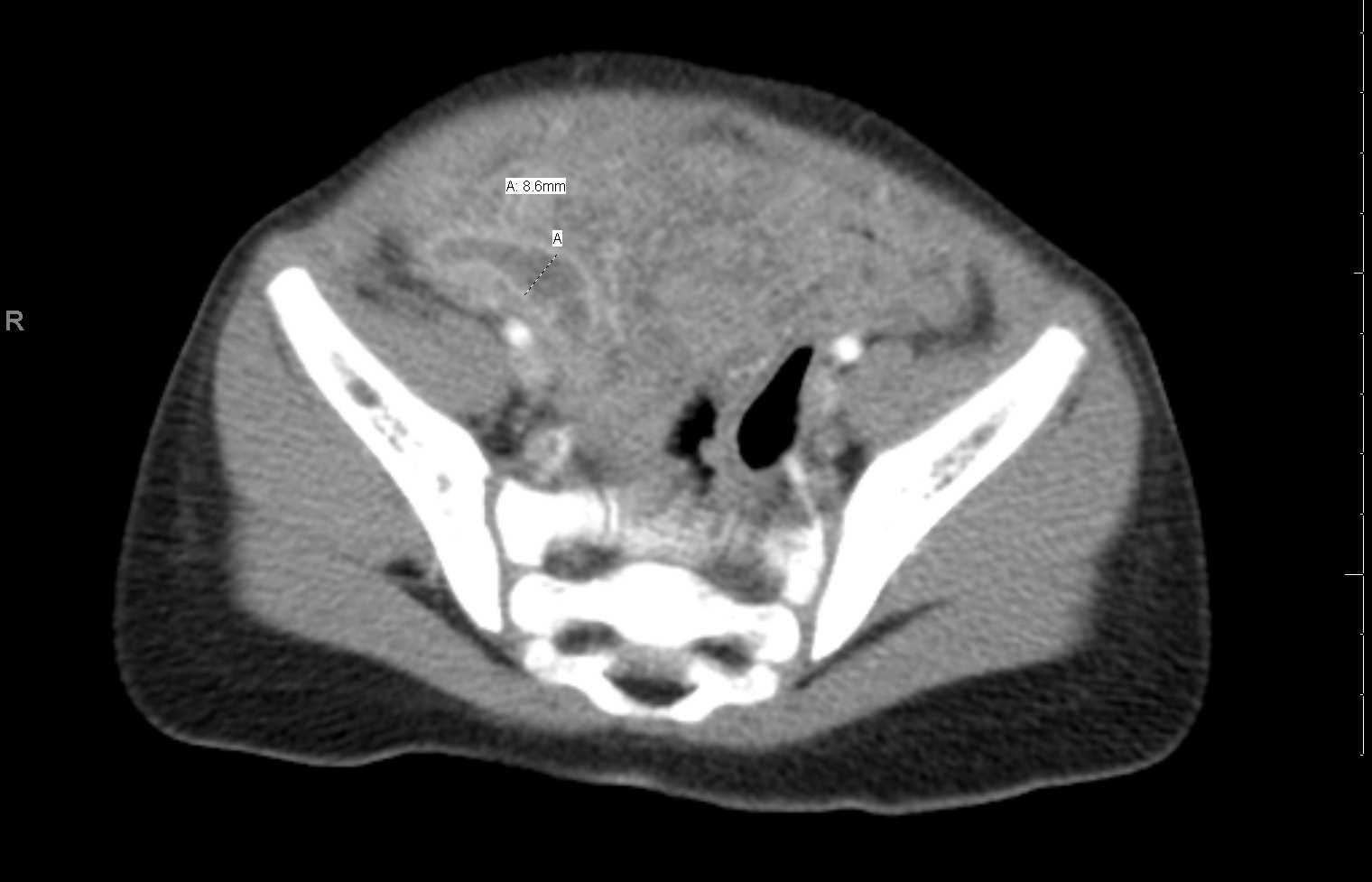
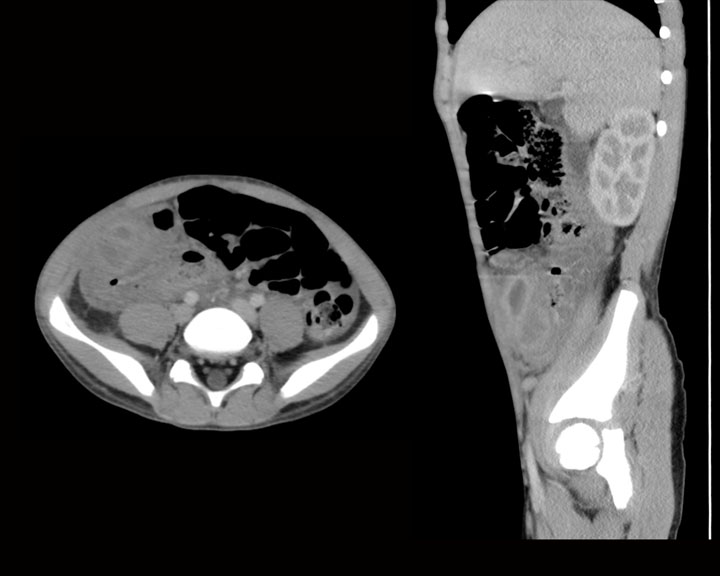
The criteria used in CT for diagnosing appendicitis include several features. These criteria encompass an enlarged appendix with an outer diameter of >6 mm to 8 or 9 mm, thickening of the appendiceal wall measuring >2 mm to 3 mm, periappendiceal fat stranding, enhancement of the appendiceal wall, the presence of inflamed soft tissue at the appendiceal base separating the appendix from the cecum, and the existence of an appendicolith.[23] In most cases of appendicitis, observing intraluminal contrast media or air due to luminal distention is uncommon.
The major concern with obtaining an abdominopelvic CT scan is radiation exposure; however, the average exposure with a typical abdominopelvic CT does not exceed 4 mSv and is only slightly above the background exposure of almost 3 mSv. Despite the higher resolution of CT images obtained with the maximal radiation of 4 mSv, lower exposures do not affect the clinical outcomes. Moreover, obtaining an abdominopelvic CT scan with intravenous contrast in patients suspected of acute appendicitis should be limited to those with a glomerular filtration rate (GFR) ≥ 30 ml/minute per 1.73 m2.[24][25][26]
Ultrasonography (US)
Abdominal US is a widely-available imaging modality frequently employed as the primary imaging tool in evaluating patients with acute abdominal pain. In addition, it is the preferred primary imaging modality in evaluating children and pregnant patients with suspected acute appendicitis.
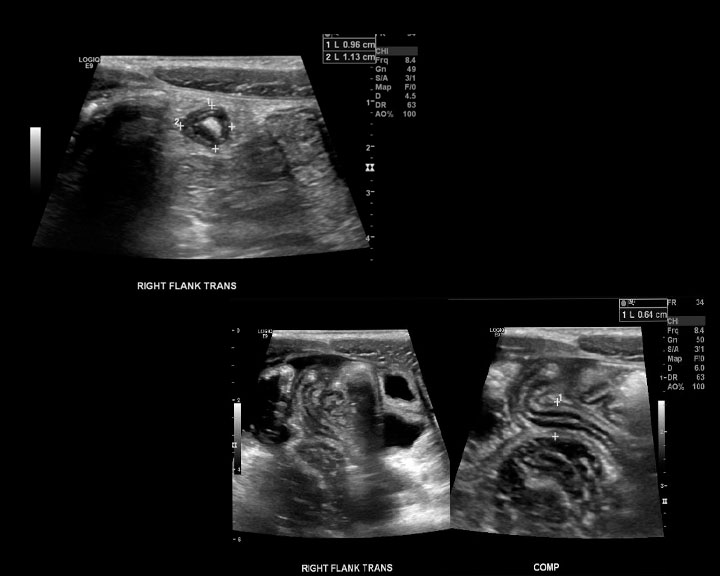
Ultrasonographic findings that indicate the possibility of acute appendicitis include an anteroposterior appendiceal diameter >6 mm, the presence of an appendicolith, and increased echogenicity of the periappendiceal fat. A specific ultrasonographic compressibility index and an appendiceal diameter of <5 mm are used to exclude appendicitis.
Certain factors can limit abdominal US in evaluating suspected acute appendicitis. One primary concern is the innate limitations of the modality in patients with obesity. The increased adipose tissue thickness in obese patients can make it more challenging to visualize the appendix and accurately assess for signs of appendicitis using ultrasound. Moreover, the graded compression technique during the abdominal US may be poorly tolerated in patients with complicated appendicitis and peritonitis.[27]
Magnetic Resonance Imaging (MRI)
Abdominopelvic MRI is considered highly sensitive and specific for diagnosing acute appendicitis. However, its use in evaluating suspected acute appendicitis is limited due to high costs and the need for specialized radiologic expertise for accurate imaging interpretation. The indications for MRI evaluation of suspected acute appendicitis are limited to particular patient populations for whom radiation exposure is less desirable. This population most commonly involves pregnant patients. If accessible, MRI is the second-most preferred imaging modality in pregnant patients with suspected acute appendicitis. While protocols vary significantly, most encompass imaging in three planes using a swiftly-acquired sequence featuring T2 weighting, and a subset incorporates T2 fat-suppressed imaging. MRI findings consistent with acute appendicitis parallel those observed in other modalities, such as luminal distension and dilation, wall thickening, and free periappendiceal fluid.[28]
The Use of Scoring Systems in the Evaluation of Acute Appendicitis
Several scoring systems have been developed to diagnose acute appendicitis promptly. These scoring systems primarily utilize criteria derived from the medical history, physical examination, and the results of laboratory testing and imaging studies. The Alvarado scoring system has been used to evaluate suspected acute appendicitis since 1986, and the modified Alvarado scoring system is the most widely used in current practice.
The modified Alvardo scoring system assigns a point value to diagnostic criteria as outlined:
- 2 points each: tenderness in the right lower quadrant and leukocytosis
- 1 point each: migratory right lower quadrant pain, rebound tenderness in the right lower quadrant, fever, nausea or vomiting, and anorexia
The highest score an individual with suspected acute appendicitis can receive is 9 points. Higher scores are consistent with a higher probability of acute appendicitis. An Alvarado score of 7 points or higher is significantly associated with acute appendicitis.[29]
Treatment / Management
Medical Management of Acute Appendicitis
Despite significant advancements in managing acute appendicitis with primary antibiotic therapy, the primary treatment option for acute appendicitis continues to be surgical. A large, randomized trial of antibiotic therapy for the primary management of acute appendicitis showed that while antibiotic therapy might have comparable results with appendectomy in the short term, 1 of 4 participants in the antibiotic therapy arm required appendectomy within 1 year.[30](A1)
The efficacy of antibiotics as the primary treatment for acute uncomplicated appendicitis has been extensively researched, yielding mixed and contradictory results and conclusions.[31][32][33] Adverse events, including 30-day postintervention peritonitis, were higher in the antibiotic therapy arm of one trial. However, other trials support the feasibility of antibiotic therapy alone despite the cumulative incidence of appendicitis recurrence for uncomplicated acute appendicitis.[34](A1)
Although the Comparison of Outcomes of Antibiotic Drugs and Appendectomy (CODA) trial offers the option of using antibiotics alone to manage acute appendicitis, it is imperative to exercise caution when considering this approach. Several outcomes of this approach remain uncertain, including the potential for missed malignancies, cases of recurrent appendicitis, and the long-term efficacy of this method.[35](A1)
The Prospective Observational Study on Acute Appendicitis Worldwide (POSAW), an international collaborative study, has confirmed that surgical management remains the main effective option for treating appendicitis.[30][36] Despite the availability of alternative therapeutic approaches with primary antibiotic therapy, appendectomy remains the standard practice for treating acute uncomplicated appendicitis.[37](A1)
The antibiotic coverage for acute appendicitis typically involves targeting aerobic and anaerobic bacteria pending culture results; a combination of antibiotics is used. A third-generation cephalosporin, such as ceftriaxone or cefotaxime, or a beta-lactam/beta-lactamase inhibitor, such as ampicillin-sulbactam, provides coverage against aerobic gram-negative bacteria. Either metronidazole or clindamycin is administered to provide coverage against anaerobic bacteria. This combination of antibiotics is chosen to cover a broad range of potential pathogens that may be involved in appendicitis. However, the choice of antibiotics may vary depending on local antimicrobial resistance patterns and individual patient factors, such as allergies or previous antibiotic exposure.
Surgical Management of Acute Appendicitis
The patient must be kept nil per os (NPO) in the emergency department and hydrated intravenously with crystalloid fluid. Antibiotics should be administered intravenously as per the surgical care team. The surgical team is responsible for obtaining an informed consent from the patient.
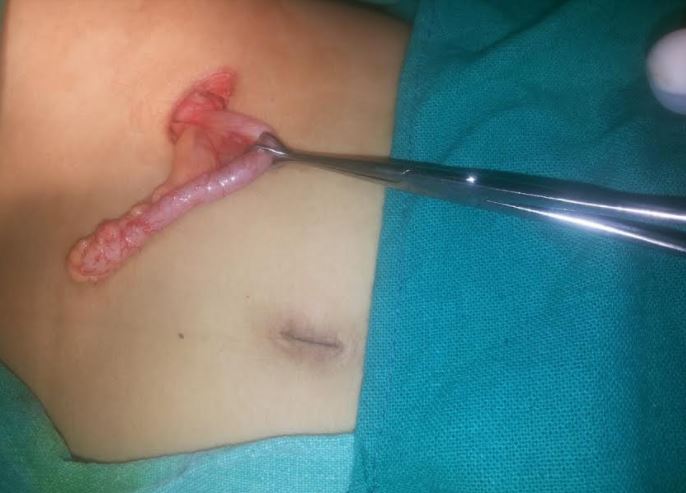
The gold-standard therapeutic intervention for acute appendicitis is appendectomy. Laparoscopic appendectomy is preferred over the open approach. Most uncomplicated appendectomies are performed laparoscopically. Several studies have compared the outcomes between patients who underwent laparoscopic appendectomy and those who underwent open appendectomy. The results suggested a lower incidence of wound infection, decreased level of postoperative analgesic requirement, and shorter postoperative hospital stays in the former group. The main disadvantage of laparoscopic appendectomy is the longer operative time.[38] (B2)
There is some disagreement regarding preoperative antibiotic administration for uncomplicated appendicitis. Some surgeons feel routine antibiotics in these cases are not warranted, while others give them routinely. Several studies have also promoted the treatment of uncomplicated appendicitis solely with antibiotics and avoiding surgery altogether.[1][39](A1)
Many patients with a presumptive diagnosis of acute appendicitis can be managed with a laparoscopic approach uneventfully. However, several factors predict the need to convert to the open approach. The only preoperative independent factor predicting a conversion during laparoscopic appendectomy is the presence of comorbidities. Moreover, some intra-operative findings, including periappendicular abscess and diffuse peritonitis, are independent predictors of a higher conversion rate and a significant increase in postoperative complications.[40]
Patients with a known periappendiceal abscess from a perforated appendix may require a percutaneous drainage procedure, usually performed by an interventional radiologist. Percutaneous abscess drainage allows the inflammation to subside over time, enabling a less technically difficult future laparoscopic appendectomy. Patients with a known periappendiceal abscess should receive broad-spectrum antibiotics, which may be continued for several weeks before elective appendectomy. While laparoscopic appendectomy can be performed in the presence of a periappendiceal abscess, extensive intraoperative irrigation of the abdominopelvic cavity is required, and the trocar sites may need to be left open to heal by secondary intention.
Alternative Surgical Techniques
While laparoscopic appendectomy has been widely used as the preferred approach for surgical management of acute appendicitis in many centers, open appendectomy might still be the practical choice in some clinical scenarios, such as complicated appendicitis with phlegmon. Several alternative surgical techniques, including Natural Orifice Transluminal Endoscopic Surgery (NOTES) and Single-incision Laparoscopic Surgery (SILS), have been introduced recently.
NOTES accesses the peritoneal cavity through natural orifices such as the gastrointestinal or vaginal tract. This surgical approach allows for a scarless or nearly scarless procedure. The major potential advantages of NOTES appendectomy are the avoidance of visible scars and reduced postoperative pain. A detailed comparison of postoperative outcomes that includes NOTES appendectomy is not yet possible; patient numbers are limited. The most significant drawback of this surgical technique is the need to hybrid with the laparoscopic approach to provide adequate retraction during the procedure and confirm the closure of the entry site.[41][42][43][44][45] (A1)
As a surgical technique, SILS for an appendectomy is performed with one incision in the umbilicus or a preexisting abdominal scar. Potential advantages of the SILS technique include decreased postoperative pain, wound-related postoperative complications, and recovery time.[46] However, up to 40% of patients require intraoperative conversion to a conventional laparoscopic procedure. The major disadvantage of SILS for an appendectomy is the higher risk of long-term complications, particularly incisional hernia.(A1)
Differential Diagnosis
The differential diagnosis of acute appendicitis includes but is not limited to Crohn ileitis, mesenteric adenitis, complicated cecal diverticulum, mittelschmerz, salpingitis, ruptured ovarian cyst, ectopic pregnancy, tubo-ovarian abscess, musculoskeletal disorders, endometriosis, pelvic inflammatory disease, gastroenteritis, right-sided colitis, renal colic, kidney stones, irritable bowel disease, testicular torsion, ovarian torsion, round ligament syndrome, and epididymitis.
A comprehensive medical history and a problem-oriented physical examination are necessary to narrow the differential diagnosis. Recent viral infection is suggestive of acute mesenteric adenitis. Acute bacterial ileitis may be due to infections with Yersinia or Campylobacter species.[47] Severe cervical motion tenderness during the bimanual pelvic examination may indicate pelvic inflammatory disease.
One of the most challenging differential diagnoses of acute appendicitis is the acute presentation of Crohn disease. While a past medical history significant for Crohn disease can prevent unnecessary surgical procedures in the setting of acute abdominal pain, Crohn disease can initially present acutely, mimicking acute appendicitis. Intraoperatively, ileal inflammation should raise the suspicion of Crohn disease.
Surgical Oncology
The occurrence rate of appendiceal neoplasms in the United States is 1.2 cases per 100,000; nearly 30% of these patients present with acute abdominal pain. The most common appendiceal malignancies are gastroenteropancreatic neuroendocrine or carcinoid tumors (GEP-NETs), goblet cell carcinoma (GCC), colonic-type adenocarcinoma, and mucinous neoplasm.[48]
Gastroenteropancreatic Neuroendocrine Tumors (GEP-NETs)
GEP-NETs are the most common histopathological subtype of appendiceal malignancies. They rarely metastasize; primary metastatic sites are the liver and lymph nodes. Therefore, in patients with suspicious GEP-NETs, further evaluation of the liver and the ileocolic lymph node basin are essential. Surgical management is dictated by the size of the primary tumor. An appendectomy with negative margins is the only surgical management in carcinoid tumors of <1 cm in size. A right hemicolectomy is indicated for a carcinoid tumor of >2 cm. The optimum surgical intervention for carcinoid tumors measuring from 1 to 2 cm remains undefined. However, a right hemicolectomy is recommended for mesenteric invasion, enlarged lymph nodes, or equivocal surgical margins.
Goblet Cell Carcinoma
Goblet cell carcinomas are ubiquitous in appendiceal malignancies, sharing the diagnostic features of both appendiceal adenocarcinoma and neuroendocrine tumors. A comprehensive peritoneal evaluation with further peritoneal cancer index score (PCIS) documentation should be undertaken. A right hemicolectomy will benefit patients with a non-metastatic lesion or a lesion ≥2 cm in size.[49]
Lymphoma
Non-Hodgkin lymphoma (NHL), including Mucosa-Associated Lymphoid Tissue (MALT) lymphoma, may initially present as acute appendicitis. The surgical management of this highly uncommon appendiceal malignancy should be limited to a simple appendectomy. However, a comprehensive systemic evaluation should be undertaken to exclude any potential metastatic site.[50]
Appendiceal Adenocarcinoma
Adenocarcinoma of the appendix, a rare appendiceal neoplasm with three histopathological subtypes, commonly presents as acute appendicitis. The standard treatment is a right hemicolectomy. The surgical management of appendiceal adenocarcinoma is irrespective of the tumor size or the involvement of the lymph node basin.[51]
Mucocele and Mucinous Neoplasm
Appendiceal mucoceles can manifest with symptoms similar to acute appendicitis. Mucoceles can arise from various benign or malignant processes involving mucosal hyperplasia and intra-appendiceal cystic formations. Several preoperative radiological features, including a well-encapsulated cystic structure in the right lower quadrant, would raise the suspicion of an appendiceal mucocele; a definitive diagnosis requires intraoperative evaluation and histopathological reports.
The preferred surgical management of appendiceal mucoceles is an appendectomy with great cautionary measures to prevent capsular rupture. It is important to assess for peritoneal involvement; peritoneal biopsy should be considered. In cases of suspicious mucinous neoplasm of the appendix, it is vital to perform a thorough peritoneal examination and consider recording any findings using the PCIS when mucin is present. Patient selection for the laparoscopic approach in managing appendiceal mucocele is limited to those with radiologic features suggestive of a homogenous cyst.[52]
Prognosis
Appendectomy is a relatively safe surgical procedure. In a global observational study, the overall mortality rate for appendicitis was 0.28%.[53] The mortality rate for appendicitis is higher in under-industrialized countries and ranges from 1% to 4%, whereas in industrialized countries, the mortality rate is 0.24%. The following factors are associated with increased mortality rates in appendicitis: age greater than 80 years, immunosuppression, severe cardiovascular disease or the presence of other comorbidities, previous episodes of suspected appendicitis, and prior antimicrobial therapy.
If acute appendicitis is diagnosed and definitively treated early in the course of the disease, recovery is expected within 24 to 48 hours. However, patients that present with advanced abscesses, peritonitis, or sepsis may have a more prolonged and complicated course, possibly requiring additional surgery.
Complications
The most common complication of appendectomy is an infection of the surgical site; this risk is highest in patients with complicated appendicitis with perforation. Surgical site infections include postoperative abscesses and wound infections. Hematomas and postoperative pain are also common complications of appendectomy. [6]
Recurrent appendicitis can occur in almost half of the patients managed nonoperatively; reported recurrence rates vary by study and length of follow-up. An interval appendectomy may be performed to mitigate the risk of recurrent appendicitis. Another form of recurrent appendicitis is stump appendicitis, resulting from an incomplete appendectomy and subsequent inflammation in the residual appendiceal stump. While stump appendicitis is most often seen following operative management of complicated appendicitis with perforation, it can occur whenever an excessively long appendiceal stump is left in situ. A stump size ≤5 mm minimizes the risk of stump appendicitis. Stump resection via an open or laparoscopic approach is the definitive therapeutic option; perforated appendiceal stumps often require extensive bowel resection.[54]
Diffuse peritonitis and sepsis are severe consequences of untreated or complicated appendicitis. These conditions can cause significant morbidity and, in some cases, even death.
Postoperative and Rehabilitation Care
Patients with uncomplicated appendicitis generally experience an uneventful postoperative course, and antibiotic therapy is not required. However, patients with complicated appendicitis should be scheduled for a 4-day course of antibiotic therapy. Wound complications, including infections, should be managed by ensuring an adequate wound opening and irrigation, followed by packing. However, antibiotic therapy is essential in managing patients who have complications such as abscess formation and deep fascial plane involvement.
Deterrence and Patient Education
Patients may resume normal activity within a few days to a week. However, the patient should avoid any strenuous activity and heavy lifting for the first 4 to 6 weeks.
Pearls and Other Issues
Patients with perforated appendicitis with an abscess warrant special consideration. Those who present with an abscess and do not exhibit peritonitis may benefit from CT or ultrasound-guided percutaneous drain placement and antibiotic therapy. Interval appendectomy is classically performed 6 to 10 weeks after recovery. Historically, 20% to 40% of patients treated medically for perforated appendicitis with an abscess had recurrent appendicitis. However, more recent studies suggest these rates are much lower.
Complications of appendicitis and appendectomy include surgical site infections, prolonged ileus, enterocutaneous fistula, and small bowel obstruction. In addition, intraabdominal abscess formation occurs in 3% to 4% of patients following an open appendectomy and 9% to 24% after a laparoscopic appendectomy.
Occasionally, an incorrect diagnosis of acute appendicitis is made when the correct diagnosis is Crohn disease of the cecum or terminal ileum. In such cases, if the base of the appendix is involved, it should be left in place. In this situation, removing the appendix carries a high risk of leak and fistula formation. Alternatively, if the base of the appendix is unaffected, appendectomy is recommended, even if the appendix appears grossly normal. This approach helps avoid future confusion when distinguishing between an exacerbation of Crohn disease and acute appendicitis.
Historically, the appendix was removed during nonrelated abdominal surgery to avoid developing appendicitis later in life. In current clinical practice, a normal appendix is left in situ during unrelated scheduled procedures. However, if the preoperative diagnosis of acute appendicitis proves incorrect, intraoperative appendectomy is recommended to avoid future diagnostic confusion.
Enhancing Healthcare Team Outcomes
Patients with acute appendicitis usually present to the emergency department with abdominal pain as their primary symptom. The triage team must be well-versed in recognizing the signs and symptoms of appendicitis. Prompt identification is necessary to facilitate admission and treatment and decrease the risk of appendiceal perforation. However, accurately diagnosing acute appendicitis can be difficult.
Several guidelines exist that can help practitioners make a diagnosis of acute appendicitis. While most physicians and advanced practice practitioners rely on the physical exam, others may choose to obtain an abdominal ultrasound in the diagnostic process. In cases where the diagnosis is uncertain, an abdominopelvic CT scan with IV contrast may be helpful; a CT without contrast is a reasonable option in cases of poor kidney function. The American College of Radiology recommends ultrasound as the imaging modality of choice for pregnant women with suspected appendicitis. In cases where the ultrasound results are inconclusive, MRI is suggested as the preferred imaging technique to aid in diagnosis within the same patient population.[55][56]
While the patient is undergoing investigation, intravenous access should be contained and fluids administered; the patient should be kept NPO until a definitive diagnosis is made.
Controversy exists regarding the optimal management of an appendiceal mass or phlegmon and the appropriate timing for surgery. There is no longer any question that laparoscopic appendectomy is associated with minimal pain and faster recovery, but it is costly. Other studies indicate that a single small incision provides comparable results to a laparoscopic appendectomy and is cost-effective. Given these controversies, an interprofessional team approach to the diagnosis and management of appendicitis must be established in each institution to ensure that the patient has no morbidity and that the management is cost-effective.[57] [Level 3]
Outcomes
Numerous large series have demonstrated that open and laparoscopic procedures yield excellent outcomes when treating simple appendicitis. [Level 3] However, more severe and complicated appendicitis is associated with poorer outcomes and increased utilization of resources. Further, the atypical presentation of appendicitis in pregnant patients and older individuals also makes diagnosis difficult and leads to a higher incidence of complications.[58][59] [Level 3] In an era of managed care where quality care indices are closely monitored, healthcare workers must be familiar with the current standards of diagnosing and managing appendicitis. Failure to adhere to these standards may result in denial of reimbursement.
Media
(Click Image to Enlarge)
(Click Image to Enlarge)
References
Vaos G, Dimopoulou A, Gkioka E, Zavras N. Immediate surgery or conservative treatment for complicated acute appendicitis in children? A meta-analysis. Journal of pediatric surgery. 2019 Jul:54(7):1365-1371. doi: 10.1016/j.jpedsurg.2018.07.017. Epub 2018 Jul 27 [PubMed PMID: 30115448]
Level 1 (high-level) evidenceGignoux B, Blanchet MC, Lanz T, Vulliez A, Saffarini M, Bothorel H, Robert M, Frering V. Should ambulatory appendectomy become the standard treatment for acute appendicitis? World journal of emergency surgery : WJES. 2018:13():28. doi: 10.1186/s13017-018-0191-4. Epub 2018 Jun 28 [PubMed PMID: 29988464]
Eng KA, Abadeh A, Ligocki C, Lee YK, Moineddin R, Adams-Webber T, Schuh S, Doria AS. Acute Appendicitis: A Meta-Analysis of the Diagnostic Accuracy of US, CT, and MRI as Second-Line Imaging Tests after an Initial US. Radiology. 2018 Sep:288(3):717-727. doi: 10.1148/radiol.2018180318. Epub 2018 Jun 19 [PubMed PMID: 29916776]
Level 1 (high-level) evidenceKartal İ. Childhood neuroendocrine tumors of the digestive system: A single center experience. Medicine. 2022 Feb 11:101(6):e28795. doi: 10.1097/MD.0000000000028795. Epub [PubMed PMID: 35147110]
Khan MS, Chaudhry MBH, Shahzad N, Tariq M, Memon WA, Alvi AR. Risk of appendicitis in patients with incidentally discovered appendicoliths. The Journal of surgical research. 2018 Jan:221():84-87. doi: 10.1016/j.jss.2017.08.021. Epub 2017 Sep 18 [PubMed PMID: 29229158]
Stringer MD. Acute appendicitis. Journal of paediatrics and child health. 2017 Nov:53(11):1071-1076. doi: 10.1111/jpc.13737. Epub 2017 Oct 17 [PubMed PMID: 29044790]
Bhangu A, Søreide K, Di Saverio S, Assarsson JH, Drake FT. Acute appendicitis: modern understanding of pathogenesis, diagnosis, and management. Lancet (London, England). 2015 Sep 26:386(10000):1278-1287. doi: 10.1016/S0140-6736(15)00275-5. Epub [PubMed PMID: 26460662]
Level 3 (low-level) evidenceUcar Karabulut K, Erinanc H, Yonar A, Kisinma A, Ucar Y. Correlation of histological diagnosis and laboratory findings in distinguishing acute appendicitis and lymphoid hyperplasia. Annals of surgical treatment and research. 2022 Nov:103(5):306-311. doi: 10.4174/astr.2022.103.5.306. Epub 2022 Nov 1 [PubMed PMID: 36452309]
Narula N, Gibbs KE, Kong F, Mukherjee I. Appendiceal Intussusception, Diverticula, and Fecalith Associated With Appendicitis. The American surgeon. 2022 Sep 8:():31348221126954. doi: 10.1177/00031348221126954. Epub 2022 Sep 8 [PubMed PMID: 36074037]
Buckius MT, McGrath B, Monk J, Grim R, Bell T, Ahuja V. Changing epidemiology of acute appendicitis in the United States: study period 1993-2008. The Journal of surgical research. 2012 Jun 15:175(2):185-90. doi: 10.1016/j.jss.2011.07.017. Epub 2011 Aug 9 [PubMed PMID: 22099604]
Level 2 (mid-level) evidenceSahm M, Koch A, Schmidt U, Wolff S, Pross M, Gastinger I, Lippert H. [Acute appendicitis - clinical health-service research on the current surgical therapy]. Zentralblatt fur Chirurgie. 2013 Jun:138(3):270-7. doi: 10.1055/s-0031-1283947. Epub 2012 Mar 16 [PubMed PMID: 22426968]
Level 2 (mid-level) evidenceAddiss DG, Shaffer N, Fowler BS, Tauxe RV. The epidemiology of appendicitis and appendectomy in the United States. American journal of epidemiology. 1990 Nov:132(5):910-25 [PubMed PMID: 2239906]
Level 2 (mid-level) evidenceTéoule P, Laffolie J, Rolle U, Reissfelder C. Acute Appendicitis in Childhood and Adulthood. Deutsches Arzteblatt international. 2020 Nov 6:117(45):764-774. doi: 10.3238/arztebl.2020.0764. Epub [PubMed PMID: 33533331]
Hamilton AL, Kamm MA, Ng SC, Morrison M. Proteus spp. as Putative Gastrointestinal Pathogens. Clinical microbiology reviews. 2018 Jul:31(3):. doi: 10.1128/CMR.00085-17. Epub 2018 Jun 13 [PubMed PMID: 29899011]
Redden M, Ghadiri M. Acute appendicitis with associated trichobezoar of feline hair. Journal of surgical case reports. 2022 Mar:2022(3):rjac133. doi: 10.1093/jscr/rjac133. Epub 2022 Mar 29 [PubMed PMID: 35355580]
Level 3 (low-level) evidenceCorrea J, Jimeno J, Vallverdu H, Bizzoca C, Collado-Roura F, Estalella L, Hermoso J, Silva N, Sanchez-Pradell C, Parés D. Correlation between intraoperative surgical diagnosis of complicated acute appendicitis and the pathology report: clinical implications. Surgical infections. 2015 Feb:16(1):41-4. doi: 10.1089/sur.2013.155. Epub [PubMed PMID: 25761079]
Level 2 (mid-level) evidenceHoffmann JC, Trimborn CP, Hoffmann M, Schröder R, Förster S, Dirks K, Tannapfel A, Anthuber M, Hollerweger A. Classification of acute appendicitis (CAA): treatment directed new classification based on imaging (ultrasound, computed tomography) and pathology. International journal of colorectal disease. 2021 Nov:36(11):2347-2360. doi: 10.1007/s00384-021-03940-8. Epub 2021 Jun 18 [PubMed PMID: 34143276]
Snyder MJ, Guthrie M, Cagle S. Acute Appendicitis: Efficient Diagnosis and Management. American family physician. 2018 Jul 1:98(1):25-33 [PubMed PMID: 30215950]
van Aerts RMM, van de Laarschot LFM, Banales JM, Drenth JPH. Clinical management of polycystic liver disease. Journal of hepatology. 2018 Apr:68(4):827-837. doi: 10.1016/j.jhep.2017.11.024. Epub 2017 Nov 24 [PubMed PMID: 29175241]
Iwamoto Y, Onishi T, Suzuki R, Arima K, Sugimura Y. Uretero-appendiceal fistula. International journal of urology : official journal of the Japanese Urological Association. 2008 Feb:15(2):180-1. doi: 10.1111/j.1442-2042.2007.01952.x. Epub [PubMed PMID: 18269461]
Level 3 (low-level) evidenceYang HR, Wang YC, Chung PK, Chen WK, Jeng LB, Chen RJ. Laboratory tests in patients with acute appendicitis. ANZ journal of surgery. 2006 Jan-Feb:76(1-2):71-4 [PubMed PMID: 16483301]
Level 2 (mid-level) evidenceWithers AS, Grieve A, Loveland JA. Correlation of white cell count and CRP in acute appendicitis in paediatric patients. South African journal of surgery. Suid-Afrikaanse tydskrif vir chirurgie. 2019 Dec:57(4):40 [PubMed PMID: 31773931]
Rao PM. Cecal apical changes with appendicitis: diagnosing appendicitis when the appendix is borderline abnormal or not seen. Journal of computer assisted tomography. 1999 Jan-Feb:23(1):55-9 [PubMed PMID: 10050808]
Pooler BD, Repplinger MD, Reeder SB, Pickhardt PJ. MRI of the Nontraumatic Acute Abdomen: Description of Findings and Multimodality Correlation. Gastroenterology clinics of North America. 2018 Sep:47(3):667-690. doi: 10.1016/j.gtc.2018.04.010. Epub 2018 Jul 7 [PubMed PMID: 30115443]
Swenson DW, Ayyala RS, Sams C, Lee EY. Practical Imaging Strategies for Acute Appendicitis in Children. AJR. American journal of roentgenology. 2018 Oct:211(4):901-909. doi: 10.2214/AJR.18.19778. Epub 2018 Aug 14 [PubMed PMID: 30106612]
Kim DW, Suh CH, Yoon HM, Kim JR, Jung AY, Lee JS, Cho YA. Visibility of Normal Appendix on CT, MRI, and Sonography: A Systematic Review and Meta-Analysis. AJR. American journal of roentgenology. 2018 Sep:211(3):W140-W150. doi: 10.2214/AJR.17.19321. Epub 2018 Jul 24 [PubMed PMID: 30040469]
Level 1 (high-level) evidenceHwang ME. Sonography and Computed Tomography in Diagnosing Acute Appendicitis. Radiologic technology. 2018 Jan:89(3):224-237 [PubMed PMID: 29298941]
Kave M, Parooie F, Salarzaei M. Pregnancy and appendicitis: a systematic review and meta-analysis on the clinical use of MRI in diagnosis of appendicitis in pregnant women. World journal of emergency surgery : WJES. 2019:14():37. doi: 10.1186/s13017-019-0254-1. Epub 2019 Jul 22 [PubMed PMID: 31367227]
Level 1 (high-level) evidenceAwayshih MMA, Nofal MN, Yousef AJ. Evaluation of Alvarado score in diagnosing acute appendicitis. The Pan African medical journal. 2019:34():15. doi: 10.11604/pamj.2019.34.15.17803. Epub 2019 Sep 6 [PubMed PMID: 31762884]
CODA Collaborative, Flum DR, Davidson GH, Monsell SE, Shapiro NI, Odom SR, Sanchez SE, Drake FT, Fischkoff K, Johnson J, Patton JH, Evans H, Cuschieri J, Sabbatini AK, Faine BA, Skeete DA, Liang MK, Sohn V, McGrane K, Kutcher ME, Chung B, Carter DW, Ayoung-Chee P, Chiang W, Rushing A, Steinberg S, Foster CS, Schaetzel SM, Price TP, Mandell KA, Ferrigno L, Salzberg M, DeUgarte DA, Kaji AH, Moran GJ, Saltzman D, Alam HB, Park PK, Kao LS, Thompson CM, Self WH, Yu JT, Wiebusch A, Winchell RJ, Clark S, Krishnadasan A, Fannon E, Lavallee DC, Comstock BA, Bizzell B, Heagerty PJ, Kessler LG, Talan DA. A Randomized Trial Comparing Antibiotics with Appendectomy for Appendicitis. The New England journal of medicine. 2020 Nov 12:383(20):1907-1919. doi: 10.1056/NEJMoa2014320. Epub 2020 Oct 5 [PubMed PMID: 33017106]
Level 1 (high-level) evidenceHansson J, Körner U, Khorram-Manesh A, Solberg A, Lundholm K. Randomized clinical trial of antibiotic therapy versus appendicectomy as primary treatment of acute appendicitis in unselected patients. The British journal of surgery. 2009 May:96(5):473-81. doi: 10.1002/bjs.6482. Epub [PubMed PMID: 19358184]
Level 1 (high-level) evidenceStyrud J, Eriksson S, Nilsson I, Ahlberg G, Haapaniemi S, Neovius G, Rex L, Badume I, Granström L. Appendectomy versus antibiotic treatment in acute appendicitis. a prospective multicenter randomized controlled trial. World journal of surgery. 2006 Jun:30(6):1033-7 [PubMed PMID: 16736333]
Level 1 (high-level) evidenceSalminen P, Tuominen R, Paajanen H, Rautio T, Nordström P, Aarnio M, Rantanen T, Hurme S, Mecklin JP, Sand J, Virtanen J, Jartti A, Grönroos JM. Five-Year Follow-up of Antibiotic Therapy for Uncomplicated Acute Appendicitis in the APPAC Randomized Clinical Trial. JAMA. 2018 Sep 25:320(12):1259-1265. doi: 10.1001/jama.2018.13201. Epub [PubMed PMID: 30264120]
Level 1 (high-level) evidenceVons C, Barry C, Maitre S, Pautrat K, Leconte M, Costaglioli B, Karoui M, Alves A, Dousset B, Valleur P, Falissard B, Franco D. Amoxicillin plus clavulanic acid versus appendicectomy for treatment of acute uncomplicated appendicitis: an open-label, non-inferiority, randomised controlled trial. Lancet (London, England). 2011 May 7:377(9777):1573-9. doi: 10.1016/S0140-6736(11)60410-8. Epub [PubMed PMID: 21550483]
Level 1 (high-level) evidenceWriting Group for the CODA Collaborative, Zhang IY, Voldal EC, Davidson GH, Liao JM, Thompson CM, Self WH, Kao LS, Cherry-Bukowiec J, Raghavendran K, Kaji AH, DeUgarte DA, Gonzalez E, Mandell KA, Ohe K, Siparsky N, Price TP, Evans DC, Victory J, Chiang W, Jones A, Kutcher ME, Ciomperlik H, Liang MK, Evans HL, Faine BA, Neufeld M, Sanchez SE, Krishnadasan A, Comstock BA, Heagerty PJ, Lawrence SO, Monsell SE, Fannon EEC, Kessler LG, Talan DA, Flum DR. Association of Patient Belief About Success of Antibiotics for Appendicitis and Outcomes: A Secondary Analysis of the CODA Randomized Clinical Trial. JAMA surgery. 2022 Dec 1:157(12):1080-1087. doi: 10.1001/jamasurg.2022.4765. Epub [PubMed PMID: 36197656]
Level 1 (high-level) evidenceSartelli M, Baiocchi GL, Di Saverio S, Ferrara F, Labricciosa FM, Ansaloni L, Coccolini F, Vijayan D, Abbas A, Abongwa HK, Agboola J, Ahmed A, Akhmeteli L, Akkapulu N, Akkucuk S, Altintoprak F, Andreiev AL, Anyfantakis D, Atanasov B, Bala M, Balalis D, Baraket O, Bellanova G, Beltran M, Melo RB, Bini R, Bouliaris K, Brunelli D, Castillo A, Catani M, Che Jusoh A, Chichom-Mefire A, Cocorullo G, Coimbra R, Colak E, Costa S, Das K, Delibegovic S, Demetrashvili Z, Di Carlo I, Kiseleva N, El Zalabany T, Faro M, Ferreira M, Fraga GP, Gachabayov M, Ghnnam WM, Giménez Maurel T, Gkiokas G, Gomes CA, Griffiths E, Guner A, Gupta S, Hecker A, Hirano ES, Hodonou A, Hutan M, Ioannidis O, Isik A, Ivakhov G, Jain S, Jokubauskas M, Karamarkovic A, Kauhanen S, Kaushik R, Kavalakat A, Kenig J, Khokha V, Khor D, Kim D, Kim JI, Kong V, Lasithiotakis K, Leão P, Leon M, Litvin A, Lohsiriwat V, López-Tomassetti Fernandez E, Lostoridis E, Maciel J, Major P, Dimova A, Manatakis D, Marinis A, Martinez-Perez A, Marwah S, McFarlane M, Mesina C, Pędziwiatr M, Michalopoulos N, Misiakos E, Mohamedahmed A, Moldovanu R, Montori G, Mysore Narayana R, Negoi I, Nikolopoulos I, Novelli G, Novikovs V, Olaoye I, Omari A, Ordoñez CA, Ouadii M, Ozkan Z, Pal A, Palini GM, Partecke LI, Pata F, Pędziwiatr M, Pereira Júnior GA, Pintar T, Pisarska M, Ploneda-Valencia CF, Pouggouras K, Prabhu V, Ramakrishnapillai P, Regimbeau JM, Reitz M, Rios-Cruz D, Saar S, Sakakushev B, Seretis C, Sazhin A, Shelat V, Skrovina M, Smirnov D, Spyropoulos C, Strzałka M, Talving P, Teixeira Gonsaga RA, Theobald G, Tomadze G, Torba M, Tranà C, Ulrych J, Uzunoğlu MY, Vasilescu A, Occhionorelli S, Venara A, Vereczkei A, Vettoretto N, Vlad N, Walędziak M, Yilmaz TU, Yuan KC, Yunfeng C, Zilinskas J, Grelpois G, Catena F. Prospective Observational Study on acute Appendicitis Worldwide (POSAW). World journal of emergency surgery : WJES. 2018:13():19. doi: 10.1186/s13017-018-0179-0. Epub 2018 Apr 16 [PubMed PMID: 29686725]
Level 2 (mid-level) evidenceHarnoss JC, Zelienka I, Probst P, Grummich K, Müller-Lantzsch C, Harnoss JM, Ulrich A, Büchler MW, Diener MK. Antibiotics Versus Surgical Therapy for Uncomplicated Appendicitis: Systematic Review and Meta-analysis of Controlled Trials (PROSPERO 2015: CRD42015016882). Annals of surgery. 2017 May:265(5):889-900. doi: 10.1097/SLA.0000000000002039. Epub [PubMed PMID: 27759621]
Level 1 (high-level) evidenceKumar S, Jalan A, Patowary BN, Shrestha S. Laparoscopic Appendectomy Versus Open Appendectomy for Acute Appendicitis: A Prospective Comparative Study. Kathmandu University medical journal (KUMJ). 2016 Jul-Sept.:14(55):244-248 [PubMed PMID: 28814687]
Level 2 (mid-level) evidenceZani A, Hall NJ, Rahman A, Morini F, Pini Prato A, Friedmacher F, Koivusalo A, van Heurn E, Pierro A. European Paediatric Surgeons' Association Survey on the Management of Pediatric Appendicitis. European journal of pediatric surgery : official journal of Austrian Association of Pediatric Surgery ... [et al] = Zeitschrift fur Kinderchirurgie. 2019 Feb:29(1):53-61. doi: 10.1055/s-0038-1668139. Epub 2018 Aug 15 [PubMed PMID: 30112745]
Level 3 (low-level) evidenceAntonacci N, Ricci C, Taffurelli G, Monari F, Del Governatore M, Caira A, Leone A, Cervellera M, Minni F, Cola B. Laparoscopic appendectomy: Which factors are predictors of conversion? A high-volume prospective cohort study. International journal of surgery (London, England). 2015 Sep:21():103-7. doi: 10.1016/j.ijsu.2015.06.089. Epub 2015 Jul 29 [PubMed PMID: 26231996]
Thambidorai CR, Aman Fuad Y. Laparoscopic appendicectomy for complicated appendicitis in children. Singapore medical journal. 2008 Dec:49(12):994-7 [PubMed PMID: 19122949]
Siribumrungwong B, Chantip A, Noorit P, Wilasrusmee C, Ungpinitpong W, Chotiya P, Leerapan B, Woratanarat P, McEvoy M, Attia J, Thakkinstian A. Comparison of Superficial Surgical Site Infection Between Delayed Primary Versus Primary Wound Closure in Complicated Appendicitis: A Randomized Controlled Trial. Annals of surgery. 2018 Apr:267(4):631-637. doi: 10.1097/SLA.0000000000002464. Epub [PubMed PMID: 28796014]
Level 1 (high-level) evidenceTurk E, Acimis NM, Karaca F, Edirne Y, Tan A, Kilic C. The effect on postoperative pain of pulling the rectus muscle medially during open appendectomy surgery. Minerva chirurgica. 2014 Jun:69(3):141-6 [PubMed PMID: 24970302]
Hucl T, Benes M, Kocik M, Splichalova A, Maluskova J, Krak M, Lanska V, Heczkova M, Kieslichova E, Oliverius M, Spicak J. Comparison of Inflammatory Response to Transgastric and Transcolonic NOTES. Gastroenterology research and practice. 2016:2016():7320275. doi: 10.1155/2016/7320275. Epub 2016 Jun 14 [PubMed PMID: 27403157]
Khashab MA, Kalloo AN. NOTES: current status and new horizons. Gastroenterology. 2012 Apr:142(4):704-710.e1. doi: 10.1053/j.gastro.2012.02.022. Epub 2012 Feb 17 [PubMed PMID: 22349111]
Level 3 (low-level) evidenceAhmed K, Wang TT, Patel VM, Nagpal K, Clark J, Ali M, Deeba S, Ashrafian H, Darzi A, Athanasiou T, Paraskeva P. The role of single-incision laparoscopic surgery in abdominal and pelvic surgery: a systematic review. Surgical endoscopy. 2011 Feb:25(2):378-96. doi: 10.1007/s00464-010-1208-6. Epub 2010 Jul 10 [PubMed PMID: 20623239]
Level 1 (high-level) evidenceJiang J, Wu Y, Tang Y, Shen Z, Chen G, Huang Y, Zheng S, Zheng Y, Dong R. A novel nomogram for the differential diagnosis between advanced and early appendicitis in pediatric patients. Biomarkers in medicine. 2019 Oct:13(14):1157-1173. doi: 10.2217/bmm-2019-0036. Epub 2019 Sep 27 [PubMed PMID: 31559834]
Van de Moortele M, De Hertogh G, Sagaert X, Van Cutsem E. Appendiceal cancer : a review of the literature. Acta gastro-enterologica Belgica. 2020 Jul-Sep:83(3):441-448 [PubMed PMID: 33094592]
Zhang K, Meyerson C, Kassardjian A, Westbrook LM, Zheng W, Wang HL. Goblet Cell Carcinoid/Carcinoma: An Update. Advances in anatomic pathology. 2019 Mar:26(2):75-83. doi: 10.1097/PAP.0000000000000222. Epub [PubMed PMID: 30601149]
Level 3 (low-level) evidenceMarte A, Sabatino MD, Cautiero P, Accardo M, Romano M, Parmeggiani P. Unexpected finding of laparoscopic appendectomy: appendix MALT lymphoma in children. Pediatric surgery international. 2008 Apr:24(4):471-3 [PubMed PMID: 17628810]
Level 3 (low-level) evidenceXie X, Zhou Z, Song Y, Li W, Diao D, Dang C, Zhang H. The Management and Prognostic Prediction of Adenocarcinoma of Appendix. Scientific reports. 2016 Dec 16:6():39027. doi: 10.1038/srep39027. Epub 2016 Dec 16 [PubMed PMID: 27982068]
Morano WF, Gleeson EM, Sullivan SH, Padmanaban V, Mapow BL, Shewokis PA, Esquivel J, Bowne WB. Clinicopathological Features and Management of Appendiceal Mucoceles: A Systematic Review. The American surgeon. 2018 Feb 1:84(2):273-281 [PubMed PMID: 29580358]
Level 1 (high-level) evidenceCalis H. Morbidity and Mortality in Appendicitis in the Elderly. Journal of the College of Physicians and Surgeons--Pakistan : JCPSP. 2018 Nov:28(11):875-878. doi: 10.29271/jcpsp.2018.11.875. Epub [PubMed PMID: 30369383]
Keller CA, Dudley RM, Huycke EM, Chow RB, Ali A. Stump appendicitis. Radiology case reports. 2022 Jul:17(7):2534-2536. doi: 10.1016/j.radcr.2022.04.034. Epub 2022 May 13 [PubMed PMID: 35601384]
Level 3 (low-level) evidenceGorter RR, Eker HH, Gorter-Stam MA, Abis GS, Acharya A, Ankersmit M, Antoniou SA, Arolfo S, Babic B, Boni L, Bruntink M, van Dam DA, Defoort B, Deijen CL, DeLacy FB, Go PM, Harmsen AM, van den Helder RS, Iordache F, Ket JC, Muysoms FE, Ozmen MM, Papoulas M, Rhodes M, Straatman J, Tenhagen M, Turrado V, Vereczkei A, Vilallonga R, Deelder JD, Bonjer J. Diagnosis and management of acute appendicitis. EAES consensus development conference 2015. Surgical endoscopy. 2016 Nov:30(11):4668-4690 [PubMed PMID: 27660247]
Level 3 (low-level) evidenceSmith MP, Katz DS, Lalani T, Carucci LR, Cash BD, Kim DH, Piorkowski RJ, Small WC, Spottswood SE, Tulchinsky M, Yaghmai V, Yee J, Rosen MP. ACR Appropriateness Criteria® Right Lower Quadrant Pain--Suspected Appendicitis. Ultrasound quarterly. 2015 Jun:31(2):85-91. doi: 10.1097/RUQ.0000000000000118. Epub [PubMed PMID: 25364964]
Schoel L, Maizlin II, Koppelmann T, Onwubiko C, Shroyer M, Douglas A, Russell RT. Improving imaging strategies in pediatric appendicitis: a quality improvement initiative. The Journal of surgical research. 2018 Oct:230():131-136. doi: 10.1016/j.jss.2018.04.043. Epub 2018 May 25 [PubMed PMID: 30100029]
Level 2 (mid-level) evidenceZosimas D, Lykoudis PM, Pilavas A, Burke J, Leung P, Strano G, Shatkar V. Open versus laparoscopic appendicectomy in acute appendicitis: results of a district general hospital. South African journal of surgery. Suid-Afrikaanse tydskrif vir chirurgie. 2018 Jun:56(2):59-62 [PubMed PMID: 30010266]
Schneuer FJ, Adams SE, Bentley JP, Holland AJ, Huckel Schneider C, White L, Nassar N. A population-based comparison of the post-operative outcomes of open and laparoscopic appendicectomy in children. The Medical journal of Australia. 2018 Jul 16:209(2):80-85 [PubMed PMID: 29976133]