Introduction
Volar splinting of the upper extremity can be employed to immobilize hard and soft tissue injuries in addition to painful atraumatic conditions. Hard tissue skeletal injuries that may benefit from volar splinting include distal radius fractures, Colles fractures, and metacarpal or carpal fractures, excluding fractures of the first metacarpal and trapezium. Basic splinting guidelines of skeletal pathology require immobilization of the joint above and below the lesion. Exceptions to this rule include metaphyseal fractures, such as Colles or Smith fractures; metaphyseal fractures behave like injuries within the joint. For more proximal shaft fractures, the principle of volar splinting expands into sugar-tong or Muenster-type splinting, extending above the elbow.[1][2] Other conditions amenable to volar splinting include acute gouty arthritis, carpal tunnel syndrome, and radial nerve palsy.
Splinting is an adjunct to elevation and ice. Splinting improves patient comfort, facilitates recovery, and protects from further injury. Splints may be used for comfort as a temporizing measure for wrist and hand dislocations or fracture subluxations while awaiting definitive care.[3] Splints differ from casts in that the noncircumferential bandage allows for some degree of soft tissue swelling without undue constriction. Splints can be easily removed for wound care. Splinting may be the definitive treatment or temporary treatment before casting. Although plaster is considered the traditional splinting material, padded fiberglass or preformed plastic splints are commonly encountered in clinical practice.[4]
Anatomy and Physiology
Register For Free And Read The Full Article
Search engine and full access to all medical articles
10 free questions in your specialty
Free CME/CE Activities
Free daily question in your email
Save favorite articles to your dashboard
Emails offering discounts
Learn more about a Subscription to StatPearls Point-of-Care
Anatomy and Physiology
A fundamental principle of fracture immobilization with splinting is that a splint must extend from at least one joint above to one below the fracture. For example, when splinting a metacarpal fracture, the splint must extend from the mid-forearm above the wrist to beyond the metacarpophalangeal joints. The careful examination and dressing of wounds should precede splint application. The neurovascular status of the affected extremity must be assessed and documented before splint application.
Indications
Volar splinting may be indicated to immobilize hard tissue injuries such as distal radial or ulnar fractures and certain metacarpal or carpal fractures, excluding fractures of the first metacarpal or trapezium.[5] Soft tissue injuries that may benefit from volar splinting include extensive skin lacerations and structural injuries to tendons or ligaments.[6] A volar splint may provide symptomatic relief from inflamed, painful, but uninjured joints in patients with acute gout, active rheumatoid arthritis, or other painful inflammatory conditions.[7][8]
Contraindications
There are no specific contraindications to volar splinting. However, some clinical situations may warrant special consideration before placing a volar splint. Burns, open or contaminated wounds, or unstable fracture patterns must be carefully evaluated to determine if the benefits of a volar splint will outweigh the risks. If the affected limb is tense and edematous, monitoring for compartment syndrome and rapidly extending soft tissue inflammation or infection will be required, potentially making splinting less desirable.
Equipment
The following equipment is required when fashioning and placing a volar splint:
- Plaster or padded fiberglass
- Stockinette
- Undercast or cotton padding
- Cool water
- Elastic bandage
- Sling
Personnel
Volar splinting can be performed by appropriately trained personnel, including physicians, advanced practice providers, nurses, athletic trainers, or technicians. A single operator can perform the procedure.
Preparation
The clinical situation dictates the length of a volar splint. For a Colles or wrist fracture, the splint must extend from the distal palmar crease to 4 to 5 cm distal to the antecubital fossa. For metacarpal fractures, including Boxer fractures, the splint should extend beyond the metacarpophalangeal joint. For phalangeal fractures, the splint should extend beyond the tips of the digits.
In preparing equipment to place a volar splint, the operator must keep in mind that while plaster is more pliable than fiberglass, it does take longer to set. The hardening of the splint material occurs via an exothermic reaction. The amount of heat released during this reaction is proportional to the number of layers of casting material and the water temperature. When utilizing plaster for volar splinting, the layers of plaster should be limited to 12; 8 to 10 layers will usually suffice. Cool water allows time to mold the splint and reduces the risk of burn.
Technique or Treatment
Pain Management
The manipulation of acute fractures is painful. Using analgesics and anesthesia ensures comfort and muscle relaxation to reduce a fracture and apply a splint effectively.[9] Children are more likely to require general anesthesia than adults, most of whom will tolerate the procedure with regional anesthesia and adjunctive analgesia.[10] A viable substitute for regional anesthesia is the hematoma block.
To perform a hematoma block, insert a needle into the fracture site after palpating the fracture ends. Aspiration of blood and fat droplets confirms the correct position of the needle. Aspirate as much of the hematoma as possible. Inject 5 to 10 mL of local anesthesia into the fracture.[11] The hematoma will function as a fluid medium, allowing the anesthetic to diffuse within the fracture site. [12] However, most patients do not seek care until hours after the fracture, when the hematoma has already formed and cannot be aspirated. Hematoma blocks are not appropriate for patients with open fractures.[13]
Parenteral analgesics should be administered before and after fracture manipulation and splint application to relieve pain without significant sedation. Pain that persists after rest, splinting, elevation, and adequate analgesia may indicate compartment syndrome, which requires surgical consultation.
Fracture Reduction
The closed reduction of a displaced fracture requires initial distraction, deformity alignment by connecting the bone ends, and length stabilization. Sustained gentle traction that can stretch the soft tissue surrounding the fracture to realign the bony ends is required. The amount of traction applied should be greater than the magnitude of the muscle spasm. Translation of the bone ends during distraction allows fracture reduction.[14] By applying traction, intact tendons, muscles, and periosteum may immediately reduce regions of fracture comminution. Alternative fracture manipulation techniques are needed for displaced fractures with periosteal hinges and fractures that do not align with traction.[15][16] Alternative methods of fracture reduction involve simulating the injurious impact by worsening the deformity, disengaging fracture ends, and angulation correction using the distraction force.[17]
Positioning of the Affected Limb
Of the two forms of radioulnar joint instability, dorsal dislocations from a fall onto an outstretched hand are the most common. Volar dislocations are less common and occur with forceful supination.[18]
Distal extra-articular radius fractures with <5 mm of shortening and dorsal angulation of <5° require closed reduction and casting.[19] A Colles fracture demonstrates supination, dorsal tilt, and volar angulation of the distal radius.[20][21] The splinting posture of the affected extremity is pronation with slight palmar flexion and ulnar deviation to preserve fracture reduction and maintain a neutral wrist position. Excessive palmar flexion and ulnar deviation must be avoided. This position may induce increased stiffness in patients with degenerative joint disease. The position may raise carpal tunnel pressure. [22]
Smith fractures commonly occur secondary to falling on a flexed wrist or a direct blow to the dorsal aspect of the wrist. The distal fragment exhibits volar displacement, dorsal angulation, and pronation in a Smith fracture. The splinting posture requires extension and supination of the wrist.[23]
Unicortical fractures of the forearm and forearm fractures that are undisplaced or mildly displaced, characterized by less than 50% displacement and 10 degrees of angulation, are candidates for conservative management. Forearm fractures with volar angulation should be treated with immobilization in pronation, and those with dorsal angulation should be immobilized in supination.[24] The appropriate forearm rotation for immobilization will depend on the fracture location and any accompanying deforming forces. Fractures of the proximal third are splinted in supination, fractures of the middle third are immobilized in a neutral position, and fractures of the distal third are immobilized in pronation.[24]
Restoration of digital function after flexor and extensor tendon reconstruction remains one of the most challenging clinical and operative dilemmas in hand surgery. The posture of safe immobilization (POSI) is the appropriate position to immobilize the hand safely after a surgical procedure or injury. In the POSI, the wrist is dorsiflexed between 0 and 30°, the metacarpophalangeal joints are flexed between 70 to 90°, and the interphalangeal joints are fully extended.[25]
Splinting Technique
The neurovascular status of the affected limb should be assessed before splint application. Apply adequate stockinette and cotton undercast padding to prevent heat penetration. Extra padding over bony prominences, such as the ulnar styloid, and at the ends of the splint will help prevent pressure sores. The stockinette must cover the entire splint area and extend approximately 10 cm beyond either end of the planned splint location. A 2- to 3-in stockinette width is typically used for the upper limbs.[26] Wrap cotton padding concentrically around the extremity rolling from one end to the other, with each layer covering the preceding layer by 50%. This method automatically provides 2 layers of padding. The padding should reach 2 to 3 cm beyond the intended boundaries of the splint without being constrictive. To prevent regions of excessive wrinkling and subsequent pressure, joints should be put in their functional position before, during, and after applying padding. A 2- to 4-inch padding is typically used for the upper extremity.[27]
Plaster and synthetic casting materials are commonly used to splint fractures. Prepare a container of water at room temperature before starting the splinting procedure. Water that is too warm will hasten the setting process and shorten the time available for molding. The risk of severe skin burns increases with shortened set times. Cool water is encouraged if additional time is required for splint application.
The side of the extremity contralateral to the fracture should be measured to calculate the necessary length of the casting material. When creating a plaster splint, fold the plaster into layers and dip it into the container of water at an angle of 45 degrees. Completely immerse the plaster. Once the bubbling ceases, the plaster may be removed from the water. Squeeze out the excess water using longitudinal compression massage. If the splinting material is too long, the edges may be folded over to achieve the desired length. For an average-sized adult, an upper extremity splint will require approximately 10 layers of casting material.[28] The splint will generate more heat and weigh more if excess sheets are used.[29]
The sugar-tong splint is an appropriate treatment option for forearm and distal radius fractures. The sugar-tong splint originates at the distal palmar crease and extends along the volar forearm, around the elbow to the dorsum of the metacarpophalangeal joints.[30] An alternative upper extremity splint is the long arm posterior splint that extends from the axilla over the posterior surface of the 90-degree flexed elbow and along the ulna to the proximal palmar crease.[31]
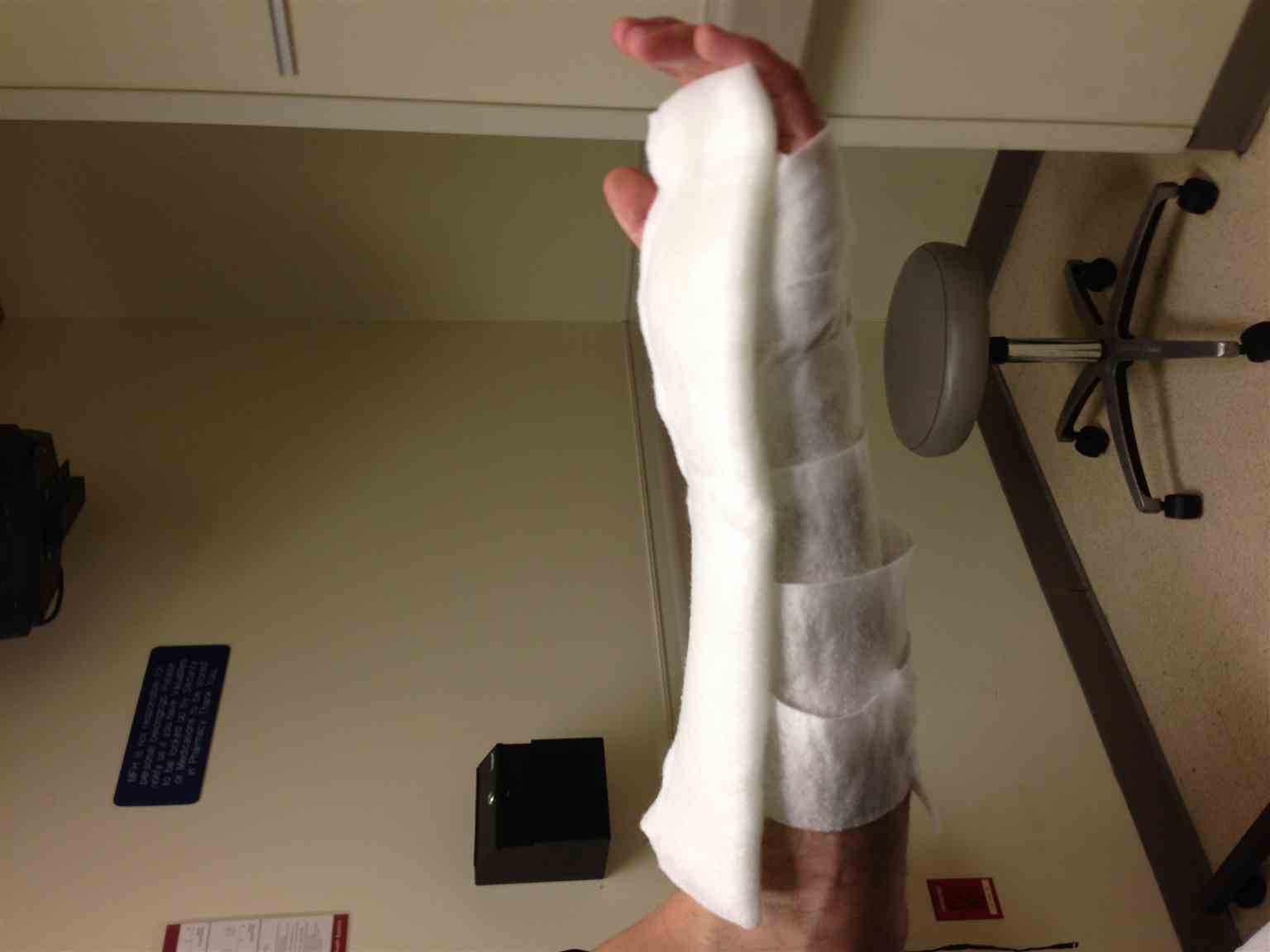
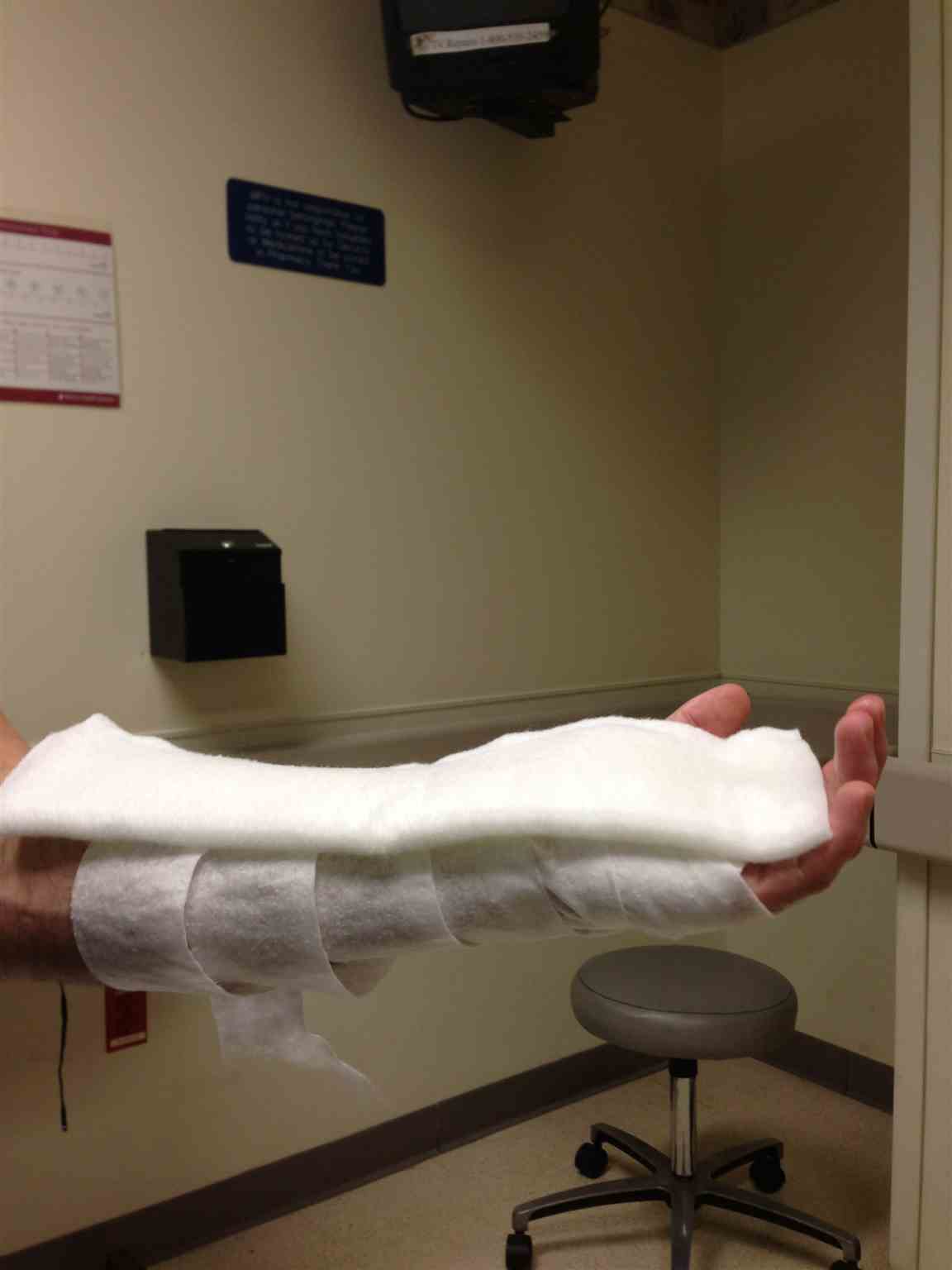
The elastic wrap holds the splint in place and should be applied to accommodate soft tissue swelling but limit movement. Neurovascular status should be reassessed after splint application. A sling is used for elevation and protection. (see Images. Volar Splint and Volar Splint Side View)
Splinting Aftercare
The length of immobilization and time to reevaluation varies greatly depending on the location, nature, and stability of the fracture. Each injury must be evaluated, handled, and monitored individually. Instruct the patient to keep the splint clean and dry. The extremity should be elevated, and an ice pack applied to the splint for 20 minutes every few hours. If the fingers become cold, blue, numb, or painful, the patient should seek medical attention. Removal of the splint allows for wound care in some cases.[32][1]
Complications
Complications of volar splinting include joint stiffness, thermal burns, pressure ulcers, wound infections, and compartment syndrome.
Clinical Significance
Volar splinting is a valuable technique for managing traumatic and atraumatic conditions of the hand and wrist. The splint immobilizes and supports the metacarpals and carpals while allowing room for swelling. The splint can be removed to examine wounds that may accompany the injury.[1]
Enhancing Healthcare Team Outcomes
Healthcare professionals can work as an interprofessional team to improve outcomes for patients who require volar splinting by utilizing collaborative communication and a patient-centered approach. Not all patients with injuries to the upper extremity are candidates for volar splinting. Each healthcare team member should actively ensure that the patient understands and is willing to participate in the care and monitoring of their volar splint before it is placed. While volar splinting may be the definitive therapy for some clinical conditions, most patients require a follow-up appointment within 1 week. Patient education is imperative as the patient will be responsible for caring for their splint in the interim.
Media
(Click Image to Enlarge)
References
Hill JR, Navo PD, Bouz G, Azad A, Pannell W, Alluri RK, Ghiassi A. Immobilization following Distal Radius Fractures: A Randomized Clinical Trial. Journal of wrist surgery. 2018 Nov:7(5):409-414. doi: 10.1055/s-0038-1667302. Epub 2018 Aug 7 [PubMed PMID: 30349755]
Level 1 (high-level) evidenceKralj R, Barcot Z, Vlahovic T, Kurtanjek M, Petracic I. The patterns of phalangeal fractures in children and adolescents: a review of 512 cases. Handchirurgie, Mikrochirurgie, plastische Chirurgie : Organ der Deutschsprachigen Arbeitsgemeinschaft fur Handchirurgie : Organ der Deutschsprachigen Arbeitsgemeinschaft fur Mikrochirurgie der Peripheren Nerven und Gefasse : Organ der V.... 2019 Feb:51(1):49-53. doi: 10.1055/a-0824-7167. Epub 2019 Feb 13 [PubMed PMID: 30759479]
Level 3 (low-level) evidenceSaitta BH, Wolf JM. Treating Proximal Interphalangeal Joint Dislocations. Hand clinics. 2018 May:34(2):139-148. doi: 10.1016/j.hcl.2017.12.004. Epub [PubMed PMID: 29625634]
Ho PC, Tse WL, Wong CW. Palmer Midcarpal Instability: An Algorithm of Diagnosis and Surgical Management. Journal of wrist surgery. 2017 Nov:6(4):262-275. doi: 10.1055/s-0037-1606379. Epub 2017 Aug 30 [PubMed PMID: 29085727]
Prucz RB, Friedrich JB. Finger joint injuries. Clinics in sports medicine. 2015 Jan:34(1):99-116. doi: 10.1016/j.csm.2014.09.002. Epub 2014 Nov 25 [PubMed PMID: 25455398]
Wada T, Oda T. Mallet fingers with bone avulsion and DIP joint subluxation. The Journal of hand surgery, European volume. 2015 Jan:40(1):8-15. doi: 10.1177/1753193414554772. Epub 2014 Oct 21 [PubMed PMID: 25336471]
Gurnani N, Hoogendoorn J, Rhemrev S. [Mallet finger: surgery versus splinting]. Nederlands tijdschrift voor geneeskunde. 2014:158():A6941 [PubMed PMID: 24618239]
Adrienne C, Manigandan C. Inpatient occupational therapists hand-splinting practice for clients with stroke: A cross-sectional survey from Ireland. Journal of neurosciences in rural practice. 2011 Jul:2(2):141-9. doi: 10.4103/0976-3147.83579. Epub [PubMed PMID: 21897676]
Level 2 (mid-level) evidenceMitchell SAT, Majuta LA, Mantyh PW. New Insights in Understanding and Treating Bone Fracture Pain. Current osteoporosis reports. 2018 Aug:16(4):325-332. doi: 10.1007/s11914-018-0446-8. Epub [PubMed PMID: 29948820]
Level 3 (low-level) evidenceAmmann S, Schoell E, Nieves Ortega R, Bingisser R. Ultrasound-guided regional anaesthesia and reduction of distal radius fractures in an emergency department. Swiss medical weekly. 2020 Sep 21:150():w20288. doi: 10.4414/smw.2020.20288. Epub 2020 Sep 23 [PubMed PMID: 33035349]
Tseng PT, Leu TH, Chen YW, Chen YP. Hematoma block or procedural sedation and analgesia, which is the most effective method of anesthesia in reduction of displaced distal radius fracture? Journal of orthopaedic surgery and research. 2018 Mar 27:13(1):62. doi: 10.1186/s13018-018-0772-7. Epub 2018 Mar 27 [PubMed PMID: 29580286]
Maleitzke T, Plachel F, Fleckenstein FN, Wichlas F, Tsitsilonis S. Haematoma block: a safe method for pre-surgical reduction of distal radius fractures. Journal of orthopaedic surgery and research. 2020 Aug 26:15(1):351. doi: 10.1186/s13018-020-01819-y. Epub 2020 Aug 26 [PubMed PMID: 32843043]
Younge D. Haematoma block for fractures of the wrist: a cause of compartment syndrome. Journal of hand surgery (Edinburgh, Scotland). 1989 May:14(2):194-5 [PubMed PMID: 2746120]
Level 3 (low-level) evidenceAnderson AB, Tintle SM. Closed Reduction Techniques for Distal Radius Fractures and Appropriate Casting Methods. Hand clinics. 2021 May:37(2):239-245. doi: 10.1016/j.hcl.2021.02.006. Epub [PubMed PMID: 33892877]
Bégué T, Judet T, de Thomasson E, Rouvreau P, de Cheveigné C, Garreau de Loubresse C, Boury G. [Treatment of comminuted fractures of the lower end of the radius with internal osteosynthesis, traction and early mobilization]. Annales de chirurgie de la main et du membre superieur : organe officiel des societes de chirurgie de la main = Annals of hand and upper limb surgery. 1995:14(1):5-13 [PubMed PMID: 7535549]
Level 3 (low-level) evidenceGitard R, Lagrange M. [Comminuted fractures of the lower end of the radius. Treatment by traction-suspension]. La Nouvelle presse medicale. 1982 Nov 20:11(47):3505-6 [PubMed PMID: 7155859]
Handoll HH, Madhok R. Closed reduction methods for treating distal radial fractures in adults. The Cochrane database of systematic reviews. 2003:2003(1):CD003763 [PubMed PMID: 12535486]
Level 1 (high-level) evidenceQazi S, Graham D, Regal S, Tang P, Hammarstedt JE. Distal Radioulnar Joint Instability and Associated Injuries: A Literature Review. Journal of hand and microsurgery. 2021 Jul:13(3):123-131. doi: 10.1055/s-0041-1730886. Epub 2021 Jun 19 [PubMed PMID: 34539128]
Nana AD, Joshi A, Lichtman DM. Plating of the distal radius. The Journal of the American Academy of Orthopaedic Surgeons. 2005 May-Jun:13(3):159-71 [PubMed PMID: 15938605]
Meena S, Sharma P, Sambharia AK, Dawar A. Fractures of distal radius: an overview. Journal of family medicine and primary care. 2014 Oct-Dec:3(4):325-32. doi: 10.4103/2249-4863.148101. Epub [PubMed PMID: 25657938]
Level 3 (low-level) evidenceSummers K, Mabrouk A, Fowles SM. Colles Fracture. StatPearls. 2023 Jan:(): [PubMed PMID: 31971712]
Raittio L, Launonen A, Hevonkorpi T, Luokkala T, Kukkonen J, Reito A, Sumrein B, Laitinen M, Mattila VM. Comparison of volar-flexion, ulnar-deviation and functional position cast immobilization in the non-operative treatment of distal radius fracture in elderly patients: a pragmatic randomized controlled trial study protocol. BMC musculoskeletal disorders. 2017 Sep 18:18(1):401. doi: 10.1186/s12891-017-1759-y. Epub 2017 Sep 18 [PubMed PMID: 28923035]
Level 1 (high-level) evidenceSchroeder JD, Varacallo M. Smith Fracture Review. StatPearls. 2023 Jan:(): [PubMed PMID: 31613494]
Caruso G, Caldari E, Sturla FD, Caldaria A, Re DL, Pagetti P, Palummieri F, Massari L. Management of pediatric forearm fractures: what is the best therapeutic choice? A narrative review of the literature. Musculoskeletal surgery. 2021 Dec:105(3):225-234. doi: 10.1007/s12306-020-00684-6. Epub 2020 Oct 14 [PubMed PMID: 33058085]
Level 3 (low-level) evidenceDobson P, Taylor R, Dunkin C. Safe splinting in hand surgery. Annals of the Royal College of Surgeons of England. 2011 Jan:93(1):94 [PubMed PMID: 21418760]
Level 3 (low-level) evidenceWalthall J, Adame JD, Varacallo M. Long Arm Splinting. StatPearls. 2024 Jan:(): [PubMed PMID: 30020655]
Howes DS, Kaufman JJ. Plaster splints: techniques and indications. American family physician. 1984 Sep:30(3):215-21 [PubMed PMID: 6475704]
Vieira GC, Barbosa RI, Marcolino AM, Shimano AC, Elui VM, Fonseca MC. Influence of the number of layers of paris bandage plasters on the mechanical properties speciments used on orthopedic splints. Revista brasileira de fisioterapia (Sao Carlos (Sao Paulo, Brazil)). 2011 Sep-Oct:15(5):380-5 [PubMed PMID: 21877061]
Shaw DC, Heckman JD. Principles and techniques of splinting musculocutaneous injuries. Emergency medicine clinics of North America. 1984 May:2(2):391-407 [PubMed PMID: 6394308]
GARTLAND JJ. The sugar tong splint. The American journal of orthopedics. 1963 May:5():131 [PubMed PMID: 13946655]
Drozd M, Miles S, Davies J. Casting: above-elbow back slabs. Emergency nurse : the journal of the RCN Accident and Emergency Nursing Association. 2009 Jul:17(4):20-2 [PubMed PMID: 19639801]
Bracker MD, Ralph LP. The numb arm and hand. American family physician. 1995 Jan:51(1):103-16 [PubMed PMID: 7810463]