Introduction
Diseases of the appendix present in two varieties: infectious/inflammatory and neoplastic etiologies. The latter can present in the form of epithelial, neuroendocrine tumors (NETs), lymphoma, mesenchymal tumors, sarcomas, and metastases.[1] Most neoplastic causes are epithelial tumors and NETs, with the former occurring in middle-aged or older adults and the latter occurring in younger patients.[2] Though neoplastic processes of the appendix are typically asymptomatic, they can grow to cause obstruction, eventually resulting in symptoms of acute appendicitis.[3] They can also produce vague pain symptoms in the right lower quadrant (RLQ) or a palpable mass. In severe cases, especially with mucinous neoplasms, they can cause pseudomyxoma peritoneii, which characteristically presents as mucin in the peritoneum and serosa of abdominal or pelvic organs.[4]
Acute appendicitis is a prevalent cause of abdominal pain, with an estimated lifetime risk of 7 to 9%.[5] It classically presents with periumbilical pain that localizes to the right lower quadrant and nausea, vomiting, anorexia, and fever. The right lower quadrant pain is typically located half the distance between the umbilicus and anterior superior iliac spine (ASIS), known as McBurney’s point.[6] Acute appendicitis may result from an obstructing fecalith or another typically mechanical obstruction. A feared complication of acute appendicitis is perforation, with a risk of 2% at 36 hours, increasing by 5% every 12 hours.[7] With worsening inflammation, patients can develop more intense tenderness to palpation and guarding. Given the complications of acute appendicitis, an early, accurate diagnosis is crucial.[8][9][10]
Anatomy
Register For Free And Read The Full Article
Search engine and full access to all medical articles
10 free questions in your specialty
Free CME/CE Activities
Free daily question in your email
Save favorite articles to your dashboard
Emails offering discounts
Learn more about a Subscription to StatPearls Point-of-Care
Anatomy
The vermiform appendix is a vestigial organ located at the terminal end of the cecum.[11] Grossly, a reliable landmark for determining the base is the convergence of the taeniae coli. It is a true diverticulum in that it shares all of the same layers as the colon: mucosa, submucosa, longitudinal and circular muscularis, and serosa. It also contains scattered B and T lymphoid cells in the mucosa and submucosa, which differentiates it from the colonic tissue from which it originates.[12]
While the location of the base of the appendix is reliable, its tail is variable in positioning. [10] The tail is most commonly retrocecal but can be subcecal, pre-ileal, post-ileal, and pelvic.[10] Its position can change with variables such as respiration, overlying bowel gas, and patient position.[11] Given the differing positions of the appendiceal tail, not all presentations for acute appendicitis will be similar. The appendix is, on average, 8 to 10 cm in length and 7 mm in diameter, with the wall thickness typically 2 mm.[13] Diameter and wall thickness are essential indicators of inflammation where a diameter over 7 mm (over 6 mm in some locations) and a wall thickness greater than 2 to 3 mm are criteria for acute appendicitis when imaging in most situations.[10]
Plain Films
Of all imaging modalities, radiographs have little clinical utility in imaging the appendix. If there is a concern for acute appendicitis, radiographs may rarely demonstrate a calcified fecalith, which is visible in cases of appendicitis; however, this is not a specific finding.[14] Another potential finding on radiographs seen with complicated appendicitis can be pneumoperitoneum; however, this rarely occurs, even with rupture.[15] Overall, the use of abdominal radiographs on a patient with acute abdominal pain typically has poor sensitivity and specificity for diagnosing acute appendicitis, though the identification of obstruction or free air would aid in diagnosing other urgent or emergent conditions.[16]
Computed Tomography
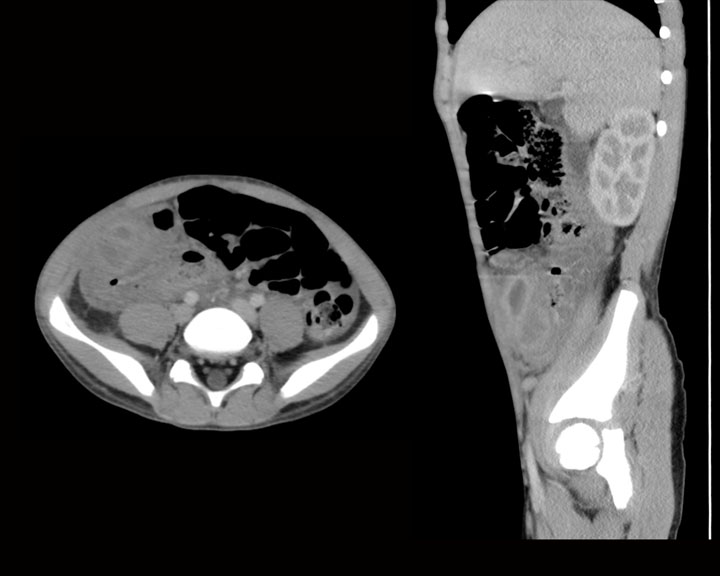
Computed tomography (CT) is one of the primary diagnostic modalities for identifying the appendix and diagnosing any disease present. Diagnosing appendicitis on CT has a sensitivity and specificity of 87% and 76%, respectively.[17] Oral and rectal contrast-enhanced CT imaging most often provides no additional diagnostic benefit; therefore, an intravenous contrast-enhanced CT is the recommended procedure for appropriate diagnosis. Classically, diagnosis of acute appendicitis is by identifying an enlarged appendix (greater than 6 mm in diameter) with wall thickening over 2 or 3 mm, wall enhancement, and surrounding inflammation evidenced by periappendiceal fat stranding or free fluid.[18] The presence of an obstructing fecalith may also be present though its absence does not preclude the diagnosis.
There has been a debate about the exact criteria for diagnosis; however, as some recent studies argue, a criteria cutoff of greater than 6 mm diameter is too small and leads to negative appendectomies.[19] While 6 mm may be a suitable cut-off for pediatric patients, many adult patients have normal appendix diameters between 6 to 7 mm. Therefore, some studies suggest using a cut-off value of over 7 mm to improve the prognostic capability of CT.[19]
For the diagnosis of neoplasms, CT has a sensitivity of 95% in symptomatic patients.[20] IV contrast, as well as oral contrast, can be beneficial for the identification and staging of tumors. The diagnostic criterion is an enlarged appendix greater than 15 mm in diameter, characteristics of cystic dilatation, or a soft tissue mass.[8] There may be mucoceles that can vary in size due to the underlying cause: mucoceles less than 2 cm are likely from luminal obstruction, whereas neoplasms typically cause larger mucoceles.[21] It will appear as a dilated appendix with homogenous low-attenuating material, with or without irregular and nodular wall thickening. Other neoplasms may demonstrate a soft-tissue mass, periappendiceal fat stranding, invasion of adjacent structures, or lymphadenopathy. Specifically, if a NET is suspected, one would look for a very small (less than 1 or 2 cm) submucosal mass in the distal appendix, which enhances significantly with or without calcifications.[22] However, NETs can be too small to be seen on imaging.[23][19]
Magnetic Resonance
Magnetic resonance imaging (MRI) has recently increased in use for the pregnant and pediatric populations due to the lack of ionizing radiation. It has a sensitivity of 96% and specificity of 96% in evaluating for appendicitis, though it has been shown to be slightly more effective in identifying the appendix in adults versus children.[24] The study is typically performed without contrast though there is variability in imaging protocols at different facilities. The criteria for appendicitis include the visualization of the enlarged appendix (over 7 mm diameter), wall thickening over 2 mm, peri-appendiceal fat stranding, fluid-filled appendix, or free fluid. These are consistent imaging criteria throughout the different modalities.
Another primary use for MRI is in staging appendiceal neoplasms, as it is more accurate than CT. The accuracy increases by adding diffusion-weighted imaging (DWI), which helps identify highly cellular tumor implants. Solid tumors will demonstrate restricted diffusion, delineating them from the adjacent organs. When included with delayed gadolinium-enhanced imaging with oral and rectal contrast, the sensitivity is 95% and specificity 70%.[23][8]
Ultrasonography
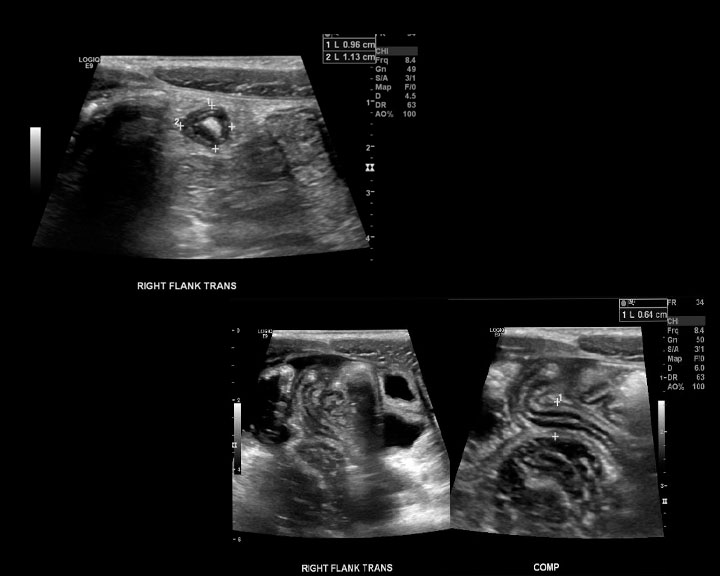
Ultrasound (US) has similar indications to MRI, though it remains useful in children who have thinner musculature and less abdominal fat. It has a sensitivity of 55% and a specificity of 95% for diagnosing acute appendicitis.[25] It is highly operator dependent, however, and therefore an equivocal or negative study cannot rule out appendicitis.
The exam employs graded compression and evaluates several factors: diameter (over 6 mm), surrounding peri-caecal fat, peri-appendiceal inflammation, free fluid, presence of reactive lymph nodes, and mural hyperplasia.[26] Surrounding inflammation is often the most reliable sign of appendicitis on US imaging, and the lack of its presence is a reliable indicator to rule it out.
A common mimic of appendicitis on sonographic imaging is lymphoid hyperplasia, a benign condition causing enlargement of the appendiceal diameter, specifically in the lamina propria.[27] The lamina propria can be seen as a hypoechoic innermost layer of the appendix. Thickening by more than 0.8 mm is diagnostic of lymphoid hyperplasia, even in the setting of an overall enlarged appendix.[28] This condition is non-operative and typically associated with inflammatory diseases such as viral enteritis.
When investigating for neoplasm, mucoceles may also be visible on ultrasound. They appear as an ovoid cystic mass with variable echogenicity. Typically they will have concentric echogenic layers (“onion skin”), acoustic shadowing from mural calcifications, and the appendix will be pear-shaped. They can also demonstrate regional adenopathy, fat stranding, and free fluid.[9][23][29]
Clinical Significance
Imaging of the appendix is most commonly performed to investigate acute appendicitis. The use of imaging for appendiceal neoplasms, though less commonly done, does have high sensitivity and specificity. If the patient has symptoms, the accuracy is improved further as neoplasms can sometimes produce symptoms of acute appendicitis (which is most common), generalized abdominal pain, palpable mass, obstruction, or distension. Imaging studies can be used to diagnose the tumor, and they can also be used to stage the tumor in the classic TNM staging system. The staging typically takes place via MRI. These studies more often identify epithelial tumors, and the diagnosis of NETs is uncommon due to their relatively small size and nonaggressive behavior. Overall, the definitive diagnosis of neoplasms requires pathologic examination after appendectomy.
On the other hand, appendicitis is regularly diagnosed using radiology studies. In fact, imaging is often the deciding factor between operative and non-operative management. Though the diagnosis can be clinical following a thorough history and physical, imaging is regularly employed to confirm the diagnosis in question. The most commonly used radiographic study is the CT scan, given its speed, sensitivity, and specificity. Though MRI and US are also relatively useful modalities to diagnose acute appendicitis, they have their limitations. Ultrasound is highly operator dependent and tends to work best on individuals with less fat and muscle content in their abdomen (i.e., children). MRI is not always readily available, especially in smaller hospitals or rural settings. It is also a more prolonged study, and it may be more difficult for patients to be still while they are in acute pain, especially children. Currently, the negative appendectomy is less than 12% in men but can be up to 33% in women; accurate imaging studies could reduce the number of unnecessary surgeries performed on patients.[30] It is, therefore, essential to know which study will provide the clinician with the most accurate information for their specific clinical scenario.[8][19]
Media
(Click Image to Enlarge)
(Click Image to Enlarge)
(Click Image to Enlarge)
(Click Image to Enlarge)
References
Tang LH. Epithelial neoplasms of the appendix. Archives of pathology & laboratory medicine. 2010 Nov:134(11):1612-20 [PubMed PMID: 21043814]
Wu H, Chintagumpala M, Hicks J, Nuchtern JG, Okcu MF, Venkatramani R. Neuroendocrine Tumor of the Appendix in Children. Journal of pediatric hematology/oncology. 2017 Mar:39(2):97-102. doi: 10.1097/MPH.0000000000000598. Epub [PubMed PMID: 27306228]
Komo T, Kohashi T, Hihara J, Oishi K, Yoshimitsu M, Kanou M, Nakashima A, Aoki Y, Miguchi M, Kaneko M, Mukaida H, Hirabayashi N. Intestinal obstruction caused by low-grade appendiceal mucinous neoplasm: A case report and review of the literature. International journal of surgery case reports. 2018:51():37-40. doi: 10.1016/j.ijscr.2018.08.001. Epub 2018 Aug 9 [PubMed PMID: 30138868]
Level 3 (low-level) evidenceRizvi SA, Syed W, Shergill R. Approach to pseudomyxoma peritonei. World journal of gastrointestinal surgery. 2018 Aug 27:10(5):49-56. doi: 10.4240/wjgs.v10.i5.49. Epub [PubMed PMID: 30190782]
Humes D, Speake WJ, Simpson J. Appendicitis. BMJ clinical evidence. 2007 Jul 1:2007():. pii: 0408. Epub 2007 Jul 1 [PubMed PMID: 19454096]
Level 1 (high-level) evidenceGrover CA, Sternbach G. Charles McBurney: McBurney's point. The Journal of emergency medicine. 2012 May:42(5):578-81. doi: 10.1016/j.jemermed.2011.06.039. Epub 2011 Oct 5 [PubMed PMID: 21982626]
Bickell NA, Aufses AH Jr, Rojas M, Bodian C. How time affects the risk of rupture in appendicitis. Journal of the American College of Surgeons. 2006 Mar:202(3):401-6 [PubMed PMID: 16500243]
Level 2 (mid-level) evidenceLeonards LM, Pahwa A, Patel MK, Petersen J, Nguyen MJ, Jude CM. Neoplasms of the Appendix: Pictorial Review with Clinical and Pathologic Correlation. Radiographics : a review publication of the Radiological Society of North America, Inc. 2017 Jul-Aug:37(4):1059-1083. doi: 10.1148/rg.2017160150. Epub 2017 Jun 9 [PubMed PMID: 28598731]
Bhangu A, Søreide K, Di Saverio S, Assarsson JH, Drake FT. Acute appendicitis: modern understanding of pathogenesis, diagnosis, and management. Lancet (London, England). 2015 Sep 26:386(10000):1278-1287. doi: 10.1016/S0140-6736(15)00275-5. Epub [PubMed PMID: 26460662]
Level 3 (low-level) evidenceJones MW, Lopez RA, Deppen JG. Appendicitis. StatPearls. 2024 Jan:(): [PubMed PMID: 29630245]
Hodge BD, Kashyap S, Khorasani-Zadeh A. Anatomy, Abdomen and Pelvis: Appendix. StatPearls. 2023 Jan:(): [PubMed PMID: 29083761]
Mizumoto T. B and T cells in lymphoid tissues of human appendix. International archives of allergy and applied immunology. 1976:51(1):80-93 [PubMed PMID: 132409]
Willekens I, Peeters E, De Maeseneer M, de Mey J. The normal appendix on CT: does size matter? PloS one. 2014:9(5):e96476. doi: 10.1371/journal.pone.0096476. Epub 2014 May 6 [PubMed PMID: 24802879]
Level 2 (mid-level) evidenceUlukaya Durakbaşa C, Taşbaşi I, Tosyali AN, Mutus M, Sehiralti V, Zemheri E. An evaluation of individual plain abdominal radiography findings in pediatric appendicitis: results from a series of 424 children. Ulusal travma ve acil cerrahi dergisi = Turkish journal of trauma & emergency surgery : TJTES. 2006 Jan:12(1):51-8 [PubMed PMID: 16456751]
Campos Canelas AL, Fernandez HM, Crociati Meguins L, Silva Barros S, Crociati Meguins EM, Ishak G, Rodrigues De Moraes LA. Pneumoperitoneum in association with perforated appendicitis in a Brazilian Amazon woman. Case report. Il Giornale di chirurgia. 2010 Mar:31(3):80-2 [PubMed PMID: 20426916]
Level 3 (low-level) evidencevan Randen A, Laméris W, Luitse JS, Gorzeman M, Hesselink EJ, Dolmans DE, Peringa J, van Geloven AA, Bossuyt PM, Stoker J, Boermeester MA, OPTIMA study group. The role of plain radiographs in patients with acute abdominal pain at the ED. The American journal of emergency medicine. 2011 Jul:29(6):582-589.e2. doi: 10.1016/j.ajem.2009.12.020. Epub 2010 Apr 24 [PubMed PMID: 20825832]
Iamwat J, Teerasamit W, Apisarnthanarak P, Noppakunsomboon N, Kaewlai R. Predictive ability of CT findings in the differentiation of complicated and uncomplicated appendicitis: a retrospective investigation of 201 patients undergone appendectomy at initial admission. Insights into imaging. 2021 Oct 21:12(1):143. doi: 10.1186/s13244-021-01086-3. Epub 2021 Oct 21 [PubMed PMID: 34674054]
Level 2 (mid-level) evidencePark G, Lee SC, Choi BJ, Kim SJ. Stratified computed tomography findings improve diagnostic accuracy for appendicitis. World journal of gastroenterology. 2014 Oct 14:20(38):13942-9. doi: 10.3748/wjg.v20.i38.13942. Epub [PubMed PMID: 25320531]
Level 2 (mid-level) evidenceMoskowitz E, Khan AD, Cribari C, Schroeppel TJ. Size matters: Computed tomographic measurements of the appendix in emergency department scans. American journal of surgery. 2019 Aug:218(2):271-274. doi: 10.1016/j.amjsurg.2018.12.010. Epub 2018 Dec 11 [PubMed PMID: 30558802]
Pickhardt PJ, Levy AD, Rohrmann CA Jr, Kende AI. Primary neoplasms of the appendix manifesting as acute appendicitis: CT findings with pathologic comparison. Radiology. 2002 Sep:224(3):775-81 [PubMed PMID: 12202713]
Level 2 (mid-level) evidenceSpyropoulos C, Rentis A, Alexaki E, Triantafillidis JK, Vagianos C. Appendiceal mucocele and pseudomyxoma peritonei; the clinical boundaries of a subtle disease. The American journal of case reports. 2014 Aug 27:15():355-60. doi: 10.12659/AJCR.890837. Epub 2014 Aug 27 [PubMed PMID: 25163976]
Level 3 (low-level) evidenceBayhan Z, Yildiz YA, Akdeniz Y, Gonullu E, Altintoprak F, Mantoglu B, Capoglu R, Kahyaoglu Akkaya Z. Appendix Neuroendocrine Tumor: Retrospective Analysis of 4026 Appendectomy Patients in a Single Center. Emergency medicine international. 2020:2020():4030527. doi: 10.1155/2020/4030527. Epub 2020 Sep 3 [PubMed PMID: 32963833]
Level 2 (mid-level) evidenceKim DW, Suh CH, Yoon HM, Kim JR, Jung AY, Lee JS, Cho YA. Visibility of Normal Appendix on CT, MRI, and Sonography: A Systematic Review and Meta-Analysis. AJR. American journal of roentgenology. 2018 Sep:211(3):W140-W150. doi: 10.2214/AJR.17.19321. Epub 2018 Jul 24 [PubMed PMID: 30040469]
Level 1 (high-level) evidenceDuke E, Kalb B, Arif-Tiwari H, Daye ZJ, Gilbertson-Dahdal D, Keim SM, Martin DR. A Systematic Review and Meta-Analysis of Diagnostic Performance of MRI for Evaluation of Acute Appendicitis. AJR. American journal of roentgenology. 2016 Mar:206(3):508-17. doi: 10.2214/AJR.15.14544. Epub [PubMed PMID: 26901006]
Level 1 (high-level) evidenceFranke C, Böhner H, Yang Q, Ohmann C, Röher HD. Ultrasonography for diagnosis of acute appendicitis: results of a prospective multicenter trial. Acute Abdominal Pain Study Group. World journal of surgery. 1999 Feb:23(2):141-6 [PubMed PMID: 9880422]
Level 1 (high-level) evidencePacharn P, Ying J, Linam LE, Brody AS, Babcock DS. Sonography in the evaluation of acute appendicitis: are negative sonographic findings good enough? Journal of ultrasound in medicine : official journal of the American Institute of Ultrasound in Medicine. 2010 Dec:29(12):1749-55 [PubMed PMID: 21098847]
Level 2 (mid-level) evidenceXu Y, Jeffrey RB, DiMaio MA, Olcott EW. Lymphoid Hyperplasia of the Appendix: A Potential Pitfall in the Sonographic Diagnosis of Appendicitis. AJR. American journal of roentgenology. 2016 Jan:206(1):189-94. doi: 10.2214/AJR.15.14846. Epub [PubMed PMID: 26700351]
Kwon LM, Lee K, Min SK, Ahn SM, Ha HI, Kim MJ. Ultrasound features of secondary appendicitis in pediatric patients. Ultrasonography (Seoul, Korea). 2018 Jul:37(3):233-243. doi: 10.14366/usg.17029. Epub 2017 Aug 25 [PubMed PMID: 29141286]
Sanchez TR, Corwin MT, Davoodian A, Stein-Wexler R. Sonography of Abdominal Pain in Children: Appendicitis and Its Common Mimics. Journal of ultrasound in medicine : official journal of the American Institute of Ultrasound in Medicine. 2016 Mar:35(3):627-35. doi: 10.7863/ultra.15.04047. Epub 2016 Feb 18 [PubMed PMID: 26892821]
Joshi MK, Joshi R, Alam SE, Agarwal S, Kumar S. Negative Appendectomy: an Audit of Resident-Performed Surgery. How Can Its Incidence Be Minimized? The Indian journal of surgery. 2015 Dec:77(Suppl 3):913-7. doi: 10.1007/s12262-014-1063-0. Epub 2014 Apr 9 [PubMed PMID: 27011482]